Pharmacokinetics and safety of fluconazole and micafungin in neonates with systemic candidiasis: a randomized, open-label clinical trial
- PMID: 29744900
- PMCID: PMC6089805
- DOI: 10.1111/bcp.13628
Pharmacokinetics and safety of fluconazole and micafungin in neonates with systemic candidiasis: a randomized, open-label clinical trial
Abstract
Aims: The pharmacokinetics (PK) of fluconazole and micafungin differ in neonates compared with children and adults. Dosing instructions in product labels appear to be inconsistent with the emerging scientific evidence. Limited information is available on the safety profile of these agents in neonates. Our objective was to study the population PK and safety of both drugs, randomly administered in neonates with suspected or confirmed systemic candidiasis.
Methods: Neonates were randomized 1:1 to fluconazole (loading dose 25 mg kg-1 ; maintenance dose 12 mg kg-1 day-1 or 20 mg kg-1 day-1 , respectively, for infants <30 weeks or ≥30 weeks' corrected gestational age) or micafungin (loading dose 15 mg kg-1 day-1 ; maintenance dose 10 mg kg-1 day-1 ). PK samples were taken on treatment days 1 and 5. Population parameters were determined using NONMEM and Monte Carlo simulations performed to reach predefined targets. Clinical and laboratory data, and adverse events were collected up to 36 weeks' corrected gestational age or hospital discharge.
Results: Thirty-six neonates were enrolled. The median (range) gestational age was 28.2 (24.1-40.1) and 26.8 (23.5-40.0) weeks for fluconazole and micafungin, respectively. Based on 163 PK samples, the median population clearance (l h-1 kg-1 ) and volume of distribution (l kg-1 ) for fluconazole were: 0.015 [95% confidence interval (CI) 0.008, 0.039] and 0.913, and for micafungin were: 0.020 (95% CI 0.010, 0.023) and 0.354 (95% CI 0.225, 0.482), respectively. The loading dose was well tolerated. No adverse events associated with micafungin or fluconazole were reported.
Conclusion: Based on Monte Carlo simulations, a loading dose for fluconazole and dosing higher than recommended for both drugs are required to increase the area under the plasma drug concentration-time curve target attainment rate in neonates.
Keywords: Candida spp; fluconazole; micafungin; neonate; pharmacokinetics; safety.
© 2018 The British Pharmacological Society.
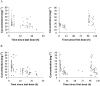
Figures


Similar articles
-
Fluconazole loading dose pharmacokinetics and safety in infants.Pediatr Infect Dis J. 2011 May;30(5):375-8. doi: 10.1097/INF.0b013e318202cbb3. Pediatr Infect Dis J. 2011. PMID: 21085048 Free PMC article.
-
Population pharmacokinetics of fluconazole in young infants.Antimicrob Agents Chemother. 2008 Nov;52(11):4043-9. doi: 10.1128/AAC.00569-08. Epub 2008 Sep 22. Antimicrob Agents Chemother. 2008. PMID: 18809946 Free PMC article.
-
Pharmacokinetics and Safety of Micafungin in Infants Supported With Extracorporeal Membrane Oxygenation.Pediatr Infect Dis J. 2016 Nov;35(11):1204-1210. doi: 10.1097/INF.0000000000001268. Pediatr Infect Dis J. 2016. PMID: 27314826 Free PMC article.
-
Clinical Pharmacokinetics and Pharmacodynamics of Micafungin.Clin Pharmacokinet. 2018 Mar;57(3):267-286. doi: 10.1007/s40262-017-0578-5. Clin Pharmacokinet. 2018. PMID: 28791666 Free PMC article. Review.
-
[Why might micafungin be the drug of choice in pediatric patients?].Enferm Infecc Microbiol Clin. 2011 Mar;29 Suppl 2:23-8. doi: 10.1016/S0213-005X(11)70005-2. Enferm Infecc Microbiol Clin. 2011. PMID: 21420573 Review. Spanish.
Cited by
-
Pharmacokinetics Alterations in Critically Ill Pediatric Patients on Extracorporeal Membrane Oxygenation: A Systematic Review.Front Pediatr. 2020 Jun 26;8:260. doi: 10.3389/fped.2020.00260. eCollection 2020. Front Pediatr. 2020. PMID: 32670992 Free PMC article.
-
Fluconazole Population Pharmacokinetics after Fosfluconazole Administration and Dosing Optimization in Extremely Low-Birth-Weight Infants.Microbiol Spectr. 2022 Apr 27;10(2):e0195221. doi: 10.1128/spectrum.01952-21. Epub 2022 Mar 10. Microbiol Spectr. 2022. PMID: 35266811 Free PMC article.
-
Perspectives on the Use of Echinocandins in the Neonatal Intensive Care Unit.Antibiotics (Basel). 2024 Dec 12;13(12):1209. doi: 10.3390/antibiotics13121209. Antibiotics (Basel). 2024. PMID: 39766599 Free PMC article. Review.
-
The Blind Spot of Pharmacology: A Scoping Review of Drug Metabolism in Prematurely Born Children.Front Pharmacol. 2022 Feb 15;13:828010. doi: 10.3389/fphar.2022.828010. eCollection 2022. Front Pharmacol. 2022. PMID: 35242037 Free PMC article.
-
Evaluation of Population Pharmacokinetic Models of Micafungin: Implications for Dosing Regimen Optimization in Critically Ill Patients.Pharmaceutics. 2024 Aug 29;16(9):1145. doi: 10.3390/pharmaceutics16091145. Pharmaceutics. 2024. PMID: 39339182 Free PMC article. Review.
References
-
- Oeser C, Vergnano S, Naidoo R, Anthony M, Chang J, Chow P, et al Neonatal invasive fungal infection in England 2004–2010. Clin Microbiol Infect 2014; 20: 936–941. - PubMed
-
- Benjamin DK, Poole C, Steinbach WJ, Rowen JL, Walsh TJ. Neonatal candidemia and end‐organ damage: a critical appraisal of the literature using meta‐analytic techniques. Pediatrics 2003; 112: 634–640. - PubMed
-
- Benjamin DK, Stoll BJ, Fanaroff AA, McDonald SA, Oh W, Higgins RD, et al National Institute of Child Health and Human Development Neonatal Research Network. Neonatal candidiasis among extremely low birth weight infants: risk factors, mortality rates, and neurodevelopmental outcomes at 18 to 22 months. Pediatrics 2006; 117: 84–92. - PubMed
Publication types
MeSH terms
Substances
Supplementary concepts
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical
Miscellaneous

