Prenatal non-invasive foetal RHD genotyping: diagnostic accuracy of a test as a guide for appropriate administration of antenatal anti-D immunoprophylaxis
- PMID: 29757138
- PMCID: PMC6214827
- DOI: 10.2450/2018.0270-17
Prenatal non-invasive foetal RHD genotyping: diagnostic accuracy of a test as a guide for appropriate administration of antenatal anti-D immunoprophylaxis
Abstract
Background: Foetal RHD genotyping can be predicted by real-time polymerase chain reaction (qPCR) using cell-free foetal DNA extracted from maternal plasma. The object of this study was to determine the diagnostic accuracy and feasibility of non-invasive RHD foetal genotyping, using a commercial multiple-exon assay, as a guide to appropriate administration of targeted antenatal immunoprophylaxis.
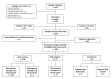
Material and methods: Cell-free foetal DNA was extracted from plasma of RhD-negative women between 11-30 weeks of pregnancy. The foetal RHD genotype was determined non-invasively by qPCR amplification of exons 5, 7 and 10 of the RHD gene using the Free DNA Fetal Kit® RhD. Results were compared with serological RhD cord blood typing at birth. The analysis of diagnostic accuracy was restricted to the period (24-28+6 weeks) during which foetal genotyping is usually performed for targeted antenatal immunoprophylaxis.
Results: RHD foetal genotyping was performed on 367 plasma samples (24-28+6 weeks). Neonatal RhD phenotype results were available for 284 pregnancies. Foetal RHD status was inconclusive in 9/284 (3.2%) samples, including four cases with RhD maternal variants. Two false-positive results were registered. The sensitivity was 100% and the specificity was 97.5% (95% CI: 94.0-100). The diagnostic accuracy was 99.3% (95% CI: 98.3-100), decreasing to 96.1% (95% CI: 93.9-98.4) when the inconclusive results were included. The negative and positive predictive values were 100% (95% CI: 100-100) and 99.0% (95% CI: 97.6-100), respectively. There was one false-negative result in a sample collected at 18 weeks. After inclusion of samples at early gestational age (<23+6 week), sensitivity and accuracy were 99.6% (95% CI: 98.7-100) and 95.5% (95% CI: 93.3-97.8), respectively.
Discussion: This study demonstrates that foetal RHD detection on maternal plasma using a commercial multiple-exon assay is a reliable and accurate tool to predict foetal RhD phenotype. It can be a safe guide for the appropriate administration of targeted prenatal immunoprophylaxis.
Conflict of interest statement
The Authors declare no conflicts of interest.
Figures
References
-
- de Haas M, Thurik FF, Koelewijn JM, van der Schoot CE. Haemolytic disease of the fetus and newborn. Vox Sang. 2015;109:99–113. - PubMed
-
- Urbaniak SJ, Greiss MA. RhD haemolytic disease of the fetus and the newborn. Blood Rev. 2000;14:44–61. - PubMed
-
- Crowther CA, Keirse MJ. Anti-D administration in pregnancy for preventing Rhesus alloimmunisation. Cochrane Database Syst Rev. 2000;2:CD000020. - PubMed
-
- de Haas M, Finning K, Massey E, Roberts DJ. Anti-D prophylaxis: past, present and future. Transfus Med. 2014;24:1–7. - PubMed
Publication types
MeSH terms
Substances
LinkOut - more resources
Full Text Sources
Medical