Efficacy and safety of photodynamic therapy for cervical intraepithelial neoplasia and human papilloma virus infection: A systematic review and meta-analysis of randomized clinical trials
- PMID: 29794788
- PMCID: PMC6392907
- DOI: 10.1097/MD.0000000000010864
Efficacy and safety of photodynamic therapy for cervical intraepithelial neoplasia and human papilloma virus infection: A systematic review and meta-analysis of randomized clinical trials
Abstract
Background: We sought to conduct a systemic review and meta-analysis of randomized clinical trials to assess the efficacy and safety of photodynamic therapy (PDT) in cervical intraepithelial neoplasia (CIN) and cervical human papilloma virus (HPV) infection.
Methods: The Medline, EMBASE, and Cochrane Central Register databases were searched using relevant keywords for entries up to May 1, 2017, irrespective of year of publication. The language was restricted to English. Randomized clinical trials and qualitative studies comparing PDT and placebo for CIN or HPV-positive patients were included. We assessed the evidence quality using a risk of bias graph in RevMan V5.3 and the Grading of Recommendations Assessment, Development, and Evaluation scoring system.
Results: Of the 168 studies identified, only 4 RCTs met the inclusion criteria for meta-analysis. In all, 292 and 141 patients received PDT or placebo, respectively. PDT significantly increased the complete remission rate (CRR) among those with CIN (odds ratio [OR]: 2.51 [1.23-5.12]; P = .01) and HPV infection (OR: 3.82 [1.91-7.65]; P = .0002). The adverse events rate (AER) for PDT was greater than that for placebo (OR: 13.32 [4.44, 40.02]; P < .00001). The overall evidence quality was very low. Similarly, in a systematic review including 21 qualitative records, the CRRs for CIN patients with PDT and cervical HPV infection patients with PDT were 82.0% and 77.5%, respectively. The AER for PDT was 31.6%, which was lower than that observed in our meta-analysis (74.6%).
Conclusions: PDT that targets CIN or cervical HPV infection improves the CRR, but slightly compromises safety. Further studies are necessary to identify the most effective and least toxic photosensitizer.
Conflict of interest statement
The authors declare no conflicts of interest.
Figures



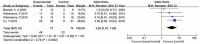

Similar articles
-
Prophylactic vaccination against human papillomaviruses to prevent cervical cancer and its precursors.Cochrane Database Syst Rev. 2018 May 9;5(5):CD009069. doi: 10.1002/14651858.CD009069.pub3. Cochrane Database Syst Rev. 2018. PMID: 29740819 Free PMC article.
-
Efficacy of photodynamic therapy in women with HSIL, LSIL and early stage squamous cervical cancer: a systematic review and meta-analysis.Photodiagnosis Photodyn Ther. 2021 Dec;36:102530. doi: 10.1016/j.pdpdt.2021.102530. Epub 2021 Sep 14. Photodiagnosis Photodyn Ther. 2021. PMID: 34534688
-
Non-steroidal anti-inflammatory agents to induce regression and prevent the progression of cervical intraepithelial neoplasia.Cochrane Database Syst Rev. 2018 Feb 12;2(2):CD004121. doi: 10.1002/14651858.CD004121.pub4. Cochrane Database Syst Rev. 2018. PMID: 29431861 Free PMC article.
-
Efficacy and safety of photodynamic therapy for cervical intraepithelial neoplasia: a systemic review.Photodiagnosis Photodyn Ther. 2014 Jun;11(2):104-12. doi: 10.1016/j.pdpdt.2014.02.012. Epub 2014 Mar 12. Photodiagnosis Photodyn Ther. 2014. PMID: 24631593
-
Efficacy of ALA-PDT in treating cervical low-grade squamous intraepithelial lesions with high-risk HPV patients: A multicentre randomized controlled trial.Int J Cancer. 2025 Sep 1;157(5):908-915. doi: 10.1002/ijc.35450. Epub 2025 Apr 23. Int J Cancer. 2025. PMID: 40268556 Clinical Trial.
Cited by
-
The role of photodynamic therapy in treating LSIL in women with high-risk HPV: a literature review.Lasers Med Sci. 2025 May 22;40(1):237. doi: 10.1007/s10103-025-04480-1. Lasers Med Sci. 2025. PMID: 40402167 Review.
-
Long Term Effectiveness of Photodynamic Therapy for CIN Treatment.Pharmaceuticals (Basel). 2019 Jul 12;12(3):107. doi: 10.3390/ph12030107. Pharmaceuticals (Basel). 2019. PMID: 31336848 Free PMC article.
-
Phototheranostics of Cervical Neoplasms with Chlorin e6 Photosensitizer.Cancers (Basel). 2022 Jan 2;14(1):211. doi: 10.3390/cancers14010211. Cancers (Basel). 2022. PMID: 35008375 Free PMC article.
-
The efficacy and safety of local 5-aminolevulinic acid-based photodynamic therapy in the treatment of cervical high-grade squamous intraepithelial lesion: a single center retrospective observational study.Front Oncol. 2024 Apr 16;14:1390982. doi: 10.3389/fonc.2024.1390982. eCollection 2024. Front Oncol. 2024. PMID: 38694787 Free PMC article.
-
Clearance of human papillomavirus infection in patients with cervical intraepithelial neoplasia: A systemic review and meta-analysis.Medicine (Baltimore). 2020 Nov 13;99(46):e23155. doi: 10.1097/MD.0000000000023155. Medicine (Baltimore). 2020. PMID: 33181688 Free PMC article.
References
-
- Siegel RL, Miller KD, Jemal A. Cancer statistics, 2016. CA Cancer J Clin 2016;66:7–30. - PubMed
-
- Lowy D. Human papillomavirus, cervical cancer prevention, and more. Vaccine 2008;26(Suppl 10):iii–v. - PubMed
-
- Trushina OI, Novikova EG, Sokolov VV, et al. Photodynamic therapy of virus-associated precancer and early stages cancer of cervix uteri. Photodiagnosis Photodyn Ther 2008;5:256–9. - PubMed
-
- Bosch FX, Sanjose SD, Castellsagué X. Epidemiology of genitoanal HPV infections and associated cancer. 2011;Berlin Heidelberg: Springer, 427–439.
Publication types
MeSH terms
Substances
LinkOut - more resources
Full Text Sources
Other Literature Sources
Miscellaneous

