Peritoneal carcinomatosis index as a predictor of diaphragmatic involvement in stage III and IV ovarian cancer
- PMID: 29844678
- PMCID: PMC5961326
- DOI: 10.2147/OTT.S147559
Peritoneal carcinomatosis index as a predictor of diaphragmatic involvement in stage III and IV ovarian cancer
Abstract
Objective: To analyze the surgical outcomes and diaphragmatic involvement in stage III and IV ovarian cancer.
Patients and methods: All patients with stage III-IV ovarian cancer between January 2013 and January 2016 were included. The outcomes of interest reviewed were as follows: surgical (complications, mortality), peritoneal carcinomatosis index (PCI), rate of complete resection, and disease-free interval and survival.
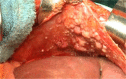
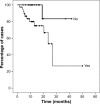
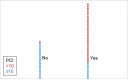
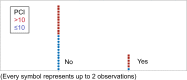
Results: Fifty-seven patients were included, 38 (67%) with diaphragmatic involvement; in 10 cases (18%), diaphragmatic resection was required. Optimal cytoreduction (OCR) was obtained in 49 cases (86%). The PCI was >10 in 31 cases (54%). Respiratory complications occurred in 10 cases (18%) and mortality in 3 (5%). Disease-free survival rate in 3 years was 53%, being 87% in cases without diaphragmatic involvement. The overall survival rate in 3 years is 46%, 83% in the cases without diaphragmatic involvement and 27% in cases with affectation (p<0.05). In cases of OCR, 3 year survival rate was 65%. In the multivariate analysis for the overall survival of cases with OCR, the only independent prognostic factor found was the operative PCI. A strong correlation was found between the total PCI and the diaphragmatic PCI (p<0.001). With a PCI >10, virtually all cases will present diaphragmatic involvement (p<0.05).
Conclusion: The tumor burden is different in stages III and IV of advanced ovarian cancer and the PCI is an effective method to quantify it. The PCI constitutes an independent prognostic factor for the advanced stages of ovarian cancer. A PCI >10 constitutes a useful prognostic factor of the affectation and forces the surgeon to thoroughly review both diaphragms.
Keywords: advanced ovarian cancer; carcinomatosis; diaphragmatic involvement; peritoneal cancer index; upper abdominal surgery.
Conflict of interest statement
Disclosure The authors report no conflicts of interest in this work.
Figures

References
-
- Abella Llueca JA, Martinez-Ramos D, Escrig-Sos J, et al. Current status of ovarian cancer in the Spanish Province of Castellon. Prognostic factors in observed and relative survival. A population cancer-registry-based study between 2004 and 2008. Prog Obstet Ginecol. 2014;57(9):405–412.
-
- du Bois A, Reuss A, Pujade-Lauraine E, Harter P, Ray-Coquard I, Pfisterer J. Role of surgical outcome as prognostic factor in advanced epithelial ovarian cancer: a combined exploratory analysis of 3 prospectively randomized phase 3 multicenter trials: by the Arbeitsgemeinschaft Gynaekologische Onkologie Studi-engruppe Ovarialkarzinom (AGO-OVAR) and the Groupe d’Investigateurs Nationaux Pour les Etudes des Cancers de l’Ovaire (GINECO) Cancer. 2009;115(6):1234–1244. - PubMed
-
- Bristow RE, Tomacruz RS, Armstrong DK, Trimble EL, Montz FJ. Survival effect of maximal cytoreductive surgery for advanced ovarian carcinoma during the platinum era: a meta-analysis. J Clin Oncol. 2002;20(5):1248–1259. - PubMed
-
- Kuhn W, Florack G, Roder J, et al. The influence of upper abdominal surgery on perioperative morbidity and mortality in patients with advanced ovarian cancer FIGO III and IV. Int J Gynecol Cancer. 1998;8(1):56–63.
-
- Serov SF, Scully RE, Sorbin LH. International Histological Classification of Tumors. Vol. 9. Geneva: World Health Organization; 1973. Histological typing of ovarian tumors; p. 17.
LinkOut - more resources
Full Text Sources
Other Literature Sources
Miscellaneous

