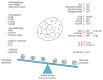
Neutrophils in Tissue Trauma of the Skin, Bone, and Lung: Two Sides of the Same Coin
- PMID: 29850639
- PMCID: PMC5937416
- DOI: 10.1155/2018/8173983
Neutrophils in Tissue Trauma of the Skin, Bone, and Lung: Two Sides of the Same Coin
Abstract
Following severe tissue injury, patients are exposed to various danger- and microbe-associated molecular patterns, which provoke a strong activation of the neutrophil defense system. Neutrophils trigger and modulate the initial posttraumatic inflammatory response and contribute critically to subsequent repair processes. However, severe trauma can affect central neutrophil functions, including circulation half-life, chemokinesis, phagocytosis, cytokine release, and respiratory burst. Alterations in neutrophil biology may contribute to trauma-associated complications, including immune suppression, sepsis, multiorgan dysfunction, and disturbed tissue regeneration. Furthermore, there is evidence that neutrophil actions depend on the quality of the initial stimulus, including trauma localization and severity, the micromilieu in the affected tissue, and the patient's overall inflammatory status. In the present review, we describe the effects of severe trauma on the neutrophil phenotype and dysfunction and the consequences for tissue repair. We particularly concentrate on the role of neutrophils in wound healing, lung injury, and bone fractures, because these are the most frequently affected tissues in severely injured patients.
Figures
References
-
- Terashima T., English D., Hogg J. C., van Eeden S. F. Release of polymorphonuclear leukocytes from the bone marrow by interleukin-8. Blood. 1998;92(3):1062–1069. - PubMed
Publication types
MeSH terms
Substances
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical
Molecular Biology Databases