Preoperative neutrophil-to-lymphocyte ratio predicts the surgical outcome of Xp11.2 translocation/TFE3 renal cell carcinoma patients
- PMID: 29890986
- PMCID: PMC5996532
- DOI: 10.1186/s12894-018-0374-z
Preoperative neutrophil-to-lymphocyte ratio predicts the surgical outcome of Xp11.2 translocation/TFE3 renal cell carcinoma patients
Abstract
Background: The preoperative neutrophil-to-lymphocyte ratio (NLR), C-reactive protein/albumin ratio (CRP/Alb ratio) and platelet-to-lymphocyte ratio (PLR) have been demonstrated to predict the clinical outcome of various human cancer, including renal cell carcinoma(RCC). The aim of our study was to explore the prognostic values of these ratios in patients with Xp11.2 translocation/TFE3 gene fusions renal cell carcinoma (Xp11.2 tRCC).
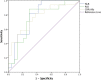
Methods: A retrospective multicentre study was performed in 82 Xp11.2 tRCC patients who underwent radical or partial nephrectomy. The optimal cutoff values of the NLR, CRP/Alb ratio and PLR were determined by the receiver operating characteristic (ROC) analysis. The impact of the NLR, CRP/Alb ratio and PLR, as well as other clinicopathological characteristics, on disease-free survival (DFS) and overall survival (OS) were evaluated using the univariate and multivariate Cox regression analyses.
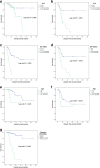
Results: The optimal cutoff values of the NLR, CRP/Alb ratio and PLR were set at 2.45, 140 and 0.08, respectively, according to the ROC analysis. Univariate analyses showed that the NLR, CRP/Alb ratio and PLR all were associated with DFS of Xp11.2 tRCC patients (P < 0.001, P = 0.005 and P = 0.001, respectively) and OS of Xp11.2 tRCC patients (P = 0.016, P = 0.003 and P = 0.014, respectively). Multivariate analysis indicated that the NLR was independently associated with DFS of Xp11.2 tRCC patients (hazard ratio [HR]: 4.25; 95% confidence interval [95% CI]: 1.19-15.18; P = 0.026) along with age (P = 0.004), the pT status (P < 0.001) and the pN status (P < 0.019), and the NLR (HR: 26.26; 95% CI: 1.44-480.3; P = 0.028) also was independently associated with OS in patients with Xp11.2 tRCC, along with age (P = 0.016) and a tumour thrombus (P = 0.007).
Conclusion: Overall, relatively high NLRs, CRP/Alb ratios and PLRs were associated with a poor prognosis of Xp11.2 tRCC patients; among of them, only the NLR independently predicted the progression of Xp11.2 tRCC, and the NLR may help to identify patients with high metastasis or relapse risk.
Keywords: C-reactive protein/albumin ratio; Neutrophil-to-lymphocyte ratio; Platelet-to-lymphocyte ratio; Renal cell carcinoma; Xp11.2 translocation.
Conflict of interest statement
Ethics approval and consent to participate
The study received the ethics approval from the Ethics Committee of Nanjing Drum Tower Hospital, Jiangsu Province Hospital, Jiangsu Cancer Hospital and Zhongda Hospital Southeast University.
All procedures performed in the study involving human participants were in accordance with the ethical standards of the institutional research committee and with the 1964 Helsinki declaration and its later amendments or comparable ethical standard.
All patients agreed and signed the informed consent to participate in the study, and they agreed that their information (including clinical information, surgical related data, pathological data, blood laboratory tests and surveillance) would be collected for scientific study and published in professional medical journals.
Competing interests
The authors declare that they have no competing interests.
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Figures
References
-
- Qu Y, Gu C, Wang H, Chang K, Yang X, Zhou X, Dai B, Zhu Y, Shi G, Zhang H, et al. Diagnosis of adults Xp11.2 translocation renal cell carcinoma by immunohistochemistry and FISH assays: clinicopathological data from ethnic Chinese population. Sci Rep. 2016;6:21677. doi: 10.1038/srep21677. - DOI - PMC - PubMed
-
- Sukov WR, Hodge JC, Lohse CM, Leibovich BC, Thompson RH, Pearce KE, Wiktor AE, Cheville JC. TFE3 rearrangements in adult renal cell carcinoma: clinical and pathologic features with outcome in a large series of consecutively treated patients. Am J Surg Pathol. 2012;36(5):663–670. - PubMed
-
- Choo MS, Jeong CW, Song C, Jeon HG, Seo SI, Hong SK, Byun SS, Chung JS, Hong SH, Hwang EC, et al. Clinicopathologic characteristics and prognosis of Xp11.2 translocation renal cell carcinoma: multicenter, propensity score matching analysis. Clin Genitourin Cancer. 2017;15(5):e819–e825. doi: 10.1016/j.clgc.2017.04.015. - DOI - PubMed
Publication types
MeSH terms
Substances
Grants and funding
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical
Research Materials
Miscellaneous

