Divergent effects of AKI to CKD models on inflammation and fibrosis
- PMID: 29897282
- PMCID: PMC6230746
- DOI: 10.1152/ajprenal.00179.2018
Divergent effects of AKI to CKD models on inflammation and fibrosis
Abstract
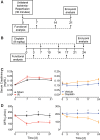
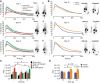
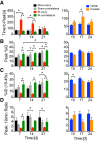
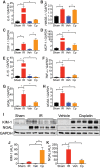
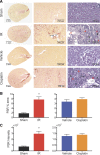
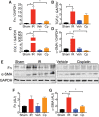
Chronic kidney disease (CKD) is a condition with significant morbidity and mortality that affects 15% of adults in the United States. One cause of CKD is acute kidney injury (AKI), which commonly occurs secondary to sepsis, ischemic events, and drug-induced nephrotoxicity. Unilateral ischemia-reperfusion injury (UIRI) without contralateral nephrectomy (CLN) and repeated low-dose cisplatin (RLDC) models of AKI to CKD demonstrate responses characteristic of the transition; however, previous studies have not effectively compared the pathogenesis. We demonstrate both models instigate renal dysfunction, inflammatory cytokine responses, and fibrosis. However, the models exhibit differences in urinary excretory function, inflammatory cell infiltration, and degree of fibrotic response. UIRI without CLN demonstrated worsening perfusion and function, measured with 99mTc-mercaptoacetyltriglycine-3 imaging, and physiologic compensation in the contralateral kidney. Furthermore, UIRI without CLN elicited a robust inflammatory response that was characterized by a prolonged polymorphonuclear cell and natural killer cell infiltrate and an early expansion of kidney resident macrophages, followed by T-cell infiltration. Symmetrical diminished function occurred in RLDC kidneys and progressively worsened until day 17 of the study. Surprisingly, RLDC mice demonstrated a decrease in inflammatory cell numbers relative to controls. However, RLDC kidneys expressed increased levels of kidney injury molecule-1 (KIM-1), high mobility group box-1 ( HMGB1), and colony stimulating factor-1 ( CSF-1), which likely recruits inflammatory cells in response to injury. These data emphasize how the divergent etiologies of AKI to CKD models affect the kidney microenvironment and outcomes. This study provides support for subtyping AKI by etiology in human studies, aiding in the elucidation of injury-specific pathophysiologic mechanisms of the AKI to CKD transition.
Keywords: chronic kidney disease; cisplatin; fibrosis; glomerular filtration rate; inflammation; ischemia-reperfusion.
Figures

References
-
- Basile DP, Friedrich JL, Spahic J, Knipe N, Mang H, Leonard EC, Changizi-Ashtiyani S, Bacallao RL, Molitoris BA, Sutton TA. Impaired endothelial proliferation and mesenchymal transition contribute to vascular rarefaction following acute kidney injury. Am J Physiol Renal Physiol 300: F721–F733, 2011. doi: 10.1152/ajprenal.00546.2010. - DOI - PMC - PubMed
Publication types
MeSH terms
Grants and funding
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical
Research Materials
Miscellaneous

