Higher dietary inflammation is associated with increased odds of depression independent of Framingham Risk Score in the National Health and Nutrition Examination Survey
- PMID: 29914664
- PMCID: PMC6011232
- DOI: 10.1016/j.nutres.2018.03.004
Higher dietary inflammation is associated with increased odds of depression independent of Framingham Risk Score in the National Health and Nutrition Examination Survey
Abstract
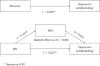
Cardiovascular disease (CVD) may increase depression risk. Risk for future CVD, which can be estimated by the Framingham Risk Score (FRS), and depression risk are both linked to systemic inflammation. Dietary consumption of proinflammatory food can be measured using the Dietary Inflammatory Index (DII) score. We examined the potential impact of DII on depression and whether this effect is independent of FRS. We hypothesized that (1) both FRS and DII would be associated with depression (Patient Health Questionnaire-9 ≥ 10) and (2) associations between DII and depressive symptoms (continuous) would be mediated by FRS. Data were included from adults without CVD who were participants of the 2007-2012 National Health and Nutrition Examination Survey (n = 11 624). Using logistic regression, we tested cross-sectional associations of FRS, DII (adjusting for FRS), and joint effects of FRS and DII with depression. Finally, using the Sobel method, we tested whether FRS mediates the relationship between DII and depressive symptoms. Individuals with FRS or DII scores in the top 2 quartiles had higher odds of depressive symptoms than those in the bottom quartile. The association of DII with depressive symptoms remained after FRS adjustment. The joint effects of elevated DII and FRS were additive. There was no evidence for mediation by FRS between DII and depressive symptoms. Thus, higher DII remained associated with increased odds of depressive symptoms net CVD risk. Collectively, the joint effects of CVD risk and DII indicate that a proinflammatory diet could add to risk for depressive symptoms even in those with a high FRS.
Keywords: Cardiovascular disease risk; Depression; Dietary inflammation; Systemic inflammation.
Copyright © 2018 Elsevier Inc. All rights reserved.
Conflict of interest statement
The authors have no conflicts of interest to disclose.
Figures

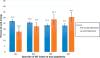
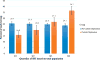

Similar articles
-
Inflammatory properties of diet mediate the effect of depressive symptoms on Framingham risk score in men and women: Results from the National Health and Nutrition Examination Survey (2007-2014).Nutr Res. 2020 Feb;74:78-86. doi: 10.1016/j.nutres.2019.11.008. Epub 2019 Nov 23. Nutr Res. 2020. PMID: 31958655
-
The Dietary Inflammatory Index, shift work, and depression: Results from NHANES.Health Psychol. 2017 Aug;36(8):760-769. doi: 10.1037/hea0000514. Epub 2017 May 29. Health Psychol. 2017. PMID: 28557499 Free PMC article.
-
The Inflammatory Potential of the Diet Is Associated with Depressive Symptoms in Different Subgroups of the General Population.J Nutr. 2017 May;147(5):879-887. doi: 10.3945/jn.116.245167. Epub 2017 Mar 29. J Nutr. 2017. PMID: 28356432 Free PMC article.
-
Dietary Inflammatory Index and Cardiovascular Risk and Mortality-A Meta-Analysis.Nutrients. 2018 Feb 12;10(2):200. doi: 10.3390/nu10020200. Nutrients. 2018. PMID: 29439509 Free PMC article. Review.
-
Dietary Inflammatory Index and Non-Communicable Disease Risk: A Narrative Review.Nutrients. 2019 Aug 12;11(8):1873. doi: 10.3390/nu11081873. Nutrients. 2019. PMID: 31408965 Free PMC article. Review.
Cited by
-
The higher dietary inflammation is associated with a higher burden of multimorbidity of cardio-metabolic and mental health disorders in an urbanizing community of southern India: A cross-sectional analysis for the APCAPS cohort.Hum Nutr Metab. 2024 Jun;36:None. doi: 10.1016/j.hnm.2024.200254. Hum Nutr Metab. 2024. PMID: 38828398 Free PMC article.
-
The interaction effects between depression and sleep status on asthma: a national cross-sectional study.Front Psychiatry. 2024 Oct 16;15:1487550. doi: 10.3389/fpsyt.2024.1487550. eCollection 2024. Front Psychiatry. 2024. PMID: 39479594 Free PMC article.
-
Construct Validation of the Dietary Inflammatory Index (DII) among Young College-Aged Women.Nutrients. 2023 Oct 27;15(21):4553. doi: 10.3390/nu15214553. Nutrients. 2023. PMID: 37960206 Free PMC article.
-
Examining Regional Differences of Dietary Inflammatory Index and Its Association with Depression and Depressive Symptoms in Korean Adults.Int J Environ Res Public Health. 2020 May 5;17(9):3205. doi: 10.3390/ijerph17093205. Int J Environ Res Public Health. 2020. PMID: 32380710 Free PMC article.
-
Dietary Inflammatory Potential and the Risk of Incident Depression in Adults: A Systematic Review.Adv Nutr. 2019 Jan 1;10(1):9-18. doi: 10.1093/advances/nmy100. Adv Nutr. 2019. PMID: 30615107 Free PMC article.
References
-
- Major Depression Among Adults. National Institute of Mental Health; 2015. Web.
-
- World Health Organization (WHO) Cardiovascular disease. WHO; 2012. Global Burden of CVD. online.
-
- Statistics NCfH. Health, United States, 2016: With Chartbook on Long-term Trends in Health. Hyattsville, Maryland: 2017. - PubMed
-
- World Health Organization. Depression. Fact Sheet. 2017 Online.
Publication types
MeSH terms
Grants and funding
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical

