Secondary peritonitis: principles of diagnosis and intervention
- PMID: 29914871
- PMCID: PMC6889898
- DOI: 10.1136/bmj.k1407
Secondary peritonitis: principles of diagnosis and intervention
Abstract
Secondary peritonitis accounts for 1% of urgent or emergent hospital admissions and is the second leading cause of sepsis in patients in intensive care units globally. Overall mortality is 6%, but mortality rises to 35% in patients who develop severe sepsis. Despite the dramatic growth in the availability and use of imaging and laboratory tests, the rapid diagnosis and early management of peritonitis remains a challenge for physicians in emergency medicine, surgery, and critical care. In this article, we review the pathophysiology of peritonitis and its potential progression to sepsis, discuss the utility and limitations of the physical examination and laboratory and radiographic tests, and present a paradigm for the management of secondary peritonitis.
Published by the BMJ Publishing Group Limited. For permission to use (where not already granted under a licence) please go to http://group.bmj.com/group/rights-licensing/permissions.
Conflict of interest statement
Competing interests: We have read and understood BMJ policy on declaration of interests and declare the following interests: none.
Figures
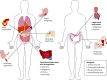

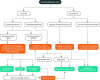

References
-
- Juvonen P, Lehtimäki T, Eskelinen M, et al. The need for surgery in acute abdominal pain: a randomized study of abdominal computed tomography. In Vivo 2014;28:305-9. - PubMed
Publication types
MeSH terms
Grants and funding
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical
