Ecological association between operative vaginal delivery and obstetric and birth trauma
- PMID: 29914910
- PMCID: PMC6008188
- DOI: 10.1503/cmaj.171076
Ecological association between operative vaginal delivery and obstetric and birth trauma
Abstract
Background: Increased use of operative vaginal delivery (use of forceps, vacuum or other device) has been recommended to address high rates of cesarean delivery. We sought to determine the association between rates of operative vaginal delivery and obstetric trauma and severe birth trauma.
Methods: We carried out an ecological analysis of term, singleton deliveries in 4 Canadian provinces (2004-2014) using data from the Canadian Institute for Health Information. The primary exposure was mode of delivery. The primary outcomes were obstetric trauma and severe birth trauma.
Results: Data on 1 938 913 deliveries were analyzed. The rate of obstetric trauma was 7.2% in nulliparous women, and 2.2% and 2.7% among parous women without and with a previous cesarean delivery, respectively, and rates of severe birth trauma were 2.1, 1.7 and 0.7 per 1000, respectively. Each 1% absolute increase in rates of operative vaginal delivery was associated with a higher frequency of obstetric trauma among nulliparous women (adjusted rate ratio [ARR] 1.06, 95% confidence interval [CI] 1.05-1.06), parous women without a previous cesarean delivery (ARR 1.10, 95% CI 1.08-1.13) and parous women with a previous cesarean delivery (ARR 1.11, 95% CI 1.07-1.16). Operative vaginal delivery was associated with more frequent severe birth trauma, but only in nulliparous women (ARR 1.05, 95% CI 1.03-1.07). In nulliparous women, sequential vacuum and forceps instrumentation was associated with the largest increase in obstetric trauma (ARR 1.44, 95% CI 1.35-1.55) and birth trauma (ARR 1.53, 95% CI 1.03-2.27).
Interpretation: Increases in population rates of operative vaginal delivery are associated with higher population rates of obstetric trauma, and in nulliparous women with severe birth trauma.
© 2018 Joule Inc. or its licensors.
Conflict of interest statement
Competing interests: None declared.
Figures
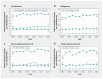
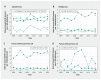
Comment in
-
Taking a stand for operative vaginal delivery.CMAJ. 2018 Jun 18;190(24):E732-E733. doi: 10.1503/cmaj.180668. CMAJ. 2018. PMID: 29914909 Free PMC article. No abstract available.
Similar articles
-
Temporal trends in severe maternal and neonatal trauma during childbirth: a population-based observational study.BMJ Open. 2018 Mar 2;8(3):e020578. doi: 10.1136/bmjopen-2017-020578. BMJ Open. 2018. PMID: 29500215 Free PMC article.
-
Perinatal and maternal morbidity and mortality after attempted operative vaginal delivery at midpelvic station.CMAJ. 2017 Jun 5;189(22):E764-E772. doi: 10.1503/cmaj.161156. CMAJ. 2017. PMID: 28584040 Free PMC article.
-
Operative vaginal delivery and midline episiotomy: a bad combination for the perineum.Am J Obstet Gynecol. 2006 Sep;195(3):749-54. doi: 10.1016/j.ajog.2006.06.078. Am J Obstet Gynecol. 2006. PMID: 16949408
-
Obstetric anal sphincter injuries - review of our date between 2015-2017.Ceska Gynekol. 2019 Winter;84(1):18-22. Ceska Gynekol. 2019. PMID: 31213053 Review. English.
-
Cesarean section on request at 39 weeks: impact on shoulder dystocia, fetal trauma, neonatal encephalopathy, and intrauterine fetal demise.Semin Perinatol. 2006 Oct;30(5):276-87. doi: 10.1053/j.semperi.2006.07.009. Semin Perinatol. 2006. PMID: 17011400 Review.
Cited by
-
Severe birth injuries in neonates and associated risk factors for injury in mothers with different types of diabetes in Finland.Int J Gynaecol Obstet. 2022 Oct;159(1):195-203. doi: 10.1002/ijgo.14073. Epub 2022 Jan 7. Int J Gynaecol Obstet. 2022. PMID: 34927725 Free PMC article.
-
Does birthweight have a role in the effect of episiotomy on anal sphincter injury?Arch Gynecol Obstet. 2020 Jan;301(1):171-177. doi: 10.1007/s00404-020-05444-2. Epub 2020 Jan 27. Arch Gynecol Obstet. 2020. PMID: 31989293
-
Trends and Determinants of Operative Vaginal Delivery at Two Academic Hospitals in Johannesburg, South Africa 2005-2019.Int J Environ Res Public Health. 2022 Dec 3;19(23):16182. doi: 10.3390/ijerph192316182. Int J Environ Res Public Health. 2022. PMID: 36498266 Free PMC article.
-
The authors respond to "Routine use of episiotomy with forceps should not be encouraged".CMAJ. 2020 Feb 24;192(8):E191-E192. doi: 10.1503/cmaj.74565. CMAJ. 2020. PMID: 32094271 Free PMC article. No abstract available.
-
Indigenous Birth as Ceremony and a Human Right.Health Hum Rights. 2021 Jun;23(1):213-224. Health Hum Rights. 2021. PMID: 34194214 Free PMC article.
References
-
- Martin JA, Hamilton BE, Osterman MJK, et al. Births: final data for 2015. National Vital Statistics Report, Vol. 66, No. 1 Hyattsville (MD): National Center for Health Statistics; 2017. - PubMed
-
- Martin JA, Hamilton BE, Osterman MJ, et al. Births: final data for 2012. Natl Vital Stat Rep 2013;62:1–68. - PubMed
-
- Health Canada. Canadian perinatal health report, 2003. Ottawa: Minister of Public Works and Government Services Canada; 2003.
-
- Canadian perinatal health report, 2008 edition. Ottawa: Public Health Agency of Canada; 2008.
-
- American College of Obstetricians and Gynecologists (College); Society for Maternal-Fetal Medicine; Caughey AB, Cahill AG, Guise JM, et al. Safe prevention of the primary cesarean delivery. Am J Obstet Gynecol 2014;210: 179–93. - PubMed
Publication types
MeSH terms
Grants and funding
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical
