Unusual Sites of High-Grade Neuroendocrine Carcinomas: A Case Series and Review of the Literature
- PMID: 29915166
- PMCID: PMC6044230
- DOI: 10.12659/AJCR.908953
Unusual Sites of High-Grade Neuroendocrine Carcinomas: A Case Series and Review of the Literature
Abstract
BACKGROUND Neuroendocrine tumors (NETs) encompass a diverse group of varying clinicopathological entities arising from cells of the endocrine and nervous systems. The presentation of these unique tumors can range from occult disease discovered incidentally to hyperactive, metastatic secretory tumors. NETs most commonly originate in the gastrointestinal and respiratory tract, although they may occur at any site in the body due to the wide distribution of neuroendocrine cells. Their classification system is complex and continues to evolve, and the current system uses histological grade in defining these subtypes. Neuroendocrine carcinomas (NECs), or high-grade, poorly-differentiated NETs, are the most aggressive subtype. Surgical resection remains the primary treatment modality and may be curative, thus early diagnosis is paramount. Management of advanced NETs remains both a diagnostic and therapeutic challenge; however, advances in our understanding of these unique neoplasms as well as an evolving classification system has led to the development of adjunctive therapeutic approaches aimed to minimize morbidity and improve patient outcomes. CASE REPORT We present 6 cases of unusual sites of high-grade neuroendocrine carcinomas involving the cervix, gallbladder, oesophagus, ovary, prostate, and urinary bladder. CONCLUSIONS Our case series highlights the heterogenous and aggressive nature of this subtype of NETs as well as their diagnostic and therapeutic difficulties. We also review the evolution of the NET classification system and its impact on the management of these malignancies.
Conflict of interest statement
None.
Figures
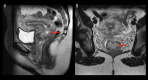


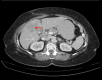
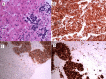
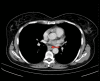
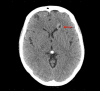
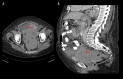


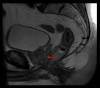

References
-
- Mougey AM, Adler DG. Neuroendocrine tumors: Review and clinical update. Hospital Physician. 2007;43(11):12–20.
-
- Taal BG, Visser O. Epidemiology of neuroendocrine tumors. Neuroendocrinology. 2004;80(Suppl. 1):3–7. - PubMed
-
- Modlin IM, Lye KD, Kidd M. A 5-decade analysis of 13,715 carcinoid tumors. Cancer. 2003;97:934–59. - PubMed
-
- Arnold R, Göke R, Wied M, Behr T. Neuroendocrine gastroentero-pancreatic (GEP) tumors (Chapter 15) In: Scheppach W, Bresalier RS, Tytgat GNJ, editors. Gastrointestinal and liver tumors. Berlin Heidelberg: Springer-Verlag; 2003. pp. 195–233.
-
- Kapoor R, Bhattacharyya T, Gupta R, et al. A systematic review of management of neuroendocrine tumors: An experience from a tertiary care centre from India. Clin Cancer Investig J. 2014;3:363–72.
Publication types
MeSH terms
LinkOut - more resources
Full Text Sources
Other Literature Sources

