A metapopulation model for the spread of MRSA in correctional facilities
- PMID: 29928718
- PMCID: PMC5963330
- DOI: 10.1016/j.idm.2016.06.001
A metapopulation model for the spread of MRSA in correctional facilities
Abstract
The spread of methicillin-resistant strains of Staphylococcus aureus (MRSA) in health-care settings has become increasingly difficult to control and has since been able to spread in the general community. The prevalence of MRSA within the general public has caused outbreaks in groups of people in close quarters such as military barracks, gyms, daycare centres and correctional facilities. Correctional facilities are of particular importance for spreading MRSA, as inmates are often in close proximity and have limited access to hygienic products and clean clothing. Although these conditions are ideal for spreading MRSA, a recent study has suggested that recurrent epidemics are caused by the influx of colonized or infected individuals into the correctional facility. In this paper, we further investigate the effects of community dynamics on the spread of MRSA within the correctional facility and determine whether recidivism has a significant effect on disease dynamics. Using a simplified hotspot model ignoring disease dynamics within the correctional facility, as well as two metapopulation models, we demonstrate that outbreaks in correctional facilities can be driven by community dynamics even when spread between inmates is restricted. We also show that disease dynamics within the correctional facility and their effect on the outlying community may be ignored due to the smaller size of the incarcerated population. This will allow construction of simpler models that consider the effects of many MRSA hotspots interacting with the general community. It is suspected that the cumulative effects of hotspots for MRSA would have a stronger feedback effect in other community settings.
Keywords: Latin Hypercube Sampling; hotspots; mathematical model; metapopulation model; methicillin-resistant Staphylococcus aureus.
Figures
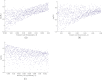
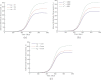
Similar articles
-
Outbreaks of infection caused by community-acquired methicillin-resistant Staphylococcus aureus in a Canadian correctional facility.Can J Infect Dis Med Microbiol. 2005 Nov;16(6):343-8. doi: 10.1155/2005/698181. Can J Infect Dis Med Microbiol. 2005. PMID: 18159517 Free PMC article.
-
Methicillin-resistant Staphylococcus aureus infections in correctional facilities---Georgia, California, and Texas, 2001-2003.MMWR Morb Mortal Wkly Rep. 2003 Oct 17;52(41):992-6. MMWR Morb Mortal Wkly Rep. 2003. PMID: 14561958
-
Predicting COVID-19 Outbreaks in Correctional Facilities Using Machine Learning.MDM Policy Pract. 2024 Jan 29;9(1):23814683231222469. doi: 10.1177/23814683231222469. eCollection 2024 Jan-Jun. MDM Policy Pract. 2024. PMID: 38293655 Free PMC article.
-
The role of international travel in the spread of methicillin-resistant Staphylococcus aureus.J Travel Med. 2014 Jul-Aug;21(4):272-81. doi: 10.1111/jtm.12133. Epub 2014 Jun 3. J Travel Med. 2014. PMID: 24894491 Review.
-
Methicillin-resistant Staphylococcus aureus in extended-care facilities: experiences in a Veterans' Affairs nursing home and a review of the literature.Infect Control Hosp Epidemiol. 1991 Jan;12(1):36-45. doi: 10.1086/646236. Infect Control Hosp Epidemiol. 1991. PMID: 1999642 Review.
Cited by
-
A systematic review of transmission dynamic studies of methicillin-resistant Staphylococcus aureus in non-hospital residential facilities.BMC Infect Dis. 2018 Apr 18;18(1):188. doi: 10.1186/s12879-018-3060-6. BMC Infect Dis. 2018. PMID: 29669512 Free PMC article.
-
Dynamic Models of Infectious Disease Transmission in Prisons and the General Population.Epidemiol Rev. 2018 Jun 1;40(1):40-57. doi: 10.1093/epirev/mxx014. Epidemiol Rev. 2018. PMID: 29566137 Free PMC article.
-
Effects of the proportion of high-risk patients and control strategies on the prevalence of methicillin-resistant Staphylococcus aureus in an intensive care unit.BMC Infect Dis. 2019 Dec 3;19(1):1026. doi: 10.1186/s12879-019-4632-9. BMC Infect Dis. 2019. PMID: 31795957 Free PMC article.
-
Quantifying the relative impact of contact heterogeneity on MRSA transmission in ICUs - a modelling study.BMC Infect Dis. 2020 Jan 3;20(1):6. doi: 10.1186/s12879-019-4738-0. BMC Infect Dis. 2020. PMID: 31900118 Free PMC article.
-
Conjugative Transfer of a Novel Staphylococcal Plasmid Encoding the Biocide Resistance Gene, qacA.Front Microbiol. 2018 Nov 19;9:2664. doi: 10.3389/fmicb.2018.02664. eCollection 2018. Front Microbiol. 2018. PMID: 30510541 Free PMC article.
References
-
- Bick J.A. Infection control in jails and prisons. Healthcare Epidemiology. 2007;45:1047–1055. - PubMed
-
- Blower S.M., Dowlatabadi H. Sensitivity and uncertainty analysis of complex models of disease transmission: And HIV model, as an example. International Statistical Review = Revue Internationale de Statistique. 1994;62(2):229–243.
LinkOut - more resources
Full Text Sources
Other Literature Sources

