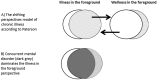
'I've put diabetes completely on the shelf till the mental stuff is in place'. How patients with doctor-assessed impaired self-care perceive disease, self-care, and support from general practitioners. A qualitative study
- PMID: 29929420
- PMCID: PMC6161682
- DOI: 10.1080/02813432.2018.1487436
'I've put diabetes completely on the shelf till the mental stuff is in place'. How patients with doctor-assessed impaired self-care perceive disease, self-care, and support from general practitioners. A qualitative study
Abstract
Objective: This paper investigated patients' experiences of disease and self-care as well as perceptions of the general practitioner's role in supporting patients with impaired self-care ability.
Design: Qualitative interviews with 13 patients with type 2 diabetes, concurrent chronic diseases, and impaired self-care ability assessed by a general practitioner. We analyzed our data using systematic text condensation. The shifting perspectives model of chronic illness formed the theoretical background for the study.
Results: Although most patients experienced challenges in adhering to recommended self-care activities, many had developed additional, personal self-care routines that increased wellbeing. Some patients were conscious of self-care trade-offs, including patients with concurrent mental disorders who were much more attentive to their mental disorder than their somatic diseases. Patients' perspectives on diseases could shift over time and were dominated by emotional considerations such as insisting on leading a normal life or struggling with limitations caused by disease. Most patients found support in the ongoing relationship with the same general practitioner, who was valued as a companion or appreciated as a trustworthy health informant.
Conclusion: Patient experiences of self-care may collide with what general practitioners find appropriate in a medical regimen. Health professionals should be aware of patients' prominent and shifting considerations about the emotional aspects of disease. Patients valued the general practitioner's role in self-care support, primarily through the long-term doctor-patient relationship. Therefore, relational continuity should be prioritized in chronic care, especially for patients with impaired self-care ability who often have a highly complex disease burden and situational context. Key points Little is known about the perspectives of disease and self-care in patients with a doctor-assessed impaired ability of self-care. • Although patients knew the prescribed regimen they often prioritized self-care routines that increased well-being at the cost of medical recommendations. • Shifting emotional aspects were prominent in patients' considerations of disease and sustained GPs' use of a patient-centred clinical method when discussing self-care. • Relational continuity with general practitioners was a highly valued support and should be prioritized for patients with impaired self-care.
Keywords: Multimorbidity; chronic disease; continuity of patient care; general practice; patient acceptance of health care; self-care.
Figures
Similar articles
-
How general practitioners perceive and assess self-care in patients with multiple chronic conditions: a qualitative study.BMC Fam Pract. 2017 Dec 22;18(1):109. doi: 10.1186/s12875-017-0679-0. BMC Fam Pract. 2017. PMID: 29273001 Free PMC article.
-
Personal continuity and access in UK general practice: a qualitative study of general practitioners' and patients' perceptions of when and how they matter.BMC Fam Pract. 2006 Feb 24;7:11. doi: 10.1186/1471-2296-7-11. BMC Fam Pract. 2006. PMID: 16504130 Free PMC article.
-
Capacity, responsibility, and motivation: a critical qualitative evaluation of patient and practitioner views about barriers to self-management in people with multimorbidity.BMC Health Serv Res. 2014 Oct 31;14:536. doi: 10.1186/s12913-014-0536-y. BMC Health Serv Res. 2014. PMID: 25367263 Free PMC article.
-
General practitioner strategies for managing patients with multimorbidity: a systematic review and thematic synthesis of qualitative research.BMC Fam Pract. 2020 Jul 1;21(1):131. doi: 10.1186/s12875-020-01197-8. BMC Fam Pract. 2020. PMID: 32611391 Free PMC article.
-
[Is it quality of life that patients really want? Assessment from a general practitioner's perspective].Z Evid Fortbild Qual Gesundhwes. 2014;108(2-3):126-9. doi: 10.1016/j.zefq.2014.03.003. Epub 2014 Apr 2. Z Evid Fortbild Qual Gesundhwes. 2014. PMID: 24780710 Review. German.
Cited by
-
"It's up to me": the experience of patients at high risk of cardiovascular disease of lifestyle change.Scand J Prim Health Care. 2020 Sep;38(3):340-351. doi: 10.1080/02813432.2020.1794414. Epub 2020 Jul 17. Scand J Prim Health Care. 2020. PMID: 32677859 Free PMC article.
-
General practitioners' experiences in consultations with foreign language patients after the introduction of a user's fee for professional interpretation: a qualitative interview study.BMC Prim Care. 2022 May 2;23(1):103. doi: 10.1186/s12875-022-01718-7. BMC Prim Care. 2022. PMID: 35501707 Free PMC article.
-
Exploring treatment burden in people with type 2 diabetes mellitus: a thematic analysis in china's primary care settings.BMC Prim Care. 2024 Mar 15;25(1):88. doi: 10.1186/s12875-024-02301-y. BMC Prim Care. 2024. PMID: 38491369 Free PMC article. Review.
-
Diabetes care provided by national standards can improve patients' self-management skills: A qualitative study of how people with type 2 diabetes perceive primary diabetes care.Health Expect. 2021 Jun;24(3):1000-1008. doi: 10.1111/hex.13247. Epub 2021 Mar 28. Health Expect. 2021. PMID: 33774899 Free PMC article.
-
Patient perspectives on multidimensional learning and person-centred care: interviews with persons living with type 2 diabetes.Scand J Prim Health Care. 2025 Mar;43(1):230-240. doi: 10.1080/02813432.2024.2423881. Epub 2024 Nov 4. Scand J Prim Health Care. 2025. PMID: 39497381 Free PMC article.
References
-
- Bodenheimer T, Wagner EH, Grumbach K. Improving primary care for patients with chronic illness. Jama 2002;288:1775–1779. - PubMed
-
- Chronic disease management – a national strategy. Disease management programmes and self-management support. Copenhagen: The National Board of Health; 2007.
-
- Forløbsprogram for Type 2 Diabetes Mellitus [Disease management programme for type 2 diabetes mellitus]: Region Zealand – Denmark; 2011.
-
- Blakeman T, Bower P, Reeves D, et al. . Bringing self-management into clinical view: a qualitative study of long-term condition management in primary care consultations. Chronic Illn. 2010;6:136–150. - PubMed
MeSH terms
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical