Using Neural Networks with Routine Health Records to Identify Suicide Risk: Feasibility Study
- PMID: 29934287
- PMCID: PMC6035342
- DOI: 10.2196/10144
Using Neural Networks with Routine Health Records to Identify Suicide Risk: Feasibility Study
Abstract
Background: Each year, approximately 800,000 people die by suicide worldwide, accounting for 1-2 in every 100 deaths. It is always a tragic event with a huge impact on family, friends, the community and health professionals. Unfortunately, suicide prevention and the development of risk assessment tools have been hindered by the complexity of the underlying mechanisms and the dynamic nature of a person's motivation and intent. Many of those who die by suicide had contact with health services in the preceding year but identifying those most at risk remains a challenge.
Objective: To explore the feasibility of using artificial neural networks with routinely collected electronic health records to support the identification of those at high risk of suicide when in contact with health services.
Methods: Using the Secure Anonymised Information Linkage Databank UK, we extracted the data of those who died by suicide between 2001 and 2015 and paired controls. Looking at primary (general practice) and secondary (hospital admissions) electronic health records, we built a binary feature vector coding the presence of risk factors at different times prior to death. Risk factors included: general practice contact and hospital admission; diagnosis of mental health issues; injury and poisoning; substance misuse; maltreatment; sleep disorders; and the prescription of opiates and psychotropics. Basic artificial neural networks were trained to differentiate between the suicide cases and paired controls. We interpreted the output score as the estimated suicide risk. System performance was assessed with 10x10-fold repeated cross-validation, and its behavior was studied by representing the distribution of estimated risk across the cases and controls, and the distribution of factors across estimated risks.
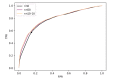
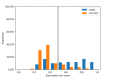
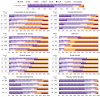
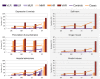
Results: We extracted a total of 2604 suicide cases and 20 paired controls per case. Our best system attained a mean error rate of 26.78% (SD 1.46; 64.57% of sensitivity and 81.86% of specificity). While the distribution of controls was concentrated around estimated risks < 0.5, cases were almost uniformly distributed between 0 and 1. Prescription of psychotropics, depression and anxiety, and self-harm increased the estimated risk by ~0.4. At least 95% of those presenting these factors were identified as suicide cases.
Conclusions: Despite the simplicity of the implemented system, the proposed methodology obtained an accuracy like other published methods based on specialized questionnaire generated data. Most of the errors came from the heterogeneity of patterns shown by suicide cases, some of which were identical to those of the paired controls. Prescription of psychotropics, depression and anxiety, and self-harm were strongly linked with higher estimated risk scores, followed by hospital admission and long-term drug and alcohol misuse. Other risk factors like sleep disorders and maltreatment had more complex effects.
Keywords: artificial neural networks; electronic health records; machine learning; risk assessment; routine data; suicide prevention.
©Marcos DelPozo-Banos, Ann John, Nicolai Petkov, Damon Mark Berridge, Kate Southern, Keith LLoyd, Caroline Jones, Sarah Spencer, Carlos Manuel Travieso. Originally published in JMIR Mental Health (http://mental.jmir.org), 22.06.2018.
Conflict of interest statement
Conflicts of Interest: None declared.
Figures


Similar articles
-
Suicide Information Database-Cymru: a protocol for a population-based, routinely collected data linkage study to explore risks and patterns of healthcare contact prior to suicide to identify opportunities for intervention.BMJ Open. 2014 Nov 25;4(11):e006780. doi: 10.1136/bmjopen-2014-006780. BMJ Open. 2014. PMID: 25424996 Free PMC article.
-
Right care, first time: a highly personalised and measurement-based care model to manage youth mental health.Med J Aust. 2019 Nov;211 Suppl 9:S3-S46. doi: 10.5694/mja2.50383. Med J Aust. 2019. PMID: 31679171
-
Contacts with primary and secondary healthcare prior to suicide: case-control whole-population-based study using person-level linked routine data in Wales, UK, 2000-2017.Br J Psychiatry. 2020 Dec;217(6):717-724. doi: 10.1192/bjp.2020.137. Br J Psychiatry. 2020. PMID: 32744207 Free PMC article.
-
[The European Psychiatric Association (EPA) guidance on suicide treatment and prevention].Neuropsychopharmacol Hung. 2012 Jun;14(2):113-36. Neuropsychopharmacol Hung. 2012. PMID: 22710852 Review. Hungarian.
-
Systematic reviews of the effectiveness of day care for people with severe mental disorders: (1) acute day hospital versus admission; (2) vocational rehabilitation; (3) day hospital versus outpatient care.Health Technol Assess. 2001;5(21):1-75. doi: 10.3310/hta5210. Health Technol Assess. 2001. PMID: 11532238 Review.
Cited by
-
Incidence, Mortality and Survival in Young People with Co-Occurring Mental Disorders and Substance Use: A Retrospective Linked Routine Data Study in Wales.Clin Epidemiol. 2022 Jan 13;14:21-38. doi: 10.2147/CLEP.S325235. eCollection 2022. Clin Epidemiol. 2022. PMID: 35058718 Free PMC article.
-
A systematic review of clinical health conditions predicted by machine learning diagnostic and prognostic models trained or validated using real-world primary health care data.PLoS One. 2023 Sep 8;18(9):e0274276. doi: 10.1371/journal.pone.0274276. eCollection 2023. PLoS One. 2023. PMID: 37682909 Free PMC article.
-
Accurate Diagnosis of Suicide Ideation/Behavior Using Robust Ensemble Machine Learning: A University Student Population in the Middle East and North Africa (MENA) Region.Diagnostics (Basel). 2020 Nov 16;10(11):956. doi: 10.3390/diagnostics10110956. Diagnostics (Basel). 2020. PMID: 33207776 Free PMC article.
-
Clinician-recalled quoted speech in electronic health records and risk of suicide attempt: a case-crossover study.BMJ Open. 2020 Apr 22;10(4):e036186. doi: 10.1136/bmjopen-2019-036186. BMJ Open. 2020. PMID: 32327481 Free PMC article.
-
Identifying long-term and imminent suicide predictors in a general population and a clinical sample with machine learning.BMC Psychiatry. 2022 Feb 15;22(1):120. doi: 10.1186/s12888-022-03702-y. BMC Psychiatry. 2022. PMID: 35168594 Free PMC article.
References
-
- World Health Organization (2017) [2018-05-10]. Suicide Fact sheet ( Updated August 2017 http://www.who.int/mediacentre/factsheets/fs398/en/)
-
- Statistics for Wales and Welsh Government (2017) [2018-05-10]. Police recorded road accidents in Wales, 2016 https://gov.wales/statistics-and-research/police-recorded-road-casualtie... .
-
- Case A, Deaton A. Mortality and morbidity in the 21 century. Brookings Pap Econ Act. 2017;2017:397–476. http://europepmc.org/abstract/MED/29033460 - PMC - PubMed
-
- McDaid D. Making an Economic Case for Investing in Suicide Prevention. The International Handbook of Suicide Prevention. 2016:775–790. doi: 10.1002/9781118903223.ch44. - DOI
-
- Public HE. Local suicide prevention planning, a practice resource. PHE publications gateway number. 2016:2016392.
LinkOut - more resources
Full Text Sources
Other Literature Sources

