Disclosure of Same-Sex Behaviors to Health-care Providers and Uptake of HIV Testing for Men Who Have Sex With Men: A Systematic Review
- PMID: 29947563
- PMCID: PMC6142161
- DOI: 10.1177/1557988318784149
Disclosure of Same-Sex Behaviors to Health-care Providers and Uptake of HIV Testing for Men Who Have Sex With Men: A Systematic Review
Abstract
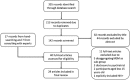
To promote HIV-testing and offer optimal care for men who have sex with men (MSM), health-care providers (HCPs) must first be aware of their patients' sexual behaviors. Otherwise, HCPs may overlook MSM's risks for HIV infection and their special health-care needs. For MSM, reporting their same-sex behaviors to HCPs (disclosure to HCPs) may promote their linkage to HIV prevention and treatment cascade and improve their health outcomes. No literature review has been conducted to examine the relationship between disclosure to HCPs and uptake of HIV-testing among MSM. The current study reviewed and synthesized findings from 29 empirical studies published in English by 2016. We summarized the rates of MSM's disclosure to HCPs, investigated the association between disclosure and HIV-testing among MSM, identified potential facilitators and barriers for disclosure, and discussed the implications of our findings in research and clinical practices. The disclosure rates varied across subgroups and study settings, ranging from 16% to 90% with a median of 61%. Disclosure to HCPs was positively associated with uptake of HIV-testing. African American MSM were less likely to disclose to HCPs. MSM who lived in urban settings with higher education attainment and higher income were more likely to disclose. MSM tended to perceive younger or gay-friendly doctors as safer targets of disclosure. Clinics with LGBT-friendly signs were viewed as safer contexts for disclosure. Having previous communications about substance use, sex, and HIV with HCPs could also facilitate disclosure. The main reasons for nondisclosure included lack of probing from HCPs, concerns on confidentiality breach and stigma, and perceived irrelevance with services. Providing appropriate trainings for HCPs and creating gay-friendly clinical settings can be effective strategies to facilitate disclosures of same-sex behaviors among MSM and meet their specific medical needs. Interventions to promote disclosure should give priorities to MSM from the most marginalized subgroups (e.g., MSM in rural areas, MSM of ethnic minorities).
Keywords: HIV-testing; MSM; disclosure of same-sex behavior; disclosure to HCPs; literature review.
Conflict of interest statement
Figures
References
-
- Adams J., McCreanor T., Braun V. (2008). Doctoring New Zealand’s gay men. The New Zealand Medical Journal, 121(1287), 11–21. - PubMed
-
- Adams J., McCreanor T., Braun V. (2013). Gay men’s explanations of health and how to improve it. Qualitative Health Research, 23(7), 887–899. - PubMed
-
- Bernstein K. T., Liu K. L., Begier E. M., Koblin B., Karpati A., Murrill C. (2008). Same-sex attraction disclosure to health care providers among New York City men who have sex with men: Implications for HIV testing approaches. Archives of Internal Medicine, 168(13), 1458–1464. - PubMed
Publication types
MeSH terms
Grants and funding
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical