Incidence of and risk factors for stoma-site incisional herniation after reversal
- PMID: 29951636
- PMCID: PMC5989939
- DOI: 10.1002/bjs5.48
Incidence of and risk factors for stoma-site incisional herniation after reversal
Abstract
Background: Stoma reversal is often considered a straightforward procedure with low short-term complication rates. The aim of this study was to determine the rate of incisional hernia following stoma reversal and identify risk factors for its development.
Methods: This was an observational study of consecutive patients who underwent stoma reversal between 2009 and 2015 at a teaching hospital. Patients followed for at least 12 months were eligible. The primary outcome was the development of incisional hernia at the previous stoma site. Independent risk factors were assessed using multivariable logistic regression analysis.
Results: After a median follow-up of 24 (range 12-89) months, 110 of 318 included patients (34·6 per cent) developed an incisional hernia at the previous stoma site. In 85 (77·3 per cent) the hernia was symptomatic, and 72 patients (65·5 per cent) underwent surgical correction. Higher BMI (odds ratio (OR) 1·12, 95 per cent c.i. 1·04 to 1·21), stoma prolapse (OR 3·27, 1·04 to 10·27), parastomal hernia (OR 5·08, 1·30 to 19·85) and hypertension (OR 2·52, 1·14 to 5·54) were identified as independent risk factors for the development of incisional hernia at the previous stoma site. In addition, the risk of incisional hernia was greater in patients with underlying malignant disease who had undergone a colostomy than in those who had had an ileostomy (OR 5·05, 2·28 to 11·23).
Conclusion: Incisional hernia of the previous stoma site was common and frequently required surgical correction. Higher BMI, reversal of colostomy in patients with an underlying malignancy, stoma prolapse, parastomal hernia and hypertension were identified as independent risk factors.
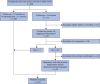
Figures
Comment in
-
Incidence of and risk factors for stoma-site incisional herniation after reversal.BJS Open. 2019 May 7;3(3):415. doi: 10.1002/bjs5.50165. eCollection 2019 Jun. BJS Open. 2019. PMID: 31183458 Free PMC article. No abstract available.
References
-
- Chow A, Tilney HS, Paraskeva P, Jeyarajah S, Zacharakis E, Purkayastha S. The morbidity surrounding reversal of defunctioning ileostomies: a systematic review of 48 studies including 6107 cases. Int J Colorectal Dis 2009; 24: 711–723. - PubMed
-
- Cingi A, Cakir T, Sever A, Aktan AO. Enterostomy site hernias: a clinical and computerized tomographic evaluation. Dis Colon Rectum 2006; 49: 1559–1563. - PubMed
-
- Tilney HS, Sains PS, Lovegrove RE, Reese GE, Heriot AG, Tekkis PP. Comparison of outcomes following ileostomy versus colostomy for defunctioning colorectal anastomoses. World J Surg 2007; 31: 1142–1151. - PubMed
-
- Bakx R, Busch OR, Bemelman WA, Veldink GJ, Slors JF, van Lanschot JJ. Morbidity of temporary loop ileostomies. Dig Surg 2004; 21: 277–281. - PubMed
LinkOut - more resources
Full Text Sources
Other Literature Sources