Engineering Intravenously Administered Nanoparticles to Reduce Infusion Reaction and Stop Bleeding in a Large Animal Model of Trauma
- PMID: 29965731
- PMCID: PMC6830447
- DOI: 10.1021/acs.bioconjchem.8b00335
Engineering Intravenously Administered Nanoparticles to Reduce Infusion Reaction and Stop Bleeding in a Large Animal Model of Trauma
Abstract
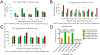
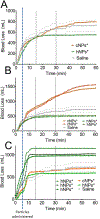
Bleeding from traumatic injury is the leading cause of death for young people across the world, but interventions are lacking. While many agents have shown promise in small animal models, translating the work to large animal models has been exceptionally difficult in great part because of infusion-associated complement activation to nanomaterials that leads to cardiopulmonary complications. Unfortunately, this reaction is seen in at least 10% of the population. We developed intravenously infusible hemostatic nanoparticles that were effective in stopping bleeding and improving survival in rodent models of trauma. To translate this work, we developed a porcine liver injury model. Infusion of the first generation of hemostatic nanoparticles and controls 5 min after injury led to massive vasodilation and exsanguination even at extremely low doses. In naïve animals, the physiological changes were consistent with a complement-associated infusion reaction. By tailoring the zeta potential, we were able to engineer a second generation of hemostatic nanoparticles and controls that did not exhibit the complement response at low and moderate doses but did at the highest doses. These second-generation nanoparticles led to cessation of bleeding within 10 min of administration even though some signs of vasodilation were still seen. While the complement response is still a challenge, this work is extremely encouraging in that it demonstrates that when the infusion-associated complement response is managed, hemostatic nanoparticles are capable of rapidly stopping bleeding in a large animal model of trauma.
Figures


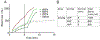

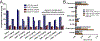
References
-
- Rhee P, Joseph B, Pandit V, Aziz H, Vercruysse G, Kulvatunyou N, and Friese RS (2014) Increasing trauma deaths in the United States. Ann Surg 260, 13–21. - PubMed
-
- Committee on Military Trauma Care’s Learning Health, S., Its Translation to the Civilian, S., Board on Health Sciences, P., Board on the Health of Select, P., Health, Medicine, D., National Academies of Sciences, E., and Medicine (2016) A National Trauma Care System: Integrating Military and Civilian Trauma Systems to Achieve Zero Preventable Deaths After Injury, National Academies Press (US) Copyright 2016 by the National Academy of Sciences. All rights reserved., Washington (DC). - PubMed
-
- Sauaia A, Moore FA, Moore EE, Moser KS, Brennan R, Read RA, and Pons PT (1995) Epidemiology of trauma deaths: a reassessment. Journal Of Trauma‐injury Infection And Critical Care 38, 185–193. - PubMed
-
- Champion HR, Bellamy RF, Roberts CP, and Leppaniemi A (2003) A profile of combat injury. Journal Of Trauma‐injury Infection And Critical Care 54, 13. - PubMed
Publication types
MeSH terms
Substances
Grants and funding
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical

