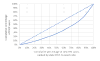
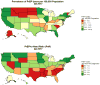
The prevalence of pre-exposure prophylaxis use and the pre-exposure prophylaxis-to-need ratio in the fourth quarter of 2017, United States
- PMID: 29983236
- PMCID: PMC6286209
- DOI: 10.1016/j.annepidem.2018.06.005
The prevalence of pre-exposure prophylaxis use and the pre-exposure prophylaxis-to-need ratio in the fourth quarter of 2017, United States
Abstract
Purpose: The number of individuals who have started a regimen for HIV pre-exposure prophylaxis (PrEP) in the United States is not well characterized but has been on the rise since 2012. This analysis assesses the distribution of PrEP use nationally and among subgroups.
Methods: A validated algorithm quantifying tenofovir disoproxil fumarate/emtricitabine for PrEP in the United States was applied to a national prescription database to determine the quarterly prevalence of PrEP use. HIV diagnoses from 2016 were used as an epidemiological proxy for PrEP need. The PrEP-to-need ratio (PnR) was defined as the number of PrEP users divided by new HIV diagnoses.
Results: A total of 70,395 individuals used PrEP in the fourth quarter of 2017: 67,166 males and 3229 females. Nationally, prevalence of PrEP use was 26/100,000 (range across states per 100,000 [RAS/100k]: 4-73) and the PnR was 1.8 (RAS: 0.5-6.6). Prevalence of PrEP use among males and females, respectively, was 50/100,000 and 2/100,000 (RAS/100k: 7-143 and 0.3-7) and PnR was 2.1 and 0.4 (RAS: 0.6-7.1 and 0.1-4.0). Prevalence of PrEP use was lowest among individuals aged less than or equal to 24 and more than or equal to 55 years (15/100,000 and 6/100,000, RAS/100k: 1-45 and 0.4-14), with PnR 0.9 and 1.5 (RAS: 0.2-5.6 and 0.3-7.0). The Northeast had the highest PnR (3.3); the South had the lowest (1.0). States with Medicaid expansion had more than double the PnR than states without expansion.
Conclusions: Available data suggest that females, individuals aged less than or equal to 24 years and residents of the South had lower levels of PrEP use relative to epidemic need. These results are ecological, and misclassification may attenuate results. PnR is useful for future assessments of HIV prevention strategy uptake.
Keywords: HIV; Pre-exposure prophylaxis; Prevention.
Copyright © 2018 The Authors. Published by Elsevier Inc. All rights reserved.
Figures
References
-
- Choopanya K, Martin M, Suntharasamai P, et al. Antiretroviral prophylaxis for HIV infection in injecting drug users in Bangkok, Thailand (the Bangkok Tenofovir Study): a randomised, double-blind, placebo-controlled phase 3 trial. The Lancet. 381(9883):2083–2090. - PubMed
-
- Martin M, Vanichseni S, Suntharasamai P, et al. The impact of adherence to preexposure prophylaxis on the risk of HIV infection among people who inject drugs. Aids. 2015;29(7):819–824. - PubMed
Publication types
MeSH terms
Substances
Grants and funding
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical
Miscellaneous