Improving Delivery of Secondary Prophylaxis for Rheumatic Heart Disease in a High-Burden Setting: Outcome of a Stepped-Wedge, Community, Randomized Trial
- PMID: 30018165
- PMCID: PMC6064833
- DOI: 10.1161/JAHA.118.009308
Improving Delivery of Secondary Prophylaxis for Rheumatic Heart Disease in a High-Burden Setting: Outcome of a Stepped-Wedge, Community, Randomized Trial
Abstract
Background: Health system strengthening is needed to improve delivery of secondary prophylaxis against rheumatic heart disease.
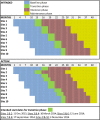
Methods and results: We undertook a stepped-wedge, randomized trial in northern Australia. Five pairs of Indigenous community clinics entered the study at 3-month steps. Study phases comprised a 12 month baseline phase, 3 month transition phase, 12 month intensive phase and a 3- to 12-month maintenance phase. Clinics received a multicomponent intervention supporting activities to improve penicillin delivery, aligned with the chronic care model, with continuous quality-improvement feedback on adherence. The primary outcome was the proportion receiving ≥80% of scheduled penicillin injections. Secondary outcomes included "days at risk" of acute rheumatic fever recurrence related to late penicillin and acute rheumatic fever recurrence rates. Overall, 304 patients requiring prophylaxis were eligible. The proportion receiving ≥80% of scheduled injections during baseline was 141 of 304 (46%)-higher than anticipated. No effect attributable to the study was evident: in the intensive phase, 126 of 304 (41%) received ≥80% of scheduled injections (odds ratio compared with baseline: 0.78; 95% confidence interval, 0.54-1.11). There was modest improvement in the maintenance phase among high-adhering patients (43% received ≥90% of injections versus 30% [baseline] and 28% [intensive], P<0.001). Also, the proportion of days at risk in the whole cohort decreased in the maintenance phase (0.28 versus 0.32 [baseline] and 0.34 [intensive], P=0.001). Acute rheumatic fever recurrence rates did not differ between study sites during the intensive phase and the whole jurisdiction (3.0 versus 3.5 recurrences per 100 patient-years, P=0.65).
Conclusions: This strategy did not improve adherence to rheumatic heart disease secondary prophylaxis within the study time frame. Longer term primary care strengthening strategies are needed.
Clinical trial registration: URL: www.anzctr.org.au. Unique identifier: ACTRN12613000223730.
Keywords: acute rheumatic fever; adherence; cluster randomized trial; quality improvement; rheumatic heart disease; systems of care.
© 2018 The Authors. Published on behalf of the American Heart Association, Inc., by Wiley.
Figures


References
-
- Ralph AP, Carapetis JR. Group A streptococcal diseases and their global burden. Curr Top Microbiol Immunol. 2013;368:1–27. - PubMed
-
- Australian Institute of Health and Welfare . Australian Burden of Disease Study: impact and causes of illness and death in Aboriginal and Torres Strait Islander people 2011. Australian Burden of Disease Study series no. 6. Cat. no. BOD 7. Canberra: AIHW; 2016. Available at: https://www.aihw.gov.au/getmedia/e31976fc-adcc-4612-bd08-e54fd2f3303c/19.... Accessed June 22, 2018.
-
- Australian Institute of Health and Welfare . Aboriginal and Torres Strait Islander Health Performance Framework 2014 online data tables. Measure 1.06: Acute rheumatic fever and rheumatic heart disease. 2015. Available at: http://www.aihw.gov.au/indigenous-data/health-performance-framework/. Accessed June 22, 2018.
-
- Roberts KV, Maguire GP, Brown A, Atkinson DN, Remenyi B, Wheaton G, Ilton M, Carapetis J. Rheumatic heart disease in Indigenous children in northern Australia: differences in prevalence and the challenges of screening. Med J Aust. 2015;203:221.e1–7. - PubMed
-
- Australian Institute of Health and Welfare . Rheumatic heart disease and acute rheumatic fever in Australia: 1996–2012, Cardiovascular Disease Series. Cat. no. CVD 60. Canberra; 2013.
Publication types
MeSH terms
Substances
Associated data
LinkOut - more resources
Full Text Sources
Other Literature Sources

