Electronic alerts, comparative practitioner metrics, and education improve thromboprophylaxis and reduce venous thrombosis in community hospitals
- PMID: 30046752
- PMCID: PMC6046588
- DOI: 10.1002/rth2.12119
Electronic alerts, comparative practitioner metrics, and education improve thromboprophylaxis and reduce venous thrombosis in community hospitals
Abstract
Background: Venous thromboembolism prophylaxis remains underutilized in hospitalized medical patients at high risk for venous thromboembolism. We previously reported that a multifaceted intervention was associated with a sustained increase in appropriate thromboprophylaxis and reduced symptomatic venous thromboembolism among medical patients hospitalized in two urban teaching hospitals. The effectiveness of this intervention in community hospitals is unknown.
Methods: We performed a prospective multicenter cohort study in three community hospitals. All medical patients admitted from February 1, 2011 to January 31, 2014 were eligible. Consecutive eligible patients were enrolled into the 12-month "control," 12-month "intervention," or 12-month "maintenance" group. We provided electronic alerts, physician performance feedback, and targeted medical education for the intervention group. Only the alert component of the intervention continued in the maintenance group. The primary outcome was the rate of appropriate thromboprophylaxis among patients at high risk for venous thromboembolism defined as the prescription of guideline recommended chemoprophylaxis, or identification of a chemoprophylaxis contraindication. Secondary outcomes included rates of symptomatic venous thromboembolism, major bleeding, all-cause mortality, heparin-induced thrombocytopenia, physician satisfaction, and alert fatigue.
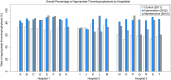
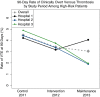
Results: Appropriate thromboprophylaxis when compared to the control group rate of 67% was higher for the intervention group (85%) and for the maintenance group (77%; P < .001 for each comparison). A reduction of 90-day symptomatic venous thromboembolism accompanied the intervention (control 4.5%, intervention 3.4%, maintenance 3.0%, P = .04).
Conclusions: This multifaceted intervention was associated with an overall increase in appropriate thromboprophylaxis of medical patients compared with the control period. Hospital-associated venous thrombosis rates decreased.
Keywords: prevention; quality improvement; thromboprophylaxis medical patient; venous thromboembolism.
Figures

References
-
- Leizorovicz A, Cohen AT, Turpie AG, Olsson CG, Vaitkus PT, Goldhaber SZ. Randomized, placebo‐controlled trial of dalteparin for the prevention of venous thromboembolism in acutely ill medical patients. Circulation. 2004;110:874–9. - PubMed
-
- Samama MM, Cohen AT, Darmon JY, et al. A comparison of enoxaparin with placebo for the prevention of venous thromboembolism in acutely ill medical patients. Prophylaxis in Medical Patients with Enoxaparin Study Group. N Engl J Med. 1999;341:793–800. - PubMed
-
- Barbar S, Noventa F, Rossetto V, et al. A risk assessment model for the identification of hospitalized medical patients at risk for venous thromboembolism: the Padua Prediction Score. J Thromb Haemost. 2010;8:2450–7. - PubMed
-
- Woller SC, Stevens SM, Evans RS, et al. Electronic alerts, comparative practitioner metrics, and education improves thromboprophylaxis and reduces thrombosis. Am J Med. 2016;129:1124.e1117–26. - PubMed
LinkOut - more resources
Full Text Sources
Other Literature Sources

