Denosumab compared to bisphosphonates to treat postmenopausal osteoporosis: a meta-analysis
- PMID: 30071889
- PMCID: PMC6090940
- DOI: 10.1186/s13018-018-0865-3
Denosumab compared to bisphosphonates to treat postmenopausal osteoporosis: a meta-analysis
Abstract
Background: The standard treatment for osteoporosis was controversial. Denosumab and bisphosphonates were two most common drugs. The purpose of this study was to compare the efficacy and safety of denosumab with bisphosphonates to treat osteoporosis.
Methods: Published literatures, only including randomized controlled trials (RCTs), were searched in the following electronic databases: PubMed, Embase, Web of Science, Cochrane Library, and Google database from inception to April 20 2018. Studies that compared denosumab with bisphosphonates to treat osteoporosis were included. Random-effect model was used for meta-analysis due to the unavoidable clinical heterogeneity. We used the risk of fracture as the primary outcome. Stata 12.0 was used for meta-analysis.
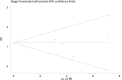
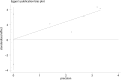
Results: Eleven studies involving 5446 patients (denosumab = 2873, bisphosphonates = 2573) were included in the present meta-analysis. There was no significant difference between the risk of fracture (risk ratio (RR), 1.13; 95% confidence interval (CI), 0.82-1.55; P = 0.466), adverse events (AEs) (RR 1.00; 95% CI 0.96-1.04; P = 0.957) and withdrawn due to AEs (RR 0.68; 95% CI 0.34-137; P = 0.280). Denosumab compared with bisphosphonates significantly increased change in total hip, femoral neck, lumbar spine, and one-third radius bone mineral density (BMD) for postmenopausal osteoporosis patients (P < 0.05).
Conclusions: Our meta-analysis suggested that denosumab but not bisphosphonates significantly increased change in total hip, femoral neck, lumbar spine, and one-third radius BMD for postmenopausal osteoporosis patients. Current evidence suggested no benefit of denosumab for reducing risk of fracture than bisphosphonates. More long-term follow-up RCTs are needed to identify the potential complications of denosumab.
Keywords: Bisphosphonates; Denosumab; Fracture; Meta-analysis.
Conflict of interest statement
This is a meta-analysis; no relative problems exist.
Not applicable.
The authors declare that they have no competing interests.
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Figures












References
-
- Liu W, et al. Meta-analysis of osteoporosis: fracture risks, medication and treatment. Minerva Med. 2015;106(4):203–214. - PubMed
-
- Maghbooli Z, et al. Negative correlation of high-density of lipoprotein-cholesterol and bone mineral density in postmenopausal Iranian women with vitamin D deficiency. Menopause. 2018. 10.1097/GME.0000000000001082. - PubMed
-
- Buerba RA, et al. Bisphosphonate and Teriparatide use in thoracolumbar spinal fusion: a systematic review and meta-analysis of comparative studies. Spine (Phila Pa 1976). 2018. 10.1097/BRS.0000000000002608. - PubMed
Publication types
MeSH terms
Substances
LinkOut - more resources
Full Text Sources
Other Literature Sources
Miscellaneous

