Predeployment predictors of psychiatric disorder-symptoms and interpersonal violence during combat deployment
- PMID: 30102442
- PMCID: PMC6212319
- DOI: 10.1002/da.22807
Predeployment predictors of psychiatric disorder-symptoms and interpersonal violence during combat deployment
Abstract
Background: Preventing suicides, mental disorders, and noncombat-related interpersonal violence during deployment are priorities of the US Army. We used predeployment survey and administrative data to develop actuarial models to identify soldiers at high risk of these outcomes during combat deployment.
Methods: The models were developed in the Army Study to Assess Risk and Resilience in Servicemembers (Army STARRS) Pre-Post Deployment Study, a panel study of soldiers deployed to Afghanistan in 2012-2013. Soldiers completed self-administered questionnaires before deployment and one (T1), three (T2), and nine months (T3) after deployment, and consented to administrative data linkage. Seven during-deployment outcomes were operationalized using the postdeployment surveys. Two overlapping samples were used because some outcomes were assessed at T1 (n = 7,048) and others at T2-T3 (n = 7,081). Ensemble machine learning was used to develop a model for each outcome from 273 predeployment predictors, which were compared to simple logistic regression models.
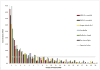
Results: The relative improvement in area under the receiver operating characteristic curve (AUC) obtained by machine learning compared to the logistic models ranged from 1.11 (major depression) to 1.83 (suicidality).The best-performing machine learning models were for major depression (AUC = 0.88), suicidality (0.86), and generalized anxiety disorder (0.85). Roughly 40% of these outcomes occurred among the 5% of soldiers with highest predicted risk.
Conclusions: Actuarial models could be used to identify high risk soldiers either for exclusion from deployment or preventive interventions. However, the ultimate value of this approach depends on the associated costs, competing risks (e.g. stigma), and the effectiveness to-be-determined interventions.
Keywords: army; deployment; mental disorder; military; predictive modeling; risk assessment; violence.
© 2018 Wiley Periodicals, Inc.
Conflict of interest statement
Figures
References
-
- Afifi TO, Taillieu T, Zamorski MA, Turner S, Cheung K, Sareen J. Association of child abuse exposure with suicidal ideation, suicide plans, and suicide attempts in military personnel and the general population in Canada. JAMA Psychiatry. 2016;73(3):229–238. - PubMed
-
- Bliese PD, Thomas JL, McGurk D, McBride S, Castro CA. Mental health advisory teams: a proactive examination of mental health during combat deployments. International Review of Psychiatry. 2011;23(2):127–134. - PubMed
-
- Booth-Kewley S, Highfill-McRoy RM, Larson GE, Garland CF, Gaskin TA. Anxiety and depression in Marines sent to war in Iraq and Afghanistan. Journal of Nervous and Mental Disease. 2012;200(9):749–757. - PubMed
-
- Breiman L. Random forests. Machine Learning. 2001;45(1):5–32.
-
- Buntrock C, Ebert DD, Lehr D, Smit F, Riper H, Berking M, Cuijpers P. Effect of a web-based guided self-help intervention for prevention of major depression in adults with subthreshold depression: a randomized clinical trial. JAMA. 2016;315(17):1854–1863. - PubMed
Publication types
MeSH terms
Grants and funding
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical