Germs of thrones - spontaneous decolonization of Carbapenem-Resistant Enterobacteriaceae (CRE) and Vancomycin-Resistant Enterococci (VRE) in Western Europe: is this myth or reality?
- PMID: 30123500
- PMCID: PMC6090624
- DOI: 10.1186/s13756-018-0390-5
Germs of thrones - spontaneous decolonization of Carbapenem-Resistant Enterobacteriaceae (CRE) and Vancomycin-Resistant Enterococci (VRE) in Western Europe: is this myth or reality?
Abstract
Background: In France, Carbapenem-Resistant Enterobacteriaceae (CRE) and Vancomycin-Resistant Enterococci (VRE) are considered as Extensively Drug-Resistant (XDR) bacteria. Their management requires reinforcement of hospital's hygiene policies, and currently there is few consistent data concerning the spontaneous decolonization in XDR colonized patients. Our aim is to study the natural history of decolonization of XDR carriers over time in a hospital setting in a low prevalence country.
Material and methods: Retrospective multicenter study over 2 years (2015-2016) in 2 different tertiary care hospital sites and units having an agreement for permanent cohorting of such XDR carriers. We gathered the type of microorganisms, risk factors for colonization and rectal swabs from patient's follow-up. We also evaluated patient care considering isolation precautions.
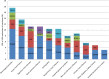
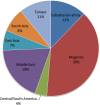
Results: We included 125 patients, aged 63+/-19y, including 72.8% of CRE (n = 91), 24.8% of VRE (n = 31) and 2.4% (n = 3) co-colonized with CRE and VRE. CRE were mainly E. coli (n = 54), K. pneumoniae (n = 51) and E. cloacae (n = 6). Mechanisms of resistance were mainly OXA-48 (n = 69), NDM-1 (n = 11), OXA-232 (n = 8) and KPC (n = 3).Prior antibiotic therapy was reported in 38.4% (n = 48) of cases. Conversely, 17.6% (n = 22) received antibiotics during follow-up.Spontaneous decolonization occurred within the first 30 days in 16.4% (n = 19/116) of cases and up to 48.2% after day-90 with a median follow-up of 96 days (0-974).We estimated that XDR carriage was associated with a larger care burden in 13.6% (n = 17) of cases, especially due to a prolongation of hospitalization of 32.5 days (15-300).
Conclusions: Our study shows that spontaneous decolonization is increasing over time (up to 48.2%). We can regret that only few patients underwent screening after 1 year, emphasizing the need for more monitoring and prospective studies.
Keywords: Carbapenem-Resistant Enterobacteriaceae; Decolonization; Vancomycin-Resistant Enterococcus.
Conflict of interest statement
Not required; as part as routine care, all procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki Declaration and its later amendments or comparable ethical standards. Not applicable. As a retrospective study, no consent was required. The authors declare that they have no competing interests. Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Figures
References
-
- Gutiérrez-Gutiérrez B, Sojo-Dorado J, Bravo-Ferrer J, Cuperus N, de Kraker M, Kostyanev T, et al. EUropean prospective cohort study on Enterobacteriaceae showing REsistance to CArbapenems (EURECA): a protocol of a European multicentre observational study. BMJ Open. 2017;7:e015365. doi: 10.1136/bmjopen-2016-015365. - DOI - PMC - PubMed
-
- Mouloudi E, Protonotariou E, Zagorianou A, Iosifidis E, Karapanagiotou A, Giasnetsova T, et al. Bloodstream Infections Caused by Metallo-β-Lactamase/Klebsiella pneumoniae Carbapenemase–Producing K. pneumoniae among Intensive Care Unit Patients in Greece: Risk Factors for Infection and Impact of Type of Resistance on Outcomes. Infect Control Hosp Epidemiol. 2010;31:1250–1256. doi: 10.1086/657135. - DOI - PubMed
-
- Centers for Disease Control and Prevention (CDC) Guidance for control of infections with carbapenem-resistant or carbapenemase-producing Enterobacteriaceae in acute care facilities. MMWR Morb Mortal Wkly Rep. 2009;58:256–260. - PubMed
Publication types
MeSH terms
Substances
Grants and funding
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical