Serum Angiopoietin-2 Predicts Mortality and Kidney Outcomes in Decompensated Cirrhosis
- PMID: 30141205
- PMCID: PMC6351209
- DOI: 10.1002/hep.30230
Serum Angiopoietin-2 Predicts Mortality and Kidney Outcomes in Decompensated Cirrhosis
Abstract
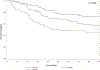
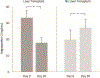
Acute kidney injury in decompensated cirrhosis has limited therapeutic options, and novel mechanistic targets are urgently needed. Angiopoietin-2 is a context-specific antagonist of Tie2, a receptor that signals vascular quiescence. Considering the prominence of vascular destabilization in decompensated cirrhosis, we evaluated Angiopoietin-2 to predict clinical outcomes. Serum Angiopoietin-2 was measured serially in a prospective cohort of hospitalized patients with decompensated cirrhosis and acute kidney injury. Clinical characteristics and outcomes were examined over a 90-day period and analyzed according to Angiopoietin-2 levels. Primary outcome was 90-day mortality. Our study included 191 inpatients (median Angiopoietin-2 level 18.2 [interquartile range 11.8, 26.5] ng/mL). Median Model for End-Stage Liver Disease (MELD) score was 23 [17, 30] and 90-day mortality was 41%. Increased Angiopoietin-2 levels were associated with increased mortality (died 21.9 [13.9, 30.3] ng/mL vs. alive 15.2 [9.8, 23.0] ng/mL; P < 0.001), higher Acute Kidney Injury Network stage (stage I 13.4 [9.8, 20.1] ng/mL vs. stage II 20.0 [14.1, 26.2] ng/mL vs. stage III 21.9 [13.0, 29.5] ng/mL; P = 0.002), and need for renal replacement therapy (16.5 [11.3, 23.6] ng/mL vs. 25.1 [13.3, 30.3] ng/mL; P = 0.005). The association between Angiopoietin-2 and mortality was significant in unadjusted and adjusted Cox regression models (P ≤ 0.001 for all models), and improved discrimination for mortality when added to MELD score (integrated discrimination increment 0.067; P = 0.001). Conclusion: Angiopoietin-2 was associated with mortality and other clinically relevant outcomes in a cohort of patients with decompensated cirrhosis with acute kidney injury. Further experimental study of Angiopoietin/Tie2 signaling is warranted to explore its potential mechanistic and therapeutic role in this population.
© 2018 by the American Association for the Study of Liver Diseases.
Conflict of interest statement
Figures
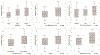

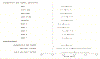
Similar articles
-
Siglec-7 as a Novel Biomarker to Predict Mortality in Decompensated Cirrhosis and Acute Kidney Injury.Dig Dis Sci. 2016 Dec;61(12):3609-3620. doi: 10.1007/s10620-016-4316-x. Epub 2016 Sep 21. Dig Dis Sci. 2016. PMID: 27655105 Free PMC article.
-
Admission plasma uromodulin and the risk of acute kidney injury in hospitalized patients with cirrhosis: a pilot study.Am J Physiol Gastrointest Liver Physiol. 2019 Oct 1;317(4):G447-G452. doi: 10.1152/ajpgi.00158.2019. Epub 2019 Aug 14. Am J Physiol Gastrointest Liver Physiol. 2019. PMID: 31411505 Free PMC article.
-
Angiopoietin-2 in acute liver failure.Crit Care Med. 2012 May;40(5):1499-505. doi: 10.1097/CCM.0b013e318241e34e. Crit Care Med. 2012. PMID: 22430236
-
Circulating Angiopoietin-2 levels predict mortality in kidney transplant recipients: a 4-year prospective case-cohort study.Transpl Int. 2014 Jun;27(6):541-52. doi: 10.1111/tri.12293. Epub 2014 Mar 24. Transpl Int. 2014. PMID: 24628855
-
The clinical value of angiopoietin-2 in liver diseases.Clin Liver Dis (Hoboken). 2022 Jul 1;19(6):244-247. doi: 10.1002/cld.1218. eCollection 2022 Jun. Clin Liver Dis (Hoboken). 2022. PMID: 36619892 Free PMC article. Review.
Cited by
-
Exploring Angiopoietin-2: Clinical Insights and Experimental Perspectives in Kidney Diseases.Kidney Int Rep. 2024 Sep 6;9(12):3375-3385. doi: 10.1016/j.ekir.2024.09.001. eCollection 2024 Dec. Kidney Int Rep. 2024. PMID: 39698365 Free PMC article. Review.
-
HCV and HCC Tango-Deciphering the Intricate Dance of Disease: A Review Article.Int J Mol Sci. 2023 Nov 7;24(22):16048. doi: 10.3390/ijms242216048. Int J Mol Sci. 2023. PMID: 38003240 Free PMC article. Review.
-
Development and validation of a nomogram for predicting all-cause mortality in American adult hypertensive populations.Front Pharmacol. 2023 Nov 22;14:1266870. doi: 10.3389/fphar.2023.1266870. eCollection 2023. Front Pharmacol. 2023. PMID: 38074152 Free PMC article.
-
Serum Angiopoietin-2 Predicts the Occurrence and Recurrence of Hepatocellular Carcinoma after Direct-Acting Antiviral Therapy for Hepatitis C.Viruses. 2023 Jan 7;15(1):181. doi: 10.3390/v15010181. Viruses. 2023. PMID: 36680221 Free PMC article.
-
Ipragliflozin Ameliorates Endoplasmic Reticulum Stress and Apoptosis through Preventing Ectopic Lipid Deposition in Renal Tubules.Int J Mol Sci. 2019 Dec 26;21(1):190. doi: 10.3390/ijms21010190. Int J Mol Sci. 2019. PMID: 31888083 Free PMC article.
References
-
- Angeli P, Gines P, Wong F, et al. Diagnosis and management of acute kidney injury in patients with cirrhosis: revised consensus recommendations of the International Club of Ascites. Gut 2015;64:531–7. - PubMed
-
- Gines P, Schrier RW. Renal failure in cirrhosis. The New England journal of medicine 2009;361:1279–90. - PubMed
-
- Schrier RW, Arroyo V, Bernardi M, Epstein M, Henriksen JH, Rodes J. Peripheral arterial vasodilation hypothesis: a proposal for the initiation of renal sodium and water retention in cirrhosis. Hepatology (Baltimore, Md) 1988;8:1151–7. - PubMed
-
- Nazar A, Pereira GH, Guevara M, et al. Predictors of response to therapy with terlipressin and albumin in patients with cirrhosis and type 1 hepatorenal syndrome. Hepatology (Baltimore, Md) 2010;51:219–26. - PubMed
-
- Boyer TD, Sanyal AJ, Wong F, et al. Terlipressin Plus Albumin Is More Effective Than Albumin Alone in Improving Renal Function in Patients With Cirrhosis and Hepatorenal Syndrome Type 1. Gastroenterology 2016. - PubMed
Publication types
MeSH terms
Substances
Grants and funding
- K24 DK078772/DK/NIDDK NIH HHS/United States
- R01 DK095072/DK/NIDDK NIH HHS/United States
- P30 DK043351/DK/NIDDK NIH HHS/United States
- American College of Gastroenterology/International
- R35 HL139424/HL/NHLBI NIH HHS/United States
- R35-HL139424/GF/NIH HHS/United States
- R01 HL093234/HL/NHLBI NIH HHS/United States
- 18CDA34110131/American Heart Association Career Development/International
- R01 HL125275/HL/NHLBI NIH HHS/United States
- 15FTF25980003/American Heart Association's NCRP Winter Fellow-to-Faculty Transition/International
- R01 DK094486/DK/NIDDK NIH HHS/United States
- K23 DK106479/DK/NIDDK NIH HHS/United States
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical
Miscellaneous

