Myeloperoxidase Inhibition Improves Ventricular Function and Remodeling After Experimental Myocardial Infarction
- PMID: 30167547
- PMCID: PMC6113523
- DOI: 10.1016/j.jacbts.2016.09.004
Myeloperoxidase Inhibition Improves Ventricular Function and Remodeling After Experimental Myocardial Infarction
Abstract
PF-1355 is an oral myeloperoxidase (MPO) inhibitor that successfully decreased elevated MPO activity in mouse myocardial infarction models. Short duration PF-1355 treatment for 7 days decreased the number of inflammatory cells and attenuated left ventricular dilation. Cardiac function and remodeling improved when treatment was increased to 21 days. Better therapeutic effect was further achieved with early compared with delayed treatment initiation (1 h vs. 24 h after infarction). In conclusion, PF-1355 treatment protected a mouse heart from acute and chronic effects of MI, and this study paves the way for future translational studies investigating this class of drugs in cardiovascular diseases.
Keywords: CNR, contrast to noise ratio; EDV, end-diastolic volume; EF, ejection fraction; IRI, ischemia reperfusion injury; LAR, lesion activation ratio; Ly-6C, lymphocyte antigen 6C; MI, myocardial infarction; MPO, myeloperoxidase; MPO-Gd, bis-5-hydroxytryptamide-diethylenetriaminepentaacetate-gadolinium; MPO−/−, myeloperoxidase knock out; inflammation; myeloperoxidase; myocardial infarction; oxidative stress; treatment.
Figures



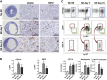



References
-
- Sutton M.G., Sharpe N. Left ventricular remodeling after myocardial infarction: pathophysiology and therapy. Circulation. 2000;101:2981–2988. - PubMed
-
- Gajarsa J., Kloner R. Left ventricular remodeling in the post-infarction heart: a review of cellular, molecular mechanisms, and therapeutic modalities. Heart Fail Rev. 2011;16:13–21. - PubMed
-
- Solomon S.D., Zelenkofske S., McMurray J.J.V. Sudden death in patients with myocardial infarction and left ventricular dysfunction, heart failure, or both. N Engl J Med. 2005;352:2581–2588. - PubMed
Publication types
LinkOut - more resources
Full Text Sources
Other Literature Sources
Research Materials
Miscellaneous

