Association of Lymph Node Count and Overall Survival in Node-Negative Endometrial Cancers
- PMID: 30175315
- PMCID: PMC6115200
- DOI: 10.1200/CCI.16.00064
Association of Lymph Node Count and Overall Survival in Node-Negative Endometrial Cancers
Abstract
Purpose: To estimate whether the number of lymph nodes removed during surgery is associated with overall survival among women with endometrial cancer.
Methods: We performed a retrospective cohort study of women with node-negative, stage I to IIIB endometrial cancer (n = 152,702) identified from the 1998-2011 National Cancer Database. Multivariable Cox proportional hazards regression tested for an association of lymph node count with survival. Restricted mean survival and relative hazard curves were plotted for survival as a function of number of removed lymph nodes.
Results: Among women with node-negative endometrioid endometrial cancer, for each additional five lymph nodes removed, the hazard for death decreased: stage I, the hazard ratio (HR) was 0.95 (95% CI, 0.93 to 0.97; P < .001), stage II, HR was 0.90 (95% CI, 0.87 to 0.94; P < .001); and stage IIIA-B, HR was 0.92 (95% CI, 0.88 to 0.96; P < .001). When grouped by grade, each additional five lymph nodes removed was also associated with decreased hazard for death: grade 1, HR was 0.96 (95% CI, 0.93 to 0.99; P = .009); grade 2,HR was0.91 (95%CI, 0.89 to0.94; P <.001);and grade 3,HR was 0.95 (95%CI, 0.92 to 0.97; P <.001). Increased lymph node dissection was also associated with increased survival among women with node-negative stage II (HR, 0.92; 95% CI, 0.86 to 0.98; P = .01) or stage IIIA-B (HR, 0.94; 95% CI, 0.89 to 0.99; P = .025) uterine serous carcinoma, but not among women with carcinosarcoma or clear cell adeno-carcinoma. Five-year survival for women with one to four nodes removed and endometrioid or serous histology was 85% (95% CI, 84% to 85%) and 54% (95% CI, 50% to 59%), respectively. Five-year survival was significantly higher for women with ≥ 20 removed nodes and endometrioid (91%; 95% CI, 90% to 91%) or serous (72%; 95% CI, 68% to 76%) histology (P < .001).
Conclusion: Increased lymph node count is associated with a 1% to 14% decreased hazard of death per each additional five lymph nodes removed and a 5% to 20% increased 5-year survival among women with pathologically node-negative endometrioid and serous endometrial cancers.
Figures
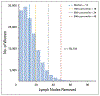


Similar articles
-
The prognostic significance of aortic lymph node metastasis in endometrial cancer: Potential implications for selective aortic lymph node assessment.Gynecol Oncol. 2019 Jun;153(3):505-510. doi: 10.1016/j.ygyno.2019.03.251. Epub 2019 Mar 30. Gynecol Oncol. 2019. PMID: 30935714 Free PMC article.
-
Survival implications of staging lymphadenectomy for non-endometrioid endometrial cancers.Gynecol Oncol. 2018 Jun;149(3):531-538. doi: 10.1016/j.ygyno.2018.03.046. Epub 2018 Mar 17. Gynecol Oncol. 2018. PMID: 29559170
-
Extent of lymph node dissection and overall survival in patients with uterine carcinosarcoma, papillary serous and endometrioid adenocarcinoma: A retrospective cohort study.Int J Surg. 2015 Dec;24(Pt A):9-13. doi: 10.1016/j.ijsu.2015.10.006. Epub 2015 Oct 22. Int J Surg. 2015. PMID: 26476418
-
Pelvic lymph node count is an important prognostic variable for FIGO stage I and II endometrial carcinoma with high-risk histology.Gynecol Oncol. 2006 Jul;102(1):92-7. doi: 10.1016/j.ygyno.2005.11.032. Epub 2006 Jan 10. Gynecol Oncol. 2006. PMID: 16406063
-
Sentinel lymph node biopsy in high-grade endometrial cancer: a systematic review and meta-analysis of performance characteristics.Am J Obstet Gynecol. 2021 Oct;225(4):367.e1-367.e39. doi: 10.1016/j.ajog.2021.05.034. Epub 2021 May 29. Am J Obstet Gynecol. 2021. PMID: 34058168
Cited by
-
Prognostic factors of endometrial cancer in elderly patient group and their effects on survival.North Clin Istanb. 2021 Jan 14;8(4):345-353. doi: 10.14744/nci.2020.47154. eCollection 2021. North Clin Istanb. 2021. PMID: 34585068 Free PMC article.
-
Impact of Para-Aortic Lymphadenectomy on Clinically FIGO Stage IIIC1 High-Grade Endometrial Cancer: A Retrospective Cohort Study from Two Tertiary Centers in Korea and Taiwan.Medicina (Kaunas). 2025 Jun 12;61(6):1079. doi: 10.3390/medicina61061079. Medicina (Kaunas). 2025. PMID: 40572767 Free PMC article.
-
Robot-Assisted versus Laparoscopic Surgery for Pelvic Lymph Node Dissection in Patients with Gynecologic Malignancies.Gynecol Minim Invasive Ther. 2023 Dec 7;13(1):37-42. doi: 10.4103/gmit.gmit_9_23. eCollection 2024 Jan-Mar. Gynecol Minim Invasive Ther. 2023. PMID: 38487615 Free PMC article.
References
-
- Creasman WT, Morrow CP, Bundy BN, et al.: Surgical pathologic spread patterns of endometrial cancer. A Gynecologic Oncology Group Study. Cancer 60:2035–2041, 1987 - PubMed
-
- Abu-Rustum NR, Gomez JD, Alektiar KM, et al.: The incidence of isolated paraaortic nodal metastasis in surgically staged endometrial cancer patients with negative pelvic lymph nodes. Gynecol Oncol 115:236–238, 2009 - PubMed
-
- Benedetti Panici P, Basile S, Maneschi F, et al.: Systematic pelvic lymphadenectomy vs. no lymphadenectomy in early-stage endometrial carcinoma: Randomized clinical trial. J Natl Cancer Inst 100:1707–1716, 2008 - PubMed
Grants and funding
LinkOut - more resources
Full Text Sources
Other Literature Sources

