Advancing Age and Comorbidity in a US Insured Population-Based Cohort of Patients With Chronic Hepatitis B
- PMID: 30175482
- PMCID: PMC6593449
- DOI: 10.1002/hep.30246
Advancing Age and Comorbidity in a US Insured Population-Based Cohort of Patients With Chronic Hepatitis B
Abstract
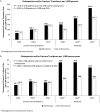
Chronic hepatitis B (CHB) comorbidity data are limited. Using insurance claims databases, our aims were to determine the prevalence and incidence of nonliver comorbidities in CHB patients over time and the predictors of select comorbidities in CHB patients. Patients were adults with continuous coverage (commercial/Medicare or Medicaid) 6 months prior to and after the first CHB diagnosis and matched non-CHB patients. Deyo-Charlson Comorbidity Index (DCCI) and comorbidities were analyzed (cardiovascular disease [CVD], carcinoma, diabetes mellitus [DM], obesity, hypertension [HTN], hyperlipidemia, alcohol use, renal impairment, chronic kidney disease [CKD], and osteoporosis/fracture [OF]). The study population included 44,026 CHB cases and 121,568 matched controls. CHB patient mean age increased from 48.1 ± 11.9 years in 2006 to 51.8 ± 12.4 years in 2015 for commercial/Medicare and from 44.1 ± 11.1 years to 50.2 ± 10.2 years for Medicaid (P < 0.001 for both). The Medicaid CHB cohort was the sickest (DCCI, 2.6, P < 0.001). The commercial/Medicare 2006 CKD prevalence rate was 36.1/1,000 in CHB patients and 10.2/1,000 in controls, increasing to 97.6 and 38.8 in 2015, respectively. The 2006 CKD incidence (per 1,000 person-years) was 10.3 and 4.8 and 15.2 and 11.3 by 2015, respectively (P < 0.05 for all). The strongest predictors for CKD were DM (hazard ratio [HR], 2.48), HTN (HR, 3.29), and CVD (HR, 2.61) (all P < 0.0001). Similar prevalence and incidence changes were observed for OF. The strongest predictors for OF were female gender (HR, 2.22), alcohol use (HR, 2.02), and viral coinfection (HR, 1.37) (all P < 0.0001). Conclusion: Insured CHB patients were older, had more comorbidities, and experienced higher incidence and prevalence of CKD and OF than controls.
© 2018 The Authors. Hepatology published by Wiley Periodicals, Inc., on behalf of the American Association for the Study of Liver Diseases.
Figures


Comment in
-
Letter to the Editor: Hip Fracture Risk in Patients With Cirrhosis: Does Diabetes Mellitus Matter?Hepatology. 2020 Apr;71(4):1518-1519. doi: 10.1002/hep.30566. Epub 2020 Mar 29. Hepatology. 2020. PMID: 30761561 No abstract available.
-
Reply.Hepatology. 2020 Apr;71(4):1519. doi: 10.1002/hep.30560. Epub 2020 Mar 29. Hepatology. 2020. PMID: 30762889 No abstract available.
References
-
- World Health Organization . Global Hepatitis Report, 2017. Geneva, Switzerland: World Health Organization; 2017.
-
- Cholankeril G, Perumpail RB, Hu M, Skowron G, Younossi ZM, Ahmed A. Chronic hepatitis B is associated with higher inpatient resource utilization and mortality versus chronic hepatitis C. Dig Dis Sci 2016;61:2505‐2515. - PubMed
-
- Cox N, Tillmann H. Emerging pipeline drugs for hepatitis B infection. Expert Opin Emerg Drugs 2011;16:713‐729. - PubMed
Publication types
MeSH terms
Grants and funding
LinkOut - more resources
Full Text Sources
Other Literature Sources
Research Materials

