Impact of potentially variable RBE in liver proton therapy
- PMID: 30183674
- PMCID: PMC6207451
- DOI: 10.1088/1361-6560/aadf24
Impact of potentially variable RBE in liver proton therapy
Abstract
Currently, the relative biological effectiveness (RBE) is assumed to be constant with a value of 1.1 in proton therapy. Although trends of RBE variations are well known, absolute values in patients are associated with considerable uncertainties. This study aims to evaluate the impact of a variable proton RBE in proton therapy liver trials using different fractionation schemes. Sixteen liver cancer cases were evaluated assuming two clinical schedules of 40 Gy/5 fractions and 58.05 Gy/15 fractions. The linear energy transfer (LET) and physical dose distribution in patients were simulated using Monte Carlo. The variable RBE distribution was calculated using a phenomenological model, considering the influence of the LET, fraction size and α/β value. Further, models to predict normal tissue complication probability (NTCP) and tumor control probability (TCP) were used to investigate potential RBE effects on outcome predictions. Applying the variable RBE model to the 5 and 15 fractions schedules results in an increase in mean fraction-size equivalent dose (FED) to the normal liver of 5.0% and 9.6% respectively. For patients with a mean FED to the normal liver larger than 29.8 Gy, this results in a non-negligible increase in the predicted NTCP of the normal liver averaging 11.6%, ranging from 2.7% to 25.6%. On the other hand, decrease in TCP was less than 5% for both fractionation regimens for all patients when assuming a variable RBE instead of constant. Consequently, the difference in TCP between the two fractionation schedules did not change significantly assuming a variable RBE while the impact on the NTCP difference was highly case specific. In addition, both the NTCP and TCP decrease with increasing α/β value for both fractionation schemes, with the decreases being more pronounced when using a variable RBE compared to using RBE = 1.1. Assuming a constant RBE of 1.1 most likely overestimates the therapeutic ratio in proton therapy for liver cancer, predominantly due to underestimation of the RBE-weighted dose to the normal liver. The impact of applying a variable RBE (as compared to RBE = 1.1) on the NTCP difference of the two fractionation regimens is case dependent. A variable RBE results in a slight increase in TCP difference. Variations in patient radiosensitivity increase when using a variable RBE.
Figures


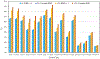




Similar articles
-
Inclusion of a variable RBE into proton and photon plan comparison for various fractionation schedules in prostate radiation therapy.Med Phys. 2017 Mar;44(3):810-822. doi: 10.1002/mp.12117. Med Phys. 2017. PMID: 28107554
-
Relating the proton relative biological effectiveness to tumor control and normal tissue complication probabilities assuming interpatient variability in α/β.Acta Oncol. 2017 Nov;56(11):1379-1386. doi: 10.1080/0284186X.2017.1371325. Epub 2017 Sep 18. Acta Oncol. 2017. PMID: 28918679
-
Applying a variable relative biological effectiveness (RBE) might affect the analysis of clinical trials comparing photon and proton therapy for prostate cancer.Phys Med Biol. 2019 Jun 5;64(11):115027. doi: 10.1088/1361-6560/ab2144. Phys Med Biol. 2019. PMID: 31082810
-
Relative biological effectiveness (RBE) values for proton beam therapy. Variations as a function of biological endpoint, dose, and linear energy transfer.Phys Med Biol. 2014 Nov 21;59(22):R419-72. doi: 10.1088/0031-9155/59/22/R419. Epub 2014 Oct 31. Phys Med Biol. 2014. PMID: 25361443 Review.
-
Relative Biological Effectiveness Uncertainties and Implications for Beam Arrangements and Dose Constraints in Proton Therapy.Semin Radiat Oncol. 2018 Jun;28(3):256-263. doi: 10.1016/j.semradonc.2018.02.010. Semin Radiat Oncol. 2018. PMID: 29933885 Review.
Cited by
-
Roadmap: proton therapy physics and biology.Phys Med Biol. 2021 Feb 26;66(5):10.1088/1361-6560/abcd16. doi: 10.1088/1361-6560/abcd16. Phys Med Biol. 2021. PMID: 33227715 Free PMC article. Review.
-
NRG Oncology White Paper on the Relative Biological Effectiveness in Proton Therapy.Int J Radiat Oncol Biol Phys. 2025 Jan 1;121(1):202-217. doi: 10.1016/j.ijrobp.2024.07.2152. Epub 2024 Jul 25. Int J Radiat Oncol Biol Phys. 2025. PMID: 39059509 Review.
-
Proton RBE dependence on dose in the setting of hypofractionation.Br J Radiol. 2020 Mar;93(1107):20190291. doi: 10.1259/bjr.20190291. Epub 2019 Aug 28. Br J Radiol. 2020. PMID: 31437004 Free PMC article. Review.
-
Exploring Helium Ions' Potential for Post-Mastectomy Left-Sided Breast Cancer Radiotherapy.Cancers (Basel). 2024 Jan 18;16(2):410. doi: 10.3390/cancers16020410. Cancers (Basel). 2024. PMID: 38254899 Free PMC article.
-
Comparing Predicted Toxicities between Hypofractionated Proton and Photon Radiotherapy of Liver Cancer Patients with Different Adaptive Schemes.Cancers (Basel). 2023 Sep 15;15(18):4592. doi: 10.3390/cancers15184592. Cancers (Basel). 2023. PMID: 37760560 Free PMC article.
References
-
- Agostinelli S, Allison J, Amako KA, Apostolakis J, Araujo H, Arce P,… & Behner F (2003). GEANT4—a simulation toolkit. Nuclear instruments and methods in physics research section A: Accelerators, Spectrometers, Detectors and Associated Equipment, 506(3), 250–303.
-
- Boda-Heggemann J, Attenberger U, Budjan J, Jahnke A, Jahnke L, Vogel L, … & Lohr F (2016). MRI morphologic alterations after liver SBRTMR-morphologische Veränderungen nach Leber-SBRT. Strahlentherapie und Onkologie, 192(9), 641–648. - PubMed
-
- Carabe-Femandez A, & Paganetti H (2011). Clinical consequences of relative biological effectiveness (RBE) variations in proton radiotherapy of the prostate, brain, and liver. International Journal of Radiation Oncology• Biology• Physics, 81(2), S725–S726. - PubMed
-
- Chadwick KH, & Leenhouts HP (1973). A molecular theory of cell survival. Physics in Medicine & Biology, 18(1), 78. - PubMed
-
- Dawson LA, Biersack M, Lockwood G, Eisbruch A, Lawrence TS, & Ten Haken RK (2005). Use of principal component analysis to evaluate the partial organ tolerance of normal tissues to radiation. International Journal of Radiation Oncology• Biology• Physics, 62(3), 829–837. - PubMed
Publication types
MeSH terms
Substances
Grants and funding
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical
