A Dietary Assessment App for Hospitalized Patients at Nutritional Risk: Development and Evaluation of the MyFood App
- PMID: 30194059
- PMCID: PMC6231855
- DOI: 10.2196/mhealth.9953
A Dietary Assessment App for Hospitalized Patients at Nutritional Risk: Development and Evaluation of the MyFood App
Abstract
Background: Disease-related malnutrition is a common challenge among hospitalized patients. There seems to be a lack of an effective system to follow-up nutritional monitoring and treatment of patients at nutritional risk after risk assessment. We identify a need for a more standardized system to prevent and treat disease-related malnutrition.
Objective: We aimed to develop a dietary assessment app for tablets for use in a hospital setting and to evaluate the app's ability to measure individual intake of energy, protein, liquid, and food and beverage items among hospitalized patients for two days. We also aimed to measure patients' experiences using the app.
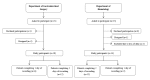
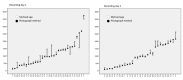
Methods: We have developed the MyFood app, which consists of three modules: 1) collection of information about the patient, 2) dietary assessment function, and 3) evaluation of recorded intake compared to individual needs. We used observations from digital photography of the meals, combined with partial weighing of the meal components, as a reference method to evaluate the app's dietary assessment system for two days. Differences in the intake estimations of energy, protein, liquid, and food and beverage items between MyFood and the photograph method were analyzed on both group and individual level.
Results: Thirty-two patients hospitalized at Oslo University Hospital were included in the study. The data collection period ran from March to May 2017. About half of the patients had ≥90% agreement between MyFood and the photograph method for energy, protein, and liquid intake on both recording days. Dinner was the meal with the lowest percent agreement between methods. MyFood overestimated patients' intake of bread and cereals and underestimated fruit consumption. Agreement between methods increased from day 1 to day 2 for bread and cereals, spreads, egg, yogurt, soup, hot dishes, and desserts. Ninety percent of participants reported that MyFood was easy to use, and 97% found the app easy to navigate.
Conclusions: We developed the MyFood app as a tool to monitor dietary intake among hospitalized patients at nutritional risk. The recorded intake of energy, protein, and liquid using MyFood showed good agreement with the photograph method for the majority of participants. The app's ability to estimate intake within food groups was good, except for bread and cereals which were overestimated and fruits which were underestimated. The app was well accepted among study participants and has the potential to be a dietary assessment tool for use among patients in clinical practice.
Keywords: decision support system; dietary assessment; disease-related malnutrition; eHealth; mHealth; validation study.
©Mari Mohn Paulsen, Martina Lovise Lindhart Hagen, Marte Hesvik Frøyen, Rikke Julie Foss-Pedersen, Dagfinn Bergsager, Randi Julie Tangvik, Lene Frost Andersen. Originally published in JMIR Mhealth and Uhealth (http://mhealth.jmir.org), 07.09.2018.
Conflict of interest statement
Conflicts of Interest: None declared.
Figures



References
-
- Agarwal E, Ferguson M, Banks M, Batterham M, Bauer J, Capra S, Isenring E. Malnutrition and poor food intake are associated with prolonged hospital stay, frequent readmissions, and greater in-hospital mortality: results from the Nutrition Care Day Survey 2010. Clin Nutr. 2013 Oct;32(5):737–45. doi: 10.1016/j.clnu.2012.11.021.S0261-5614(12)00269-5 - DOI - PubMed
-
- Sorensen J, Kondrup J, Prokopowicz J, Schiesser M, Krähenbühl L, Meier R, Liberda M, EuroOOPS study group EuroOOPS: an international, multicentre study to implement nutritional risk screening and evaluate clinical outcome. Clin Nutr. 2008 Jun;27(3):340–9. doi: 10.1016/j.clnu.2008.03.012.S0261-5614(08)00067-8 - DOI - PubMed
LinkOut - more resources
Full Text Sources
Other Literature Sources
Molecular Biology Databases
Miscellaneous

