Relative Clinical and Cost Burden of Community-Acquired Pneumonia Hospitalizations in Older Adults in the United States-A Cross-Sectional Analysis
- PMID: 30200286
- PMCID: PMC6161150
- DOI: 10.3390/vaccines6030059
Relative Clinical and Cost Burden of Community-Acquired Pneumonia Hospitalizations in Older Adults in the United States-A Cross-Sectional Analysis
Abstract
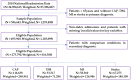
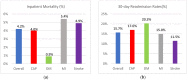
The relative burden of community-acquired pneumonia (CAP) in older adults (≥65 years old) compared to other serious diseases is important to prioritize preventive treatment. A retrospective analysis was conducted using the 2014 National Readmission Database to evaluate the length of stay, inpatient mortality, 30-day readmissions, and costs of CAP compared to diabetes mellitus (DM), myocardial infarction (MI), and stroke. 275,790 hospitalizations were analyzed and represented a national estimate of 616,300 hospitalizations, including 269,961 for CAP, 71,284 for DM, 126,946 for MI, and 148,109 for stroke. The mean length of stay in CAP was 5.2 days, which was higher than DM (4.6) and MI (4.3) but similar to stroke (5.6). The inpatient mortality risk was lower for DM (RR: 0.37, 95% CI: 0.29⁻0.46) but higher for MI (RR: 1.67, 95% CI: 1.50⁻1.85) and stroke (RR: 1.67, 95% CI: 1.51⁻1.83). The median costs for CAP ($7282) were higher compared to DM ($6217) but lower compared to MI ($14,802) and stroke ($8772). The 30-day readmission rate was 17% in CAP, which was higher compared to MI (15%) and stroke (11.5%) and lower compared to DM (20.3%). In patients with CAP, disease burden is on par with other serious diseases. CAP should be prioritized for prevention in older adults with strategies such as vaccination and smoking cessation.
Keywords: burden of illness; community-acquired pneumonia; diabetes mellitus; elderly; myocardial infarction; stroke.
Conflict of interest statement
The authors declare no conflict of interest.
Figures

References
-
- 10 Leading Causes of Death by Age Group, United States—2015. [(accessed on 22 August 2017)]; Available online: https://www.cdc.gov/injury/images/lc-charts/leading_causes_of_death_age_....
-
- Kaplan V., Angus D.C., Griffin M.F., Clermont G., Scott W.R., Linde-Zwirble W.T. Hospitalized community-acquired pneumonia in the elderly: Age-and sex-related patterns of care and outcome in the United States. Am. J. Respir. Crit. Care Med. 2002;165:766–772. doi: 10.1164/ajrccm.165.6.2103038. - DOI - PubMed
Grants and funding
LinkOut - more resources
Full Text Sources
Other Literature Sources
Miscellaneous

