Enterohemorrhagic E. coli (EHEC)-Secreted Serine Protease EspP Stimulates Electrogenic Ion Transport in Human Colonoid Monolayers
- PMID: 30200426
- PMCID: PMC6162544
- DOI: 10.3390/toxins10090351
Enterohemorrhagic E. coli (EHEC)-Secreted Serine Protease EspP Stimulates Electrogenic Ion Transport in Human Colonoid Monolayers
Abstract
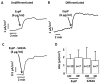
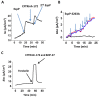
One of the characteristic manifestations of Shiga-toxin-producing Escherichia coli (E. coli) infection in humans, including EHEC and Enteroaggregative E. coli O104:H4, is watery diarrhea. However, neither Shiga toxin nor numerous components of the type-3 secretion system have been found to independently elicit fluid secretion. We used the adult stem-cell-derived human colonoid monolayers (HCM) to test whether EHEC-secreted extracellular serine protease P (EspP), a member of the serine protease family broadly expressed by diarrheagenic E. coli can act as an enterotoxin. We applied the Ussing chamber/voltage clamp technique to determine whether EspP stimulates electrogenic ion transport indicated by a change in short-circuit current (Isc). EspP stimulates Isc in HCM. The EspP-stimulated Isc does not require protease activity, is not cystic fibrosis transmembrane conductance regulator (CFTR)-mediated, but is partially Ca2+-dependent. EspP neutralization with a specific antibody reduces its potency in stimulating Isc. Serine Protease A, secreted by Enteroaggregative E. coli, also stimulates Isc in HCM, but this current is CFTR-dependent. In conclusion, EspP stimulates colonic CFTR-independent active ion transport and may be involved in the pathophysiology of EHEC diarrhea. Serine protease toxins from E. coli pathogens appear to serve as enterotoxins, potentially significantly contributing to watery diarrhea.
Keywords: CFTR; EHEC; SPATEs; diarrhea; human colonoid monolayers; intracellular Ca2+; serine protease EspP; short circuit current.
Conflict of interest statement
The authors declare no conflicts of interest. The funders had no role in the design of the study; in the collection, analyses, or interpretation of data; in the writing of the manuscript, and in the decision to publish the results.
Figures



References
Publication types
MeSH terms
Substances
Grants and funding
LinkOut - more resources
Full Text Sources
Other Literature Sources
Molecular Biology Databases
Miscellaneous

