Are Invasive Procedures Effective for Chronic Pain? A Systematic Review
- PMID: 30204920
- PMCID: PMC6611529
- DOI: 10.1093/pm/pny154
Are Invasive Procedures Effective for Chronic Pain? A Systematic Review
Abstract
Objective: To assess the evidence for the safety and efficacy of invasive procedures for reducing chronic pain and improving function and health-related quality of life compared with sham (placebo) procedures.
Design: Systematic review with meta-analysis.
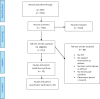
Methods: Studies were identified by searching multiple electronic databases, examining reference lists, and communicating with experts. Randomized controlled trials comparing invasive procedures with identical but otherwise sham procedures for chronic pain conditions were selected. Three authors independently extracted and described study characteristics and assessed Cochrane risk of bias. Two subsets of data on back and knee pain, respectively, were pooled using random-effects meta-analysis. Overall quality of the literature was assessed through Grading of Recommendations, Assessment, Development, and Evaluation.
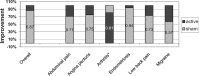
Results: Twenty-five trials (2,000 participants) were included in the review assessing the effect of invasive procedures over sham. Conditions included low back (N = 7 trials), arthritis (4), angina (4), abdominal pain (3), endometriosis (3), biliary colic (2), and migraine (2). Thirteen trials (52%) reported an adequate concealment of allocation. Fourteen studies (56%) reported on adverse events. Of these, the risk of any adverse event was significantly higher for invasive procedures (12%) than sham procedures (4%; risk difference = 0.05, 95% confidence interval [CI] = 0.01 to 0.09, P = 0.01, I2 = 65%). In the two meta-analysis subsets, the standardized mean difference for reduction of low back pain in seven studies (N = 445) was 0.18 (95% CI = -0.14 to 0.51, P = 0.26, I2 = 62%), and for knee pain in three studies (N = 496) it was 0.04 (95% CI = -0.11 to 0.19, P = 0.63, I2 = 36%). The relative contribution of within-group improvement in sham treatments accounted for 87% of the effect compared with active treatment across all conditions.
Conclusions: There is little evidence for the specific efficacy beyond sham for invasive procedures in chronic pain. A moderate amount of evidence does not support the use of invasive procedures as compared with sham procedures for patients with chronic back or knee pain. Given their high cost and safety concerns, more rigorous studies are required before invasive procedures are routinely used for patients with chronic pain.
Keywords: Meta-analysis; Pain; Placebo; Sham; Surgery; Systematic Review.
© 2018 American Academy of Pain Medicine.
Figures

References
-
- Institute of Medicine Committee on Advancing Pain Research. Relieving Pain in America: A Blueprint for Transforming Prevention, Care, Education, and Research. Washington, DC: National Academies Press, National Academy of Sciences; 2011. - PubMed
-
- Hardt J, Jacobsen C, Goldberg J, Nickel R, Buchwald D.. Prevalence of chronic pain in a representative sample in the United States. Pain Med 2008;9(7):803–12. - PubMed
-
- Tsang A, Von Korff M, Lee S, et al. Common chronic pain conditions in developed and developing countries: Gender and age differences and comorbidity with depression-anxiety disorders. J Pain 2008;9(10):883–91. - PubMed
-
- Anastassopoulos KP, Chow W, Tapia CI, et al. Reported side effects, bother, satisfaction, and adherence in patients taking hydrocodone for non-cancer pain. J Opioid Manag 2013;9(2):97–109. - PubMed
Publication types
MeSH terms
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical

