Microthrombotic Renal Vascular Lesions Are Associated to Increased Renal Inflammatory Infiltration in Murine Lupus Nephritis
- PMID: 30210500
- PMCID: PMC6120987
- DOI: 10.3389/fimmu.2018.01948
Microthrombotic Renal Vascular Lesions Are Associated to Increased Renal Inflammatory Infiltration in Murine Lupus Nephritis
Abstract
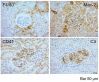
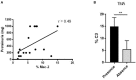
Background: Vascular microthrombotic lesions in lupus nephritis with or without antiphospholipid antibodies may relate to worse renal outcomes. Whether microthrombotic lesions are a consequence of renal inflammation or independently contribute to renal damage is unclear. Our aim was to investigate the relationship between microthrombotic renal vascular lesions and nephritis progression in MRL/lpr mice. Methods: MRL/lpr mice were analyzed for the presence of renal microvascular, glomerular and tubulointerstitial lesions and the effect of anti-aggregation (aspirin or clopidogrel) and dexamethasone on renal clinical and pathological manifestations was evaluated. Intravascular platelet aggregates (CD41), peri- (F4/80), and intraglomerular (Mac-2) macrophage infiltration, and C3 deposition were quantified by immunohistochemistry. Renal function was assessed by measuring proteinuria, and serum levels of creatinine and albumin. Anti-dsDNA and anti-cardiolipin antibodies, and thromboxane B2 levels were quantified by ELISA. Results: Frequency of microthrombotic renal lesions in MRL/lpr mice was high and was associated with immune-mediated renal damage. Proteinuria positively correlated with glomerular macrophage infiltration and was higher in mice with proliferative glomerular lesions. All mice had detectable anti-dsDNA and anti-cardiolipin IgG, regardless the presence of microthrombosis. Proteinuria and glomerular macrophage infiltration were significantly reduced in all treatment groups. Dexamethasone and platelet anti-aggregation similarly reduced glomerular damage and inflammation, but only platelet anti-aggregation significantly reduced anti-cardiolipin antibodies, renal complement deposition and thromboxane B2 levels. Conclusions: Platelet anti-aggregation reduced renal inflammatory damage, renal complement deposition, anti-cardiolipin antibodies, and thromboxane B2 levels and in MRL/lpr mice, suggesting that platelet activation has a pathogenic effect on immune-mediated nephritis. Our results point to MRL/lpr mice with lupus nephritis as an appropriate model to analyze the potential impact of anti-thrombotic intervention on renal inflammation.
Keywords: complement; inflammation; lupus nephritis; macrophages; microthrombosis; platelets.
Figures


References
Publication types
MeSH terms
Substances
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical
Miscellaneous

