Evaluating the Impact of a Feeding Protocol in Neonates before and after Biventricular Cardiac Surgery
- PMID: 30229192
- PMCID: PMC6132815
- DOI: 10.1097/pq9.0000000000000080
Evaluating the Impact of a Feeding Protocol in Neonates before and after Biventricular Cardiac Surgery
Abstract
Introduction: Feeding difficulties and malnutrition are important challenges when caring for newborns with critical congenital heart disease (CCHD) without clear available guidelines for providers. This study describes the utilization of a feeding protocol with the focus on standardization, feeding modality, and total parenteral nutrition (TPN) utilization postoperatively.
Methods: Patients included neonates with CCHD undergoing complex biventricular repair using cardiopulmonary bypass. Data were collected in 2013 preintervention and from 2015 to 2017 postintervention. The feeding protocol outlined guidelines for and postoperative use of TPN. Adverse outcomes data included rates of central line-associated bloodstream infections, necrotizing enterocolitis, chylothorax, and vocal cord dysfunction. Balance outcomes measured were weight for age Z-score at discharge, number of abdominal radiographs obtained, readmission within 90 days, and central venous line utilization.
Results: We included a total of 121 neonates: 49 in the preintervention group and 72 in the postintervention group. The protocol standardized feeding practices in CCHD neonates undergoing surgery with improved compliance from 70% early in the study period to 90% at the end of the study. Infants were fed enterally more preoperatively (86% versus 67%; P = 0.023), reached a fluid goal sooner (63 hours versus 72 hours; P = 0.035), and postoperative duration of TPN usage was significantly shorter in the postintervention period (48 hours versus 62 hours; P = 0.041) with no increase in adverse outcome events or unintended consequences.
Conclusions: By implementing a feeding protocol, we reduced practice variation among providers, increased the number of patients fed enterally preoperatively and reduced postoperative use of TPN without increased complications.
Figures


 , mean;
, mean;  , average SD 1: point more than 3 SD from center line. Figure made with Minitab18.
, average SD 1: point more than 3 SD from center line. Figure made with Minitab18.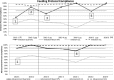
References
-
- Owens JL, Musa N. Nutrition support after neonatal cardiac surgery. Nutr Clin Pract. 2009;24:242–249.. - PubMed
-
- Newcombe J, Fry-Bowers E. A post-operative feeding protocol to improve outcomes for neonates with critical congenital heart disease. J Pediatr Nurs. 2017;35:139–143.. - PubMed
-
- Wong JJ, Cheifetz IM, Ong C, et al. Nutrition support for children undergoing congenital heart surgeries: a narrative review. World J Pediatr Congenit Heart Surg. 2015;6:443–454.. - PubMed
-
- Wang KS, Ford HR, Upperman JS. Metabolic response to stress in the neonate who has surgery. Neoreviews. 2006;7:410–418..
-
- Alten JA, Rhodes LA, Tabbutt S, et al. Perioperative feeding management of neonates with CHD: analysis of the Pediatric Cardiac Critical Care Consortium (PC4) registry. Cardiol Young. 2015;25:1593–1601.. - PubMed
LinkOut - more resources
Full Text Sources
Other Literature Sources
Research Materials
