Hepatic fat and glucose tolerance in women with recent gestational diabetes
- PMID: 30233804
- PMCID: PMC6135458
- DOI: 10.1136/bmjdrc-2018-000549
Hepatic fat and glucose tolerance in women with recent gestational diabetes
Abstract
Objective: Women with a history of gestational diabetes mellitus (GDM) have an elevated risk of ultimately developing pre-diabetes and diabetes later in life. They also have an increased prevalence of fatty liver, but recent studies have reported conflicting findings on whether hepatic fat affects their risk of pre-diabetes/diabetes. Thus, we sought to evaluate the associations of liver fat with glucose homeostasis and determinants thereof in women with and without recent gestational dysglycemia.
Methods: Two hundred and fifty-seven women underwent an antepartum oral glucose tolerance test (OGTT), which diagnosed 97 with GDM, 40 with gestational impaired glucose tolerance (GIGT), and 120 with normal glucose tolerance (NGT). At a mean of 4.8 years post partum, they underwent an OGTT (which revealed that 52 had progressed to pre-diabetes/diabetes) and hepatic ultrasound, on which liver fat was graded as none (n=164), mild (n=66), or moderate (n=27).
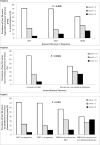
Results: Liver fat was more prevalent in women with previous GDM than in those with GIGT or NGT (p=0.009) and in women with current pre-diabetes/diabetes than in those without (p=0.0003). As the severity of liver fat increased, there was a progressive worsening of insulin sensitivity and beta-cell function, coupled with rising fasting and 2-hour glucose (all p<0.0001). On multiple linear regression analyses, moderate liver fat was independently associated with lower insulin sensitivity (p=0.0002) and higher 2-hour glucose (p=0.009). Moreover, moderate liver fat emerged as an independent predictor of pre-diabetes/diabetes (OR=3.66, 95% CI 1.1 to 12.5).
Conclusion: The higher prevalence of liver fat in women with previous GDM is associated with their increased risk of pre-diabetes/diabetes.
Keywords: fatty liver; gestational diabetes; insulin sensitivity; liver fat; pre-diabetes.
Conflict of interest statement
Competing interests: None declared.
Figures

Similar articles
-
Each degree of glucose intolerance in pregnancy predicts distinct trajectories of β-cell function, insulin sensitivity, and glycemia in the first 3 years postpartum.Diabetes Care. 2014 Dec;37(12):3262-9. doi: 10.2337/dc14-1529. Epub 2014 Sep 17. Diabetes Care. 2014. PMID: 25231898
-
The postpartum cardiovascular risk factor profile of women with isolated hyperglycemia at 1-hour on the oral glucose tolerance test in pregnancy.Nutr Metab Cardiovasc Dis. 2011 Sep;21(9):706-12. doi: 10.1016/j.numecd.2011.02.010. Epub 2011 Jun 23. Nutr Metab Cardiovasc Dis. 2011. PMID: 21703831
-
Analysis of oral glucose tolerance test in pregnant women with abnormal glucose metabolism.Chin Med J (Engl). 2005 Jun 20;118(12):995-9. Chin Med J (Engl). 2005. PMID: 15978207
-
Gestational diabetes mellitus and subsequent development of overt diabetes mellitus.Dan Med Bull. 1998 Nov;45(5):495-509. Dan Med Bull. 1998. PMID: 9850811 Review.
-
[Gestational diabetes mellitus (Update 2019)].Wien Klin Wochenschr. 2019 May;131(Suppl 1):91-102. doi: 10.1007/s00508-018-1419-8. Wien Klin Wochenschr. 2019. PMID: 30980150 Review. German.
Cited by
-
Incidence of Prediabetes/Diabetes among Women with Prior Gestational Diabetes and Non-Alcoholic Fatty Liver Disease: A Prospective Observational Study.Indian J Endocrinol Metab. 2023 Jul-Aug;27(4):319-324. doi: 10.4103/ijem.ijem_60_23. Epub 2023 Aug 28. Indian J Endocrinol Metab. 2023. PMID: 37867978 Free PMC article.
-
Insulin resistance, beta-cell function, adipokine profiles and cardiometabolic risk factors among Chinese youth with isolated impaired fasting glucose versus impaired glucose tolerance: the BCAMS study.BMJ Open Diabetes Res Care. 2020 Feb;8(1):e000724. doi: 10.1136/bmjdrc-2019-000724. BMJ Open Diabetes Res Care. 2020. PMID: 32049638 Free PMC article.
-
Synergistic effect of non-alcoholic fatty liver disease and history of gestational diabetes to increase risk of type 2 diabetes.Eur J Epidemiol. 2023 Aug;38(8):901-911. doi: 10.1007/s10654-023-01016-1. Epub 2023 May 31. Eur J Epidemiol. 2023. PMID: 37253998
-
Gestational diabetes mellitus and development of intergenerational non-alcoholic fatty liver disease (NAFLD) after delivery: a systematic review and meta-analysis.EClinicalMedicine. 2024 Apr 29;72:102609. doi: 10.1016/j.eclinm.2024.102609. eCollection 2024 Jun. EClinicalMedicine. 2024. PMID: 38707911 Free PMC article.
-
Implications of Nonalcoholic Fatty Liver Disease on Pregnancy and Maternal and Child Outcomes.Gastroenterol Hepatol (N Y). 2019 Apr;15(4):221-228. Gastroenterol Hepatol (N Y). 2019. PMID: 31435201 Free PMC article.
References
-
- Ballestri S, Zona S, Targher G, et al. . Nonalcoholic fatty liver disease is associated with an almost twofold increased risk of incident type 2 diabetes and metabolic syndrome. Evidence from a systematic review and meta-analysis. J Gastroenterol Hepatol 2016;31:936–44. 10.1111/jgh.13264 - DOI - PubMed
LinkOut - more resources
Full Text Sources
Other Literature Sources
Research Materials
