Development and validation of a modified quick SOFA scale for risk assessment in sepsis syndrome
- PMID: 30256855
- PMCID: PMC6157867
- DOI: 10.1371/journal.pone.0204608
Development and validation of a modified quick SOFA scale for risk assessment in sepsis syndrome
Abstract
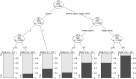
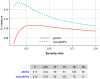
Sepsis is a severe clinical syndrome owing to its high mortality. Quick Sequential Organ Failure Assessment (qSOFA) score has been proposed for the prediction of fatal outcomes in sepsis syndrome in emergency departments. Due to the low predictive performance of the qSOFA score, we propose a modification to the score by adding age. We conducted a multicenter, retrospective cohort study among regional referral centers from various regions of the country. Participants recruited data of patients admitted to emergency departments and obtained a diagnosis of sepsis syndrome. Crude in-hospital mortality was the primary endpoint. A generalized mixed-effects model with random intercepts produced estimates for adverse outcomes. Model-based recursive partitioning demonstrated the effects and thresholds of significant covariates. Scores were internally validated. The H measure compared performances of scores. A total of 580 patients from 22 centers were included for further analysis. Stages of sepsis, age, time to antibiotics, and administration of carbapenem for empirical treatment were entered the final model. Among these, severe sepsis (OR, 4.40; CIs, 2.35-8.21), septic shock (OR, 8.78; CIs, 4.37-17.66), age (OR, 1.03; CIs, 1.02-1.05) and time to antibiotics (OR, 1.05; CIs, 1.01-1.10) were significantly associated with fatal outcomes. A decision tree demonstrated the thresholds for age. We modified the quick Sequential Organ Failure Assessment (mod-qSOFA) score by adding age (> 50 years old = one point) and compared this to the conventional score. H-measures for qSOFA and mod-qSOFA were found to be 0.11 and 0.14, respectively, whereas AUCs of both scores were 0.64. We propose the use of the modified qSOFA score for early risk assessment among sepsis patients for improved triage and management of this fatal syndrome.
Conflict of interest statement
The authors have declared that no competing interests exist.
Figures
Similar articles
-
Low sensitivity of qSOFA, SIRS criteria and sepsis definition to identify infected patients at risk of complication in the prehospital setting and at the emergency department triage.Scand J Trauma Resusc Emerg Med. 2017 Nov 3;25(1):108. doi: 10.1186/s13049-017-0449-y. Scand J Trauma Resusc Emerg Med. 2017. PMID: 29100549 Free PMC article.
-
Classification versus Prediction of Mortality Risk using the SIRS and qSOFA Scores in Patients with Infection Transported by Paramedics.Prehosp Emerg Care. 2020 Mar-Apr;24(2):282-289. doi: 10.1080/10903127.2019.1624901. Epub 2019 Jun 19. Prehosp Emerg Care. 2020. PMID: 31140890
-
Quick sequential organ failure assessment compared to systemic inflammatory response syndrome for predicting sepsis in emergency department.J Crit Care. 2017 Dec;42:12-17. doi: 10.1016/j.jcrc.2017.06.020. Epub 2017 Jun 19. J Crit Care. 2017. PMID: 28647650
-
Accuracy of quick Sequential Organ Failure Assessment (qSOFA) score and systemic inflammatory response syndrome (SIRS) criteria for predicting mortality in hospitalized patients with suspected infection: a meta-analysis of observational studies.Clin Microbiol Infect. 2018 Nov;24(11):1123-1129. doi: 10.1016/j.cmi.2018.03.032. Epub 2018 Mar 29. Clin Microbiol Infect. 2018. PMID: 29605565
-
Head-to-head comparison of qSOFA and SIRS criteria in predicting the mortality of infected patients in the emergency department: a meta-analysis.Scand J Trauma Resusc Emerg Med. 2018 Jul 11;26(1):56. doi: 10.1186/s13049-018-0527-9. Scand J Trauma Resusc Emerg Med. 2018. PMID: 29996880 Free PMC article. Review.
Cited by
-
The clinical features, treatment and prognosis of neutropenic fever and Coronavirus disease 2019 results of the multicentre teos study.Sci Rep. 2024 Mar 3;14(1):5218. doi: 10.1038/s41598-024-55886-w. Sci Rep. 2024. PMID: 38433274 Free PMC article.
-
Quick sequential organ failure assessment score combined with other sepsis-related risk factors to predict in-hospital mortality: Post-hoc analysis of prospective multicenter study data.PLoS One. 2021 Jul 15;16(7):e0254343. doi: 10.1371/journal.pone.0254343. eCollection 2021. PLoS One. 2021. PMID: 34264977 Free PMC article.
-
Comment on "Comparison of different versions of the quick sequential organ failure assessment for predicting in-hospital mortality of sepsis patients".World J Emerg Med. 2022;13(2):160. doi: 10.5847/wjem.j.1920-8642.2022.049. World J Emerg Med. 2022. PMID: 35237376 Free PMC article. No abstract available.
-
Treatment of ventilator-associated pneumonia (VAP) caused by Acinetobacter: results of prospective and multicenter ID-IRI study.Eur J Clin Microbiol Infect Dis. 2020 Jan;39(1):45-52. doi: 10.1007/s10096-019-03691-z. Epub 2019 Sep 9. Eur J Clin Microbiol Infect Dis. 2020. PMID: 31502120 Free PMC article.
-
ABC2-SPH risk score for in-hospital mortality in COVID-19 patients: development, external validation and comparison with other available scores.Int J Infect Dis. 2021 Sep;110:281-308. doi: 10.1016/j.ijid.2021.07.049. Epub 2021 Jul 24. Int J Infect Dis. 2021. PMID: 34311100 Free PMC article.
References
-
- Angus DC, Linde-Zwirble WT, Lidicker J, Clermont G, Carcillo J, Pinsky MR. Epidemiology of severe sepsis in the United States: analysis of incidence, outcome, and associated costs of care. Crit Care Med. 2001;29: 1303–1310. - PubMed
-
- American College of Chest Physicians/Society of Critical Care Medicine Consensus Conference: definitions for sepsis and organ failure and guidelines for the use of innovative therapies in sepsis. Crit Care Med. 1992;20: 864–874. - PubMed
Publication types
MeSH terms
LinkOut - more resources
Full Text Sources
Other Literature Sources

