Outcomes after carotid endarterectomy among elderly dual Medicare-Medicaid-eligible patients
- PMID: 30266891
- PMCID: PMC6205687
- DOI: 10.1212/WNL.0000000000006380
Outcomes after carotid endarterectomy among elderly dual Medicare-Medicaid-eligible patients
Abstract
Objective: To determine whether patients who are dual eligible for Medicare and Medicaid benefits have outcomes after carotid endarterectomy (CEA) that are comparable to the outcomes of those eligible for Medicare alone.
Methods: The study cohort included fee-for-service Medicare beneficiaries ≥65 years of age who underwent CEA (ICD-9-CM code 38.12) between 2003 and 2010. Beneficiaries with ≥1 month of Medicaid coverage were considered dual eligible. We fit mixed models to assess the relationship between coverage (dual eligible vs Medicare only) and outcomes over time after adjustment for demographic and clinical characteristics.
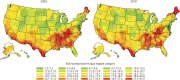
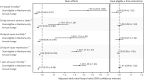
Results: There were 53,773 dual-eligible and 452,182 Medicare-only beneficiaries hospitalized for CEA. The percentage of dual-eligible patients receiving CEA increased from 10.1% in 2003 to 11.5% in 2010, with no change in geographic distribution across the country. In adjusted analyses, dual-eligible vs Medicare-only beneficiaries had a higher rate of 30-day ischemic stroke or death; higher in-hospital, 30-day, and 1-year all-cause mortality; and higher 30-day all-cause readmission. Relative annual reductions in outcomes from 2003 to 2010 ranged from 2% to 5%, but there was no significant interaction between dual-eligible status and time.
Conclusions: Dual-eligible beneficiaries had worse outcomes than those eligible for Medicare alone. Additional work is necessary to understand the reasons for this difference.
© 2018 American Academy of Neurology.
Figures
Comment in
-
Carotid endarterectomy outcomes: What does the patient bring to the table?Neurology. 2018 Oct 23;91(17):769-770. doi: 10.1212/WNL.0000000000006374. Epub 2018 Sep 28. Neurology. 2018. PMID: 30266890 No abstract available.
References
-
- Medicare-Medicaid Coordination Office. Data analysis brief: Medicare-Medicaid dual enrollment from 2006 through 2015 [online]. Available at: cms.gov/Medicare-Medicaid-Coordination/Medicare-and-Medicaid-Coordinatio.... Accessed March 3, 2017.
-
- Kasper J, Watts MO, Lyons B. Chronic disease and co-morbidity among dual eligibles: implications for patterns of Medicaid and Medicare service use and spending [online]. Available at: kaiserfamilyfoundation.files.wordpress.com/2013/01/8081.pdf. Accessed August 25, 2017.
-
- Medicare Payment Advisory Commission and Medicaid and CHIP Payment and Access Commission. Data Book: Beneficiaries Dually Eligible for Medicare and Medicaid - January 2017 [online]. Available at: macpac.gov/wp-content/uploads/2017/01/Jan17_MedPAC_MACPAC_DualsDataBook.pdf. Accessed August 25, 2017.
-
- Addo J, Ayerbe L, Mohan KM, et al. . Socioeconomic status and stroke: an updated review. Stroke 2012;43:1186–1191. - PubMed
-
- Ultee KH, Bastos Goncalves F, Hoeks SE, et al. . Low socioeconomic status is an independent risk factor for survival after abdominal aortic aneurysm repair and open surgery for peripheral artery disease. Eur J Vasc Endovasc Surg 2015;50:615–622. - PubMed
Publication types
MeSH terms
Grants and funding
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical
