Early urine electrolyte patterns in patients with acute heart failure
- PMID: 30295437
- PMCID: PMC6351901
- DOI: 10.1002/ehf2.12368
Early urine electrolyte patterns in patients with acute heart failure
Abstract
Aims: We conducted a prospective study of emergency department (ED) patients with acute heart failure (AHF) to determine if worsening HF (WHF) could be predicted based on urinary electrolytes during the first 1-2 h of ED care. Loop diuretics are standard therapy for AHF patients. A subset of patients hospitalized for AHF will develop a blunted natriuretic response to loop diuretics, termed diuretic resistance, which often leads to WHF. Early detection of diuretic resistance could facilitate escalation of therapy and prevention of WHF.
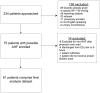
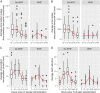
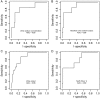
Methods and results: Patients were eligible if they had an ED AHF diagnosis, had not yet received intravenous diuretics, had a systolic blood pressure > 90 mmHg, and were not on dialysis. Urine electrolytes and urine output were collected at 1, 2, 4, and 6 h after diuretic administration. Worsening HF was defined as clinically persistent or WHF requiring escalation of diuretics or administration of intravenous vasoactives after the ED stay. Of the 61 patients who qualified in this pilot study, there were 10 (16.3%) patients who fulfilled our definition of WHF. At 1 h after diuretic administration, patients who developed WHF were more likely to have low urinary sodium (9.5 vs. 43.0 mmol; P < 0.001) and decreased urine sodium concentration (48 vs. 80 mmol/L; P = 0.004) than patients without WHF. All patients with WHF had a total urine sodium of <35.4 mmol at 1 h (100% sensitivity and 60% specificity).
Conclusions: One hour after diuretic administration, a urine sodium excretion of <35.4 mmol was highly suggestive of the development of WHF. These relationships require further testing to determine if early intervention with alternative agents can prevent WHF.
Keywords: Acute heart failure; Diuretic resistance; Emergency department; Urine electrolytes; Worsening heart failure.
© 2018 The Authors. ESC Heart Failure published by John Wiley & Sons Ltd on behalf of the European Society of Cardiology.
Figures
Similar articles
-
Prevalence and characteristics of upfront diuretic resistance in acute heart failure: The P-Value-AHF study.ESC Heart Fail. 2025 Feb;12(1):688-694. doi: 10.1002/ehf2.15069. Epub 2024 Sep 6. ESC Heart Fail. 2025. PMID: 39239801 Free PMC article. Clinical Trial.
-
Role of spot urinary sodium in outpatients with heart failure.Rev Esp Cardiol (Engl Ed). 2025 Mar;78(3):185-195. doi: 10.1016/j.rec.2024.07.002. Epub 2024 Jul 20. Rev Esp Cardiol (Engl Ed). 2025. PMID: 39038750 English, Spanish.
-
Spot urine sodium-to-creatinine ratio surpasses sodium in identifying poor diuretic response in acute heart failure.ESC Heart Fail. 2024 Oct;11(5):3438-3442. doi: 10.1002/ehf2.14883. Epub 2024 Jun 10. ESC Heart Fail. 2024. PMID: 38855817 Free PMC article.
-
Diuretic Resistance in Heart Failure.Curr Heart Fail Rep. 2019 Apr;16(2):57-66. doi: 10.1007/s11897-019-0424-1. Curr Heart Fail Rep. 2019. PMID: 30762178 Free PMC article. Review.
-
Worsening Heart Failure: Nomenclature, Epidemiology, and Future Directions: JACC Review Topic of the Week.J Am Coll Cardiol. 2023 Jan 31;81(4):413-424. doi: 10.1016/j.jacc.2022.11.023. J Am Coll Cardiol. 2023. PMID: 36697141 Review.
Cited by
-
Urine sodium concentration after intravenous furosemide in dogs with acute congestive heart failure and correlation with treatment efficacy.J Vet Intern Med. 2024 Jan-Feb;38(1):71-80. doi: 10.1111/jvim.16955. Epub 2023 Dec 1. J Vet Intern Med. 2024. PMID: 38038223 Free PMC article.
-
Loop diuretic resistance complicating acute heart failure.Heart Fail Rev. 2020 Jan;25(1):133-145. doi: 10.1007/s10741-019-09851-9. Heart Fail Rev. 2020. PMID: 31520280 Review.
-
Bioanalytical Assessment of Plasma Concentrations of Angiotensin-Converting Enzyme II Inhibitors and Angiotensin Receptor Blockers: A Pilot Study Among Patients Hospitalized With Acute Heart Failure.Am J Ther. 2020 Jul/Aug;27(4):e366-e370. doi: 10.1097/MJT.0000000000000990. Am J Ther. 2020. PMID: 31833870 Free PMC article.
-
Usefulness of natriuresis to predict in-hospital diuretic resistance.Am J Cardiovasc Dis. 2020 Oct 15;10(4):350-355. eCollection 2020. Am J Cardiovasc Dis. 2020. PMID: 33224582 Free PMC article.
-
Natriuretic Equation to Predict Loop Diuretic Response in Patients With Heart Failure.J Am Coll Cardiol. 2021 Feb 16;77(6):695-708. doi: 10.1016/j.jacc.2020.12.022. J Am Coll Cardiol. 2021. PMID: 33573739 Free PMC article.
References
-
- Adams KF Jr, Fonarow GC, Emerman CL, LeJemtel TH, Costanzo MR, Abraham WT, Berkowitz RL, Galvao M, Horton DP. Characteristics and outcomes of patients hospitalized for heart failure in the United States: rationale, design, and preliminary observations from the first 100,000 cases in the Acute Decompensated Heart Failure National Registry (ADHERE). Am Heart J 2005; 149: 209–216. - PubMed
-
- Ter Maaten JM, Valente MA, Damman K, Hillege HL, Navis G, Voors AA. Diuretic response in acute heart failure—pathophysiology, evaluation, and therapy. Nat Rev Cardiol 2015; 12: 184–192. - PubMed
-
- O'Connor CM, Starling RC, Hernandez AF, Armstrong PW, Dickstein K, Hasselblad V, Heizer GM, Komajda M, Massie BM, McMurray JJ, Nieminen MS, Reist CJ, Rouleau JL, Swedberg K, Adams KF Jr, Anker SD, Atar D, Battler A, Botero R, Bohidar NR, Butler J, Clausell N, Corbalan R, Costanzo MR, Dahlstrom U, Deckelbaum LI, Diaz R, Dunlap ME, Ezekowitz JA, Feldman D, Felker GM, Fonarow GC, Gennevois D, Gottlieb SS, Hill JA, Hollander JE, Howlett JG, Hudson MP, Kociol RD, Krum H, Laucevicius A, Levy WC, Mendez GF, Metra M, Mittal S, Oh BH, Pereira NL, Ponikowski P, Wilson WH, Tanomsup S, Teerlink JR, Triposkiadis F, Troughton RW, Voors AA, Whellan DJ, Zannad F, Califf RM. Effect of nesiritide in patients with acute decompensated heart failure. N Engl J Med 2011; 365: 32–43. - PubMed
-
- Teerlink JR, Cotter G, Davison BA, Felker GM, Filippatos G, Greenberg BH, Ponikowski P, Unemori E, Voors AA, Adams KF Jr, Dorobantu MI, Grinfeld LR, Jondeau G, Marmor A, Masip J, Pang PS, Werdan K, Teichman SL, Trapani A, Bush CA, Saini R, Schumacher C, Severin TM, Metra M. Serelaxin, recombinant human relaxin‐2, for treatment of acute heart failure (RELAX‐AHF): a randomised, placebo‐controlled trial. Lancet 2013; 381: 29–39. - PubMed
-
- Packer M, O'Connor C, McMurray JJ, Wittes J, Abraham WT, Anker SD, Dickstein K, Filippatos G, Holcomb R, Krum H, Maggioni AP, Mebazaa A, Peacock WF, Petrie MC, Ponikowski P, Ruschitzka F, van Veldhuisen DJ, Kowarski LS, Schactman M, Holzmeister J. Effect of ularitide on cardiovascular mortality in acute heart failure. N Engl J Med 2017; 376: 1956–1964. - PubMed
Publication types
MeSH terms
Substances
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical
Research Materials
Miscellaneous

