Identifying the Optimal Candidate for Salvage Lymph Node Dissection for Nodal Recurrence of Prostate Cancer: Results from a Large, Multi-institutional Analysis
- PMID: 30301694
- PMCID: PMC9084635
- DOI: 10.1016/j.eururo.2018.09.009
Identifying the Optimal Candidate for Salvage Lymph Node Dissection for Nodal Recurrence of Prostate Cancer: Results from a Large, Multi-institutional Analysis
Abstract
Background: Salvage lymph node dissection (SLND) represents a possible treatment option for prostate cancer patients affected by nodal recurrence after local treatment. However, SLND may be associated with intra- and postoperative complications, and the oncological benefit may be limited to specific groups of patients.
Objective: To identify the optimal candidates for SLND based on preoperative characteristics.
Design, setting, and participants: The study included 654 patients who experienced prostate-specific antigen (PSA) rise and nodal recurrence after radical prostatectomy (RP) and underwent SLND at nine tertiary referral centers. Lymph node recurrence was documented by positron emission tomography/computed tomography (PET/CT) scan using either 11C-choline or 68Ga-labeled prostate-specific membrane antigen ligand.
Intervention: SLND.
Outcome measurements and statistical analysis: The study outcome was early clinical recurrence (eCR) developed within 1 yr after SLND. Multivariable Cox regression analysis was used to develop a predictive model. Multivariable-derived coefficients were used to develop a novel risk calculator. Decision-curve analysis was used to evaluate the net benefit of the predictive model.
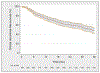
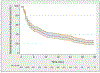
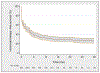
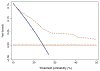
Results and limitations: Median follow-up was 30 (interquartile range, 16-50) mo among patients without clinical recurrence (CR), and 334 patients developed CR after SLND. In particular, eCR at 1 yr after SLND was observed in 150 patients, with a Kaplan-Meier probability of eCR equal to 25%. The development of eCR was significantly associated with an increased risk of cancer-specific mortality at 3 yr, being 20% versus 1.4% in patients with and without eCR, respectively (p<0.0001). At multivariable analysis, Gleason grade group 5 (hazard ratio [HR]: 2.04; p<0.0001), time from RP to PSA rising (HR: 0.99; p=0.025), hormonal therapy administration at PSA rising after RP (HR: 1.47; p=0.0005), retroperitoneal uptake at PET/CT scan (HR: 1.24; p=0.038), three or more positive spots at PET/CT scan (HR: 1.26; p=0.019), and PSA level at SLND (HR: 1.05; p<0.0001) were significant predictors of CR after SLND. The coefficients of the predictive model were used to develop a risk calculator for eCR at 1 yr after SLND. The discrimination of the model (Harrel'sC index) was 0.75. At decision-curve analysis, the net benefit of the model was higher than the "treat-all" option at all the threshold probabilities.
Conclusions: We reported the largest available series of patients treated with SLND. Roughly 25% of men developed eCR after surgery. We developed the first risk stratification tool to identify the optimal candidate to SLND based on routinely available preoperative characteristics. This tool can be useful to avoid use of SLND in men more likely to progress despite any imaging-guided approach.
Patient summary: The risk of early recurrence after salvage lymph node dissection (SLND) was approximately 25%. In this study, we developed a novel tool to predict the risk of early failure after SLND. This tool will be useful to identify patients who would benefit the most from SLND from other patients who should be spared from surgery.
Keywords: Lymph node excision; Neoplasm recurrence; Positron emission tomography computed tomography; Prostatic neoplasms; Salvage therapy.
Copyright © 2018 European Association of Urology. All rights reserved.
Conflict of interest statement
Figures

Comment in
-
Re: Identifying the Optimal Candidate for Salvage Lymph Node Dissection for Nodal Recurrence of Prostate Cancer: Results from a Large, Multi-institutional Analysis.Eur Urol. 2020 Apr;77(4):558-559. doi: 10.1016/j.eururo.2019.11.027. Epub 2019 Dec 12. Eur Urol. 2020. PMID: 31839490 No abstract available.
References
-
- Pound CR, Partin AW, Eisenberger MA, Chan DW, Pearson JD, Walsh PC. Natural history of progression after PSA elevation following radical prostatectomy. Jama 1999;281:1591–7. - PubMed
-
- Boorjian SA, Thompson RH, Tollefson MK, et al. Long-term risk of clinical progression after biochemical recurrence following radical prostatectomy: the impact of time from surgery to recurrence. Eur Urol 2011;59:893–9. - PubMed
-
- Glass TR, Tangen CM, Crawford ED, Thompson I. Metastatic carcinoma of the prostate: identifying prognostic groups using recursive partitioning. J Urol 2003;169:164–9. - PubMed
-
- Mitchell CR, Lowe VJ, Rangel LJ, Hung JC, Kwon ED, Karnes RJ. Operational characteristics of (11)c-choline positron emission tomography/computerized tomography for prostate cancer with biochemical recurrence after initial treatment. J Urol 2013;189:1308–13. - PubMed
-
- Ceci F, Herrmann K, Castellucci P, et al. Impact of 11C-choline PET/CT on clinical decision making in recurrent prostate cancer: results from a retrospective two-centre trial. Eur J Nucl Med Mol Imaging 2014;41:2222–31. - PubMed
Publication types
MeSH terms
Grants and funding
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical
Research Materials
Miscellaneous

