Association between diabetes mellitus and multi-drug-resistant tuberculosis: evidence from a systematic review and meta-analysis
- PMID: 30322409
- PMCID: PMC6190557
- DOI: 10.1186/s13643-018-0828-0
Association between diabetes mellitus and multi-drug-resistant tuberculosis: evidence from a systematic review and meta-analysis
Abstract
Background: Diabetes mellitus (DM) poses a significant risk for the development of active tuberculosis (TB) and complicates its treatment. However, there is inconclusive evidence on whether the TB-DM co-morbidity is associated with a higher risk of developing multi-drug-resistant tuberculosis (MDR-TB). The aim of this meta-analysis was to summarize available evidence on the association of DM and MDR-TB and to estimate a pooled effect measure.
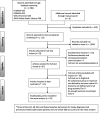
Methods: PubMed, Excerpta Medica Database (EMBASE), Web of Science, World Health Organization (WHO), and Global Health Library database were searched for all studies published in English until July 2018 and that reported the association of DM and MDR-TB among TB patients. To assess study quality, we used the Newcastle-Ottawa Scale for cohort and case-control studies and the Agency for Healthcare Research and Quality tool for cross-sectional studies. We checked the between-study heterogeneity using the Cochrane Q chi-squared statistic and I2 and examined a potential publication bias by visual inspection of the funnel plot and Egger's regression test statistic. The random-effect model was fitted to estimate the summary effects, odds ratios (ORs), and 95% confidence interval (CIs) across studies.
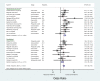
Results: This meta-analysis of 24 observational studies from 15 different countries revealed that DM has a significant association with MDR-TB (OR = 1.97, 95% CI = 1.58-2.45, I2 = 38.2%, P value for heterogeneity = 0.031). The significant positive association remained irrespective of country income level, type of DM, how TB or DM was diagnosed, and design of primary studies. A stronger association was noted in a pooled estimate of studies which adjusted for at least one confounding factor, OR = 2.43, 95% CI 1.90 to 3.12. There was no significant publication bias detected.
Conclusions: The results suggest that DM can significantly increase the odds of developing MDR-TB. Consequently, a more robust TB treatment and follow-up might be necessary for patients with DM. Efforts to control DM can have a substantial beneficial effect on TB outcomes, particularly in the case of MDR-TB.
Systematic review registration: PROSPERO CRD42016045692 .
Keywords: Diabetes mellitus; Meta-analysis; Multi-drug-resistant tuberculosis; Systematic review; Tuberculosis.
Conflict of interest statement
Ethics approval and consent to participate
Not applicable
Consent for publication
Not applicable
Competing interests
The authors declare that they have no competing interests.
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Figures

References
-
- World Health Organization . Global tuberculosis report 2017. Geneva: World Health Organization; 2017.
-
- World Health Organization . WHO end TB strategy: global strategy and targets for tuberculosis prevention, care and control after 2015. Geneva: WHO; 2015.
-
- Marais BJ, Lönnroth K, Lawn SD, Migliori GB, Mwaba P, Glaziou P, et al. Tuberculosis comorbidity with communicable and non-communicable diseases: integrating health services and control eff orts. Lancet Infect Dis 2013. 2013;13:13. - PubMed
-
- IDF . IDF Diabetes ATLAS. 2013.
Publication types
MeSH terms
LinkOut - more resources
Full Text Sources
Medical

