Cost and Hospital Resource Utilization of Staphylococcus aureus Infection Post Elective Posterior Instrumented Spinal Fusion Surgeries in U.S. Hospitals: A Retrospective Cohort Study
- PMID: 30325882
- PMCID: PMC6485304
- DOI: 10.1097/BRS.0000000000002898
Cost and Hospital Resource Utilization of Staphylococcus aureus Infection Post Elective Posterior Instrumented Spinal Fusion Surgeries in U.S. Hospitals: A Retrospective Cohort Study
Abstract
Study design: A retrospective cohort study.
Objective: The aim of this study was to assess hospital resource utilization and costs associated with Staphylococcus aureus infection within 180 days post elective posterior instrumented spinal fusion surgeries (index surgery) between 2010 and 2015.
Summary of background data: Surgical site infections (SSIs) and blood stream infections (BSIs) post spinal fusion surgeries are associated with worse clinical outcomes and increased costs. Economic data specific to the most common pathogen of infections post spinal fusion surgeries, S. aureus, are limited.
Methods: We analyzed hospital discharge and microbiology data from 129 U.S. hospitals in Premier Healthcare Database. Selection criteria included age ≥ 18 years; had a primary/secondary ICD-9-CM procedure code for index surgery; and had microbiology data during study period. Outcomes included total hospitalization cost, length of stay, and risk of all-cause readmission. Infection status was classified as culture-confirmed invasive (i.e., BSIs, deep or organ/space SSIs), any, and no S. aureus infection. Multivariable regression analyses were used to compare outcome variables between infection groups controlling for known confounders.
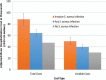
Results: Two hundred ninety-four patients had any S. aureus infection (151 had invasive infection) and 12,918 had no infection. Compared with no infection group, invasive and any infection groups had higher total hospitalization cost (adjusted mean in 2015 U.S. dollars: $88,353 and $64,356 vs. $47,366, P < 0.001), longer length of stay (adjusted mean: 20.98 and 13.15 vs. 6.77 days, P < 0.001), and higher risk of all-cause readmission [adjusted risk ratio: 2.15 (95% confidence interval: 2.06-2.25) for invasive and 1.70 (95% confidence interval: 1.61-1.80) for any infection groups].
Conclusion: S. aureus infections post elective posterior instrumented spinal fusion surgeries are associated with significantly higher hospitalization cost, length of stay, and 180-day risk of readmission than those with no such infection, which presents substantial burden to hospitals and patients. Reducing such infections may cut costs and hospital resource utilization.
Level of evidence: 3.
Figures
References
-
- Chaichana KL, Bydon M, Santiago-Dieppa DR, et al. Risk of infection following posterior instrumented lumbar fusion for degenerative spine disease in 817 consecutive cases. J Neurosurg Spine 2014; 20:45–52. - PubMed
-
- Choy W, Lam SK, Smith ZA, Dahdaleh NS. Predictors of 30-Day Hospital Readmission After Posterior Cervical Fusion in 3401 Patients. Spine 2018; 43:356–363. - PubMed
-
- Cowan JA, Jr, Dimick JB, Wainess R, et al. Changes in the utilization of spinal fusion in the United States. Neurosurgery 2006; 59:15–20. discussion 15–20. - PubMed
-
- Deyo RA, Gray DT, Kreuter W, et al. United States trends in lumbar fusion surgery for degenerative conditions. Spine (Phila Pa 1976) 2005; 30:1441–1445. discussion 1446–1447. - PubMed
MeSH terms
LinkOut - more resources
Full Text Sources
Medical
Research Materials

