Co-delivery of deferoxamine and hydroxysafflor yellow A to accelerate diabetic wound healing via enhanced angiogenesis
- PMID: 30338719
- PMCID: PMC6201774
- DOI: 10.1080/10717544.2018.1513608
Co-delivery of deferoxamine and hydroxysafflor yellow A to accelerate diabetic wound healing via enhanced angiogenesis
Abstract
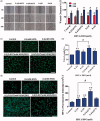
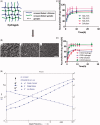
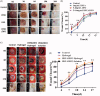
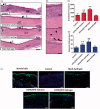
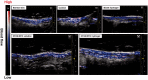
Nonhealing chronic wounds on foot induced by diabetes is a complicated pathologic process. They are mainly caused by impaired neovascularization, neuropathy, and excessive inflammation. A strategy, which can accelerate the vessel network formation as well as inhibit inflammatory response at the same time, makes it possible for effective diabetic ulcers treatment. Co-delivery of multiple drugs with complementary bioactivity offers a strategy to properly treat diabetic wound. We previously demonstrated that hydroxysafflor yellow A (HSYA) could accelerate diabetic wound healing through promoting angiogenesis and reducing inflammatory response. In order to further enhance blood vessel formation, a pro-angiogenic molecular called deferoxamine (DFO) was topically co-administrated with HSYA. The in vitro results showed that the combination of DFO and HSYA exerted synergistic effect on enhancing angiogenesis by upregulation of hypoxia inducible factor-1 alpha (HIF-1α) expression. The interpenetrating polymer networks hydrogels, characterized by good breathability and water absorption, were designed for co-loading of DFO and HSYA aiming to recruit angiogenesis relative cells and upgrade wound healing in vivo. Both DFO and HSYA in hydrogel have achieved sustained release. The in vivo studies indicated that HSYA/DFO hydrogel could accelerate diabetic wound healing. With a high expression of Hif-1α which is similar to that of normal tissue. The noninvasive US/PA imaging revealed that the wound could be recovered completely with abundant blood perfusion in dermis after given HSYA/DFO hydrogel for 28 days. In conclusion, combination of pro-angiogenic small molecule DFO and HSYA in hydrogel provides a promising strategy to productively promote diabetic wound healing as well as better the repair quality.
Keywords: Hydroxysafflor yellow A; angiogenesis; deferoxamine; diabetic wound healing; hydrogel.
Figures

Similar articles
-
Topical application of Hydroxysafflor Yellow A accelerates the wound healing in streptozotocin induced T1DM rats.Eur J Pharmacol. 2018 Mar 15;823:72-78. doi: 10.1016/j.ejphar.2018.01.018. Epub 2018 Feb 4. Eur J Pharmacol. 2018. PMID: 29408092
-
Transdermal deferoxamine prevents pressure-induced diabetic ulcers.Proc Natl Acad Sci U S A. 2015 Jan 6;112(1):94-9. doi: 10.1073/pnas.1413445112. Epub 2014 Dec 22. Proc Natl Acad Sci U S A. 2015. PMID: 25535360 Free PMC article.
-
Deferoxamine enhances neovascularization and accelerates wound healing in diabetic rats via the accumulation of hypoxia-inducible factor-1α.Diabetes Res Clin Pract. 2013 Jul;101(1):62-71. doi: 10.1016/j.diabres.2013.04.012. Epub 2013 May 28. Diabetes Res Clin Pract. 2013. PMID: 23726275
-
Deferoxamine: An Angiogenic and Antioxidant Molecule for Tissue Regeneration.Tissue Eng Part B Rev. 2019 Dec;25(6):461-470. doi: 10.1089/ten.TEB.2019.0111. Epub 2019 Sep 11. Tissue Eng Part B Rev. 2019. PMID: 31184273 Review.
-
Nanoscale Systems for Local Activation of Hypoxia-Inducible Factor-1 Alpha: A New Approach in Diabetic Wound Management.Int J Nanomedicine. 2024 Dec 21;19:13735-13762. doi: 10.2147/IJN.S497041. eCollection 2024. Int J Nanomedicine. 2024. PMID: 39723173 Free PMC article. Review.
Cited by
-
Safflower Improves Memory, Learning, and Behavior in Rats Subjected to Sleep Deprivation.Cureus. 2024 Sep 25;16(9):e70150. doi: 10.7759/cureus.70150. eCollection 2024 Sep. Cureus. 2024. PMID: 39323543 Free PMC article.
-
Hydroxysafflor Yellow A Inhibits TNF-α-Induced Inflammation of Human Fetal Lung Fibroblasts via NF-κB Signaling Pathway.Evid Based Complement Alternat Med. 2019 Dec 24;2019:4050327. doi: 10.1155/2019/4050327. eCollection 2019. Evid Based Complement Alternat Med. 2019. PMID: 31949467 Free PMC article.
-
Exploration of the common pathogenic link between COVID-19 and diabetic foot ulcers: An in silico approach.Health Sci Rep. 2023 Nov 5;6(11):e1686. doi: 10.1002/hsr2.1686. eCollection 2023 Nov. Health Sci Rep. 2023. PMID: 37936615 Free PMC article.
-
Relationship between ferroptosis and healing of diabetic foot ulcer: a prospective clinical study.Front Endocrinol (Lausanne). 2025 Jan 14;15:1412373. doi: 10.3389/fendo.2024.1412373. eCollection 2024. Front Endocrinol (Lausanne). 2025. PMID: 39877845 Free PMC article.
-
Herbal Products and Their Active Constituents for Diabetic Wound Healing-Preclinical and Clinical Studies: A Systematic Review.Pharmaceutics. 2023 Jan 14;15(1):281. doi: 10.3390/pharmaceutics15010281. Pharmaceutics. 2023. PMID: 36678910 Free PMC article. Review.
References
-
- Amin MA, Abdel-Raheem IT (2014). Accelerated wound healing and anti-inflammatory effects of physically cross linked polyvinyl alcohol-chitosan hydrogel containing honey bee venom in diabetic rats[J]. Arch Pharm Res 37:1016–31. - PubMed
-
- Andrews NC. (1999). Disorders of iron metabolism. N Engl J Med 341:1986–95. - PubMed
-
- Bergeron RJ, Wiegand J, Mcmanis JS, et al. (2003). Methoxylation of desazadesferrithiocin analogues: enhanced iron clearing efficiency. J Med Chem 46:1470–7. - PubMed
-
- Bhattarai N, Gunn J, Zhang MQ (2010). Chitosan-based hydrogels for controlled, localized drug delivery. Adv Drug Deliv Rev 62:83–99. - PubMed
MeSH terms
Substances
LinkOut - more resources
Full Text Sources
Other Literature Sources
