Refractory functional constipation: clinical management or appendicostomy?
- PMID: 30352206
- PMCID: PMC9432165
- DOI: 10.1016/j.jped.2018.09.001
Refractory functional constipation: clinical management or appendicostomy?
Abstract
Objective: To compare the clinical evolution in patients with refractory functional constipation undergoing different therapeutic regimens: oral laxatives and antegrade enemas via appendicostomy or clinical treatment with oral laxatives and rectal enemas.
Methods: Analysis of a series of 28 patients with a mean age of 7.9 years (2.4-11), followed-up in a tertiary outpatient clinic. Refractory functional constipation was defined as continuous retentive fecal incontinence after at least a 12-month period of consensus therapy. After the diagnosis of refractory condition, appendicostomy was proposed and performed in 17 patients.
Outcomes: (1) persistence of retentive fecal incontinence despite the use of enemas, (2) control of retentive fecal incontinence with enemas, and (3) control of retentive fecal incontinence, spontaneous evacuations, with no need for enemas.
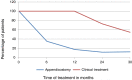
Results: Six and 12 months after the therapeutic option, control of retentive fecal incontinence was observed only in patients who underwent surgery, 11/17 and 14/17, p=0.001 and p=0.001, respectively. At 24 months, control of retentive fecal incontinence was also more frequent in operated patients: 13/17 versus 3/11 with clinical treatment, p=0.005. In the final evaluation, the median follow-up times were 2.6 and 3 years (operated vs. clinical treatment, p=0.40); one patient in each group was lost to follow-up and 9/16 operated patients had spontaneous bowel movements vs. 3/10 in the clinical treatment group, p=0.043. Surgical complications, totaling 42 episodes, were observed 14/17 patients.
Conclusion: Appendicostomy, although associated with a high frequency of complications, controlled retentive fecal incontinence earlier and more frequently than clinical treatment. The choice of one of the methods should be made by the family, after adequate information about the risks and benefits of each alternative.
Objetivo: Comparar a evolução clínica em crianças com constipação intestinal funcional refratária sob diferentes regimes terapêuticos: laxativos orais e enemas anterógrados via apendicostomia ou tratamento clínico com laxativos orais e enemas via retal.
Métodos: Análise de uma série de 28 pacientes, 7,9 anos (2,4-11), acompanhados em ambulatório terciário. Constipação intestinal funcional refratária foi definida como manutenção da incontinência fecal retentiva, em terapia consensual, por pelo menos 12 meses. Após diagnóstico de refratariedade, era proposta apendicostomia. Dezessete pacientes realizaram o procedimento cirúrgico. Desfechos: 1. Manutenção de incontinência fecal retentiva em uso de enemas; 2. Controle da incontinência fecal retentiva em uso de enemas; e 3. Controle da incontinência fecal retentiva, evacuações espontâneas, sem necessidade de enemas.
Resultados: Seis e 12 meses após opção terapêutica, controle da incontinência fecal retentiva foi observado apenas nos pacientes operados, 11/17 e 14/17, p = 0,001 e p = 0,001. Aos 24 meses, controle da incontinência fecal retentiva também mais frequente nos operados 13/17 versus 3/11 tratamento clínico, p = 0,005. Na avaliação final, medianas de tempo de seguimento: 2,6 e 3 anos (operados versus tratamento clínico, p = 0,40), um paciente em cada grupo abandonou o seguimento e 9/16 operados apresentavam evacuações espontâneas versus 3/10 no tratamento clínico, p = 0,043. Complicações cirúrgicas, 42 episódios, acometeram 14/17 pacientes.
Conclusão: A apendicostomia, embora associada a elevada frequência de complicações, controlou a incontinência fecal retentiva de maneira mais precoce e frequente que o tratamento clínico. A escolha de um dos métodos deverá caber à família, após adequada informação sobre riscos e benefícios de cada alternativa.
Keywords: Adolescent; Adolescente; Child; Constipação intestinal; Criança; Enema; Fecal incontinence; Functional constipation; Incontinência fecal.
Copyright © 2018 Sociedade Brasileira de Pediatria. Published by Elsevier Editora Ltda. All rights reserved.
Figures
Similar articles
-
The success rate of antegrade enemas for the management of idiopathic constipation.Pediatr Surg Int. 2022 Dec;38(12):1729-1736. doi: 10.1007/s00383-022-05214-y. Epub 2022 Sep 15. Pediatr Surg Int. 2022. PMID: 36107238
-
A comparison of Malone appendicostomy and cecostomy for antegrade access as adjuncts to a bowel management program for patients with functional constipation or fecal incontinence.J Pediatr Surg. 2019 Jan;54(1):123-128. doi: 10.1016/j.jpedsurg.2018.10.008. Epub 2018 Oct 5. J Pediatr Surg. 2019. PMID: 30361073
-
A randomized controlled trial of enemas in combination with oral laxative therapy for children with chronic constipation.Clin Gastroenterol Hepatol. 2009 Oct;7(10):1069-74. doi: 10.1016/j.cgh.2009.06.018. Epub 2009 Jul 1. Clin Gastroenterol Hepatol. 2009. PMID: 19576297 Clinical Trial.
-
Tube cecostomy versus appendicostomy for antegrade enemas in the management of fecal incontinence in children: A systematic review.J Pediatr Surg. 2020 Jul;55(7):1196-1200. doi: 10.1016/j.jpedsurg.2020.01.011. Epub 2020 Jan 25. J Pediatr Surg. 2020. PMID: 32037219
-
The presence of a neurodiverse disorder is associated with increased use of antegrade enema therapy in children with severe constipation: A study from the Pediatric Colorectal and Pelvic Learning Consortium (PCPLC).J Pediatr Surg. 2022 Aug;57(8):1676-1680. doi: 10.1016/j.jpedsurg.2022.04.008. Epub 2022 Apr 25. J Pediatr Surg. 2022. PMID: 35597676 Review.
Cited by
-
Towards a definition of refractory/therapy-resistant/intractable constipation in children: a cross-sectional, questionnaire-based, online survey.BMJ Paediatr Open. 2024 Dec 12;8(1):e003063. doi: 10.1136/bmjpo-2024-003063. BMJ Paediatr Open. 2024. PMID: 39667952 Free PMC article.
-
Management of children with functional constipation referred to tertiary care.J Pediatr (Rio J). 2022 May-Jun;98(3):289-295. doi: 10.1016/j.jped.2021.06.006. Epub 2021 Sep 8. J Pediatr (Rio J). 2022. PMID: 34506747 Free PMC article.
-
Radiologically supervised bowel management program outcome in patients with chronic idiopathic constipation.Pediatr Surg Int. 2023 Jul 10;39(1):229. doi: 10.1007/s00383-023-05508-9. Pediatr Surg Int. 2023. PMID: 37428259
-
How do we define therapy-resistant constipation in children aged 4-18 years old? A systematic review with meta-narrative synthesis.BMJ Paediatr Open. 2024 Jun 6;8(1):e002380. doi: 10.1136/bmjpo-2023-002380. BMJ Paediatr Open. 2024. PMID: 38844387 Free PMC article.
References
-
- Cook I.J., Talley N.J., Benninga M.A., Rao S.S., Scott S.M. Chronic constipation: overview and challenges. Neurogastroenterol Motil. 2009;21:S1–S8. - PubMed
-
- de Morais M.B., Maffei H.V. Constipação intestinal. J Pediatr (Rio J) 2000;76:147–156. - PubMed
-
- Pijpers M., Bongers M., Benninga M., Berger M. Functional constipation in children: a systematic review on prognosis and predictive factors. J Pediatr Gastroenterol Nutr. 2010;50:256–268. - PubMed
-
- Tabbers M.M., DiLorenzo C., Berger M.Y., Faure C., Langendam M.W., Nurko S., et al. Evaluation and treatment of functional constipation in infants and children: evidence-based recommendations from ESPGHAN and NASPGHAN. J Pediatr Gastroenterol Nutr. 2014;58:258–274. - PubMed
-
- Bongers M.E.J., van Wijk M.P., Reitsma J.B., Benninga M.A. Long-term prognosis for childhood constipation: clinical outcomes in adulthood. Pediatrics. 2010;126:e156. - PubMed
MeSH terms
Substances
LinkOut - more resources
Full Text Sources
Medical