Immune regulation in the aging retina
- PMID: 30352305
- PMCID: PMC6373845
- DOI: 10.1016/j.preteyeres.2018.10.003
Immune regulation in the aging retina
Abstract
The retina is an immune privileged tissue, which is protected from external and internal insults by its blood-retina barriers and immune suppressive microenvironment. Apart from the avoidance and tolerance strategies, the retina is also protected by its own defense system, i.e., microglia and the complement system. The immune privilege and defense mechanisms work together to maintain retinal homeostasis. During aging, the retina is at an increased risk of developing various degenerative diseases such as age-related macular degeneration, diabetic retinopathy, and glaucomatous retinopathy. Previously, we have shown that aging induces a para-inflammatory response in the retina. In this review, we explore the impact of aging on retinal immune regulation and the connection between homeostatic control of retinal immune privilege and para-inflammation under aging conditions and present a view that may explain why aging puts the retina at risk of developing degenerative diseases.
Keywords: Aging; Blood-retina barrier; Complement; Inflammation; Microglia; Retinal degeneration.
Copyright © 2018. Published by Elsevier Ltd.
Figures


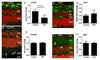

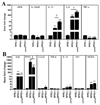



References
-
- Ahn BY, Song ES, Cho YJ, Kwon OW, Kim JK, Lee NG. Identification of an anti-aldolase autoantibody as a diagnostic marker for diabetic retinopathy by immunoproteomic analysis. Proteomics. 2006;6:1200–1209. - PubMed
-
- Anand-Apte B, H JG. Developmental Anatomy of the Retinal and Choroidal Vasculature. Encyclopedia of the Eye. 2010:9–15.
-
- Banerjee D, Dick AD. Blocking CD200-CD200 receptor axis augments NOS-2 expression and aggravates experimental autoimmune uveoretinitis in Lewis rats. Ocul Immunol Inflamm. 2004;12:115–125. - PubMed
Publication types
MeSH terms
Grants and funding
LinkOut - more resources
Full Text Sources
Medical

