The current role of laparoscopic resection for HCC: a systematic review of past ten years
- PMID: 30363804
- PMCID: PMC6182043
- DOI: 10.21037/tgh.2018.08.05
The current role of laparoscopic resection for HCC: a systematic review of past ten years
Abstract
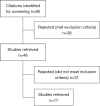
The use of laparoscopic liver resection (LLR) has progressively spread in the last 10 years. Several studies have shown the superiority of LLR to open liver resection (OLR) in term of perioperative outcomes. With this review, we aim to systematically assess short-term and long-term major outcomes in patients who underwent LLR for hepatocellular carcinoma (HCC) in order to illustrate the advantages of minimally invasive liver surgery. Through an advanced PubMed research, we selected all retrospective, prospective, and comparative clinical trials reporting short-term and long-term outcomes of any series of patients with diagnosis of HCC who underwent laparoscopic or robotic resection. Reviews, meta-analyses, or case reports were excluded. None of the patients included in this review has received a previous locoregional treatment for the same tumor nor has undergone a laparoscopic-assisted procedure. We considered morbidity and mortality for evaluation of major short-term outcomes, and overall survival (OS) and disease-free survival (DFS) for evaluation of long-term outcomes. A total of 1,501 patients from 17 retrospective studies were included, 15 studies compare LLR with OLR. Propensity-score matching (PSM) analysis was used in 11 studies (975 patients). The majority of the studies included patients with good liver function and a single HCC. Cirrhosis at pathology ranged from 33% to 100%. Overall mortality and morbidity ranges were 0-2.4% and 4.9-44% respectively, with most of the complications being Clavien-Dindo grade I or II (range: 3.9-23.3% vs. 0-9.52% for Clavien I-II and ≥ III respectively). The median blood loss ranged from 150 to 389 mL; the range of the median duration of surgery was 134-343 minutes. The maximum rate of conversion was 18.2%. The median duration of hospitalization ranged from 4 to 13 days. The ranges of overall survival rates at 1-, 3- and 5-year were 72.8-100%, 60.7-93.5% and 38-89.7% respectively. The ranges of disease free survival rates at 1-, 3- and 5-year were 45.5-91.5%, 20-72.2% and 19-67.8% respectively. The benefits of LLR in term of complication rate, blood loss, and duration of hospital stay make this procedure an advantageous alternative to OLR, especially for cirrhotic patients in whom the use of LLR reduces the risk of post-hepatectomy liver failure. The limits of LLR can be overcome by robotic surgery, which could therefore be preferred. Further benefits of minimally invasive surgery derive from its ability to reduce the formation of adhesions in view of a salvage liver transplant. In conclusion, the results of this review seem to confirm the safety and feasibility of LLR for HCC as well as its superiority to OLR according to perioperative outcomes.
Keywords: Hepatocellular carcinoma (HCC); laparoscopic liver resection (LLR); review.
Conflict of interest statement
Conflicts of Interest: The authors have no conflicts of interest to declare.
Figures
Similar articles
-
Minor laparoscopic liver resection for Hepatocellular Carcinoma is safer than minor open resection, especially for less compensated cirrhotic patients: Propensity score analysis.Surg Oncol. 2018 Dec;27(4):722-729. doi: 10.1016/j.suronc.2018.10.001. Epub 2018 Oct 3. Surg Oncol. 2018. PMID: 30449499
-
Long-term perioperative outcomes of pure laparoscopic liver resection versus open liver resection for hepatocellular carcinoma: a retrospective study.Surg Endosc. 2020 Feb;34(2):796-805. doi: 10.1007/s00464-019-06831-w. Epub 2019 Jun 3. Surg Endosc. 2020. PMID: 31161292
-
Long-term surgical outcomes in patients with hepatocellular carcinoma undergoing laparoscopic vs. open liver resection: A retrospective and propensity score-matched study.Asian J Surg. 2021 Jan;44(1):206-212. doi: 10.1016/j.asjsur.2020.05.028. Epub 2020 Jun 9. Asian J Surg. 2021. PMID: 32532684
-
Laparoscopic versus open liver resection for hepatocellular carcinoma in elderly patients: A systematic review and meta-analysis of propensity score-matched studies.Front Oncol. 2022 Nov 14;12:939877. doi: 10.3389/fonc.2022.939877. eCollection 2022. Front Oncol. 2022. PMID: 36452485 Free PMC article.
-
Short and long-term outcomes of laparoscopic compared to open liver resection for colorectal liver metastases.Hepatobiliary Surg Nutr. 2016 Aug;5(4):300-10. doi: 10.21037/hbsn.2016.02.01. Hepatobiliary Surg Nutr. 2016. PMID: 27500142 Free PMC article. Review.
Cited by
-
Explainable attention-enhanced heuristic paradigm for multi-view prognostic risk score development in hepatocellular carcinoma.Hepatol Int. 2025 Aug;19(4):866-876. doi: 10.1007/s12072-025-10793-8. Epub 2025 Mar 16. Hepatol Int. 2025. PMID: 40089963 Free PMC article.
-
New frontiers in liver resection for hepatocellular carcinoma.JHEP Rep. 2020 Jun 4;2(4):100134. doi: 10.1016/j.jhepr.2020.100134. eCollection 2020 Aug. JHEP Rep. 2020. PMID: 32695968 Free PMC article. Review.
-
Laparoscopic hepatectomy for hepatic angiomyolipoma with preoperative diagnosis of other malignancy: a report of 2 cases.Surg Case Rep. 2021 Feb 8;7(1):44. doi: 10.1186/s40792-021-01125-7. Surg Case Rep. 2021. PMID: 33555457 Free PMC article.
-
Learning curve analysis of 100 consecutive robotic liver resections.Surg Endosc. 2025 Apr;39(4):2512-2522. doi: 10.1007/s00464-025-11551-5. Epub 2025 Feb 27. Surg Endosc. 2025. PMID: 40014140 Free PMC article.
-
New trends and perspectives in hepatobiliary surgery: preface.Transl Gastroenterol Hepatol. 2018 Nov 30;3:99. doi: 10.21037/tgh.2018.11.06. eCollection 2018. Transl Gastroenterol Hepatol. 2018. PMID: 30603735 Free PMC article. No abstract available.
References
Publication types
LinkOut - more resources
Full Text Sources
Miscellaneous