Cost-Effectiveness of Alternative Anticoagulation Strategies for Postoperative Management of Total Knee Arthroplasty Patients
- PMID: 30369093
- PMCID: PMC6487236
- DOI: 10.1002/acr.23803
Cost-Effectiveness of Alternative Anticoagulation Strategies for Postoperative Management of Total Knee Arthroplasty Patients
Abstract
Objective: To evaluate the cost-effectiveness of prolonged (35-day) and standard-duration (14-day) anticoagulation therapy following total knee arthroplasty (TKA).
Methods: Using Markov modeling, we assessed clinical and economic outcomes of 14-day and 35-day anticoagulation therapy following TKA with rivaroxaban, low molecular weight heparin (LMWH), fondaparinux, warfarin, and aspirin. Incidence of complications of TKA and anticoagulation therapy (deep vein thrombosis [DVT], pulmonary embolism [PE], prosthetic joint infection [PJI], and bleeding) were derived from published literature. Daily costs ranged from $1 (aspirin) to $43 (fondaparinux). Primary outcomes included quality-adjusted life years (QALYs), direct medical costs, and incremental cost-effectiveness ratios (ICERs) at 1 year post-TKA. The preferred regimen was the regimen with highest QALYs maintaining an ICER below the willingness-to-pay threshold ($100,000/QALY). We conducted probabilistic sensitivity analyses, varying complication incidence and anticoagulation efficacy, to evaluate the impact of parameter uncertainty on model results.
Results: Aspirin resulted in the highest cumulative incidence of DVT and PE, while prolonged fondaparinux led to the largest reduction in DVT incidence (15% reduction compared to no prophylaxis). Despite differential bleeding rates (ranging from 3% to 6%), all strategies had similar incidence of PJI (1% to 2%). Prolonged rivaroxaban was the least costly strategy ($3,300 at 1 year post-TKA) and the preferred regimen in the base case. In sensitivity analyses, prolonged rivaroxaban and warfarin had similar likelihoods of being cost-effective.
Conclusion: Extending postoperative anticoagulation therapy to 35 days increases QALYs compared to standard 14-day prophylaxis. Prolonged rivaroxaban and prolonged warfarin are most likely to be cost-effective post-TKA; the costs of fondaparinux and LMWH precluded their being preferred strategies.
© 2018, American College of Rheumatology.
Conflict of interest statement
Figures
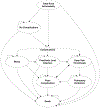

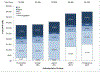
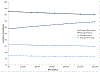
Comment in
-
Did antiphospholipid antibodies limit intervention efficacy for postoperative total knee arthroplasty-related thrombotic event prevention? Comment on the article by Smith et al.Arthritis Care Res (Hoboken). 2020 May;72(5):738. doi: 10.1002/acr.24162. Arthritis Care Res (Hoboken). 2020. PMID: 32004422 No abstract available.
-
Reply.Arthritis Care Res (Hoboken). 2020 May;72(5):738-739. doi: 10.1002/acr.24161. Arthritis Care Res (Hoboken). 2020. PMID: 32058676 No abstract available.
Similar articles
-
Trends in Deep Vein Thrombosis Prophylaxis After Total Knee Arthroplasty: 2016 to 2021.J Arthroplasty. 2024 Aug;39(8S1):S328-S332. doi: 10.1016/j.arth.2024.01.050. Epub 2024 Feb 5. J Arthroplasty. 2024. PMID: 38325530
-
Rivaroxaban for the prevention of venous thromboembolism: a single technology appraisal.Health Technol Assess. 2009 Oct;13 Suppl 3:43-8. doi: 10.3310/hta13suppl3/07. Health Technol Assess. 2009. PMID: 19846028 Review.
-
A cost-effectiveness model comparing rivaroxaban and dabigatran etexilate with enoxaparin sodium as thromboprophylaxis after total hip and total knee replacement in the irish healthcare setting.Pharmacoeconomics. 2009;27(10):829-46. doi: 10.2165/11313800-000000000-00000. Pharmacoeconomics. 2009. PMID: 19803538
-
Cost-effectiveness of low-molecular-weight heparin compared with aspirin for prophylaxis against venous thromboembolism after total joint arthroplasty.J Bone Joint Surg Am. 2013 Jul 17;95(14):1256-64. doi: 10.2106/JBJS.L.00400. J Bone Joint Surg Am. 2013. PMID: 23864173
-
Economic Evaluation of Rivaroxaban Versus Enoxaparin for Prevention of Venous Thromboembolism After Total Knee Replacement and Total Hip Replacement: A Systematic Review.Clin Drug Investig. 2020 Aug;40(8):715-725. doi: 10.1007/s40261-020-00940-4. Clin Drug Investig. 2020. PMID: 32578155
Cited by
-
Role of Direct Oral Anticoagulants for Post-operative Venous Thromboembolism Prophylaxis.Eur Cardiol. 2022 May 13;17:e11. doi: 10.15420/ecr.2021.55. eCollection 2022 Feb. Eur Cardiol. 2022. PMID: 35620356 Free PMC article. Review.
References
-
- Anderson FA, Jr., Spencer FA. Risk factors for venous thromboembolism. Circulation. 2003;107(23 Suppl 1):I9–16. - PubMed
-
- Brookenthal KR, Freedman KB, Lotke PA, Fitzgerald RH, Lonner JH. A meta-analysis of thromboembolic prophylaxis in total knee arthroplasty. The Journal of arthroplasty. 2001;16(3):293–300. - PubMed
-
- Stulberg BN, Insall JN, Williams GW, Ghelman B. Deep-vein thrombosis following total knee replacement. An analysis of six hundred and thirty-eight arthroplasties. The Journal of bone and joint surgery American volume. 1984;66(2):194–201. - PubMed
-
- Goldhaber SZ, Visani L, De Rosa M. Acute pulmonary embolism: clinical outcomes in the International Cooperative Pulmonary Embolism Registry (ICOPER). Lancet. 1999;353(9162):1386–9. - PubMed
-
- Beckman MG, Hooper WC, Critchley SE, Ortel TL. Venous thromboembolism: a public health concern. American journal of preventive medicine. 2010;38(4 Suppl):S495–501. - PubMed
Publication types
MeSH terms
Substances
Grants and funding
LinkOut - more resources
Full Text Sources
Medical

