Blood Lactate or Lactate Clearance: Which Is Robust to Predict the Neurological Outcomes after Cardiac Arrest? A Systematic Review and Meta-Analysis
- PMID: 30370306
- PMCID: PMC6189651
- DOI: 10.1155/2018/8014213
Blood Lactate or Lactate Clearance: Which Is Robust to Predict the Neurological Outcomes after Cardiac Arrest? A Systematic Review and Meta-Analysis
Abstract
Aims: Lactate and lactate clearance were supposed to be associated with cardiac arrest outcomes, but studies obtained different results. Thus, we conducted this meta-analysis to investigate the association between lactate or lactate clearance and neurological outcomes and their usefulness for prediction of neurological outcomes.
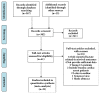
Methods: We conducted a systematic search in PubMed, Web of science, EMBASE, Medline, and Google Scholar until May 1, 2018, for relevant studies. Studies reporting lactate, lactate clearance on admission, or other time points after admission associated with neurological outcomes were included in our analysis. Pooled effect date was shown as weighed mean difference (WMD) and 95% confidence interval (CI). To measure the usefulness of lactate on admission to predict neurological outcomes, we also pooled the data of diagnostic test.
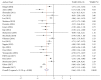
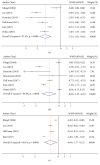
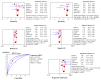
Results: 23 studies involving 6720 cardiac arrest (CA) patients were included. Results from our analysis indicated that patients with good neurological outcomes tended to have a lower lactate level on admission (WMD: -2.66 mmol/L, 95%CI: -3.39 to -1.93) and 12h, 24h, and 48h after admission (P<0.001). Furthermore, the pooled AUC for lactate level on admission to predict neurological outcomes was 0.77 (95%CI: 0.73-0.80). However, a significant association between lactate clearance and neurological outcomes was only found in 24h but not 12h lactate clearance rate.
Conclusions: Lactate levels on admission and all time points up to 48h were associated with neurological outcomes after CA, whereas the association between lactate clearance and neurological outcomes was not so stable. Lactate was a more robust surrogate marker than lactate clearance to predict neurological outcomes after CA.
Figures
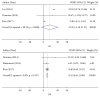
References
-
- S. Ecc Committee and A. Task Forces of the American Heart, “2005 American Heart Association Guidelines for Cardiopulmonary Resuscitation and Emergency Cardiovascular Care”, Circulation, vol. 112, no.24 Suppl, pp. IV1-203, 2005. - PubMed
-
- Nolan J. P., Soar J., Cariou A., et al. European Resuscitation Council and European Society of Intensive Care Medicine Guidelines for Post-resuscitation Care 2015. Section 5 of the European Resuscitation Council Guidelines for Resuscitation 2015. Resuscitation. 2015;95:202–222. doi: 10.1016/j.resuscitation.2015.07.018. - DOI - PubMed
Publication types
MeSH terms
Substances
LinkOut - more resources
Full Text Sources
Medical

