Survival in pulmonary hypertension due to chronic lung disease: Influence of low diffusion capacity of the lungs for carbon monoxide
- PMID: 30391191
- PMCID: PMC6556403
- DOI: 10.1016/j.healun.2018.09.011
Survival in pulmonary hypertension due to chronic lung disease: Influence of low diffusion capacity of the lungs for carbon monoxide
Abstract
Background: Patients with pulmonary hypertension (PH) due to chronic lung disease (Group 3 PH) have poor long-term outcomes. However, predictors of survival in Group 3 PH are not well described.
Methods: We performed a cohort study of Group 3 PH patients (n = 143; mean age 65 ± 12 years, 52% female) evaluated at the University of Minnesota. The Kaplan-Meier method and Cox regression analysis were used to assess survival and predictors of mortality, respectively. The clinical characteristics and survival were compared in patients categorized by PH severity based on the World Health Organization (WHO) classification and lung disease etiology.
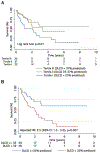
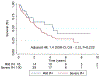
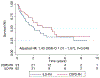
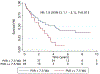
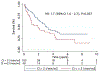
Results: After a median follow-up of 1.4 years, there were 69 (48%) deaths. The 1-, 3-, and 5-year survival rates were 79%, 48%, and 31%. Age, coronary artery disease, atrial fibrillation, Charlson comorbidity index, serum N-terminal pro‒brain natriuretic peptide (NT-proBNP), creatinine, diffusion capacity of carbon monoxide (DLCO), total lung capacity, left ventricular ejection fraction, right atrial and right ventricular enlargement on echocardiography, cardiac index, and pulmonary vascular resistance (PVR) were univariate predictors of survival. On multivariable analysis, DLCO was the only predictor of mortality (adjusted hazard ratio [HR] for every 10% decrease in predicted value: 1.31 [95% confidence interval 1.12 to 1.47]; p = 0.003). The 1-/5-year survival by tertiles of DLCO was 84%/56%, 82%/44%, and 63%/14% (p = 0.01), respectively. On receiver-operating characteristic curve analysis, DLCO <32% of predicted had the highest sensitivity and specificity for predicting survival. The 1- and 5-year survival in patients with a DLCO ≥32% predicted was 84% and 60% vs 68% and 13% in patients with a DLCO <32% predicted (adjusted HR: 2.5 [95% confidence interval 1.3 to 5.0]; p = 0.007). Lung volumes and DLCO were not related, but higher PVR was strongly associated with reduced DLCO. There was increased mortality in interstitial lung disease‒PH as compared with chronic obstructive pulmonary disease‒PH, but PH severity based on the WHO classification did not alter survival.
Conclusions: Low DLCO is a predictor of mortality and should be used to risk-stratify Group 3 PH patients.
Keywords: COPD; Cor pulmonale; Emphysema; Interstitial lung disease; pulmonary function test; right ventricle.
Copyright © 2018 Elsevier Ltd. All rights reserved.
Figures
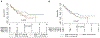
Comment in
-
Diffusion capacity of the lung-a disease biomarker linking ventilation and circulation.J Heart Lung Transplant. 2019 Feb;38(2):130-132. doi: 10.1016/j.healun.2018.11.008. Epub 2018 Dec 1. J Heart Lung Transplant. 2019. PMID: 30691594 No abstract available.
References
-
- Barberà JA, Blanco I. Gaining insights into pulmonary hypertension in respiratory diseases. Eur Respir J 2015;46:1247–50. - PubMed
-
- Gall H, Felix JF, Schneck FK, et al. The Giessen Pulmonary Hypertension Registry: survival in pulmonary hypertension subgroups. J Heart Lung Transplant 2017;36:957–67. - PubMed
Publication types
MeSH terms
Substances
Grants and funding
LinkOut - more resources
Full Text Sources
Medical
Research Materials

