Mitochondrial transplantation prolongs cold ischemia time in murine heart transplantation
- PMID: 30391192
- PMCID: PMC6574228
- DOI: 10.1016/j.healun.2018.09.025
Mitochondrial transplantation prolongs cold ischemia time in murine heart transplantation
Abstract
Background: Cold ischemia time (CIT) causes ischemia‒reperfusion injury to the mitochondria and detrimentally effects myocardial function and tissue viability. Mitochondrial transplantation replaces damaged mitochondria and enhances myocardial function and tissue viability. Herein we investigated the efficacy of mitochondrial transplantation in enhancing graft function and viability after prolonged CIT.
Methods: Heterotopic heart transplantation was performed in C57BL/6J mice. Upon heart harvesting from C57BL/6J donors, 0.5 ml of either mitochondria (1 × 108 in respiration buffer; mitochondria group) or respiration buffer (vehicle group) was delivered antegrade to the coronary arteries via injection to the coronary ostium. The hearts were excised and preserved for 29 ± 0.3 hours in cold saline (4°C). The hearts were then heterotopically transplanted. A second injection of either mitochondria (1 × 108) or respiration buffer (vehicle) was delivered antegrade to the coronary arteries 5 minutes after transplantation. Grafts were analyzed for 24 hours. Beating score, graft function, and tissue injury were measured.
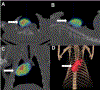
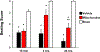
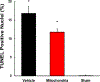
Results: Beating score, calculated ejection fraction, and shortening fraction were significantly enhanced (p < 0.05), whereas necrosis and neutrophil infiltration were significantly decreased (p < 0.05) in the mitochondria group as compared with the vehicle group at 24 hours of reperfusion. Transmission electron microscopy showed the presence of contraction bands in vehicle but not in mitochondria grafts.
Conclusions: Mitochondrial transplantation prolongs CIT to 29 hours in the murine heart transplantation model, significantly enhances graft function, and decreases graft tissue injury. Mitochondrial transplantation may provide a means to reduce graft failure and improve transplantation outcomes after prolonged CIT.
Keywords: cold ischemia time; heart transplantation; ischemia–reperfusion; mitochondria; mitochondrial transplantation.
Copyright © 2018 Elsevier Ltd. All rights reserved.
Conflict of interest statement
Conflict of Interest statement
Dr. McCully, Dr. Cowan and Dr. del Nido have patents pending for the isolation and usage of mitochondria. There are no other conflicts of interest by any of the authors. The authors attest they had full freedom to explore the data, analyze the results independent from any sponsor and that they had sole authority to make the final decision to submit the material for publication.
Figures
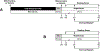
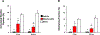

Comment in
-
Organ(elle) Transplants.Am J Transplant. 2018 Dec;18(12):2839-2840. doi: 10.1111/ajt.15157. Am J Transplant. 2018. PMID: 30476365 No abstract available.
Similar articles
-
The mitochondria-targeted anti-oxidant MitoQ decreases ischemia-reperfusion injury in a murine syngeneic heart transplant model.J Heart Lung Transplant. 2015 Nov;34(11):1471-80. doi: 10.1016/j.healun.2015.05.007. Epub 2015 Jun 11. J Heart Lung Transplant. 2015. PMID: 26140808 Free PMC article.
-
Reduction of cold ischemia-reperfusion injury by graft-expressing clusterin in heart transplantation.J Heart Lung Transplant. 2011 Jul;30(7):819-26. doi: 10.1016/j.healun.2011.03.007. Epub 2011 Apr 22. J Heart Lung Transplant. 2011. PMID: 21515078
-
Supplementing preservation solution with mitochondria-targeted H2 S donor AP39 protects cardiac grafts from prolonged cold ischemia-reperfusion injury in heart transplantation.Am J Transplant. 2019 Nov;19(11):3139-3148. doi: 10.1111/ajt.15539. Epub 2019 Sep 3. Am J Transplant. 2019. PMID: 31338943
-
Mitochondrial Transplantation in Myocardial Ischemia and Reperfusion Injury.Adv Exp Med Biol. 2017;982:595-619. doi: 10.1007/978-3-319-55330-6_31. Adv Exp Med Biol. 2017. PMID: 28551809 Review.
-
The Critical Role of Bioenergetics in Donor Cardiac Allograft Preservation.J Cardiovasc Transl Res. 2016 Jun;9(3):176-183. doi: 10.1007/s12265-016-9692-2. Epub 2016 May 10. J Cardiovasc Transl Res. 2016. PMID: 27164961 Review.
Cited by
-
Effect of Parecoxib Sodium on Myocardial Ischemia-Reperfusion Injury Rats.Med Sci Monit. 2021 Jan 4;27:e928205. doi: 10.12659/MSM.928205. Med Sci Monit. 2021. PMID: 33395402 Free PMC article.
-
Recent advances in mitochondrial transplantation to treat disease.Biomater Transl. 2025 Mar 25;6(1):4-23. doi: 10.12336/biomatertransl.2025.01.002. eCollection 2025. Biomater Transl. 2025. PMID: 40313574 Free PMC article. Review.
-
Hurdles to Cardioprotection in the Critically Ill.Int J Mol Sci. 2019 Aug 5;20(15):3823. doi: 10.3390/ijms20153823. Int J Mol Sci. 2019. PMID: 31387264 Free PMC article. Review.
-
Bases for Treating Skin Aging With Artificial Mitochondrial Transfer/Transplant (AMT/T).Front Bioeng Biotechnol. 2020 Aug 13;8:919. doi: 10.3389/fbioe.2020.00919. eCollection 2020. Front Bioeng Biotechnol. 2020. PMID: 32903493 Free PMC article.
-
Mitochondrial transplantation enhances murine lung viability and recovery after ischemia-reperfusion injury.Am J Physiol Lung Cell Mol Physiol. 2020 Jan 1;318(1):L78-L88. doi: 10.1152/ajplung.00221.2019. Epub 2019 Nov 6. Am J Physiol Lung Cell Mol Physiol. 2020. PMID: 31693391 Free PMC article.
References
-
- Colvin M, Smith JM, Hadley N, et al. OPTN/SRTR 2016 Annual Data Report: Heart. Am J Transplant 2018;18(Suppl 1):291–362. - PubMed
-
- Subramaniam K Early graft failure after heart transplantation: prevention and treatment. Int Anesthesiol Clin 2012;50:202–227. - PubMed
-
- Lund LH, Khush KK, Cherikh WS, et al. International Society for Heart and Lung Transplantation. The Registry of the International Society for Heart and Lung Transplantation: Thirty-fourth Adult Heart Transplantation Report-2017; Focus Theme: Allograft ischemic time. J Heart Lung Transplant 2017;36:1037–1046. - PubMed
-
- Weiss ES, Allen JG, Kilic A, et al. Development of a quantitative donor risk index to predict short-term mortality in orthotopic heart transplantation. J Heart Lung Transplant 2012;31:266–273. - PubMed
Publication types
MeSH terms
Grants and funding
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical

