Cranioplasty Using Autologous Bone versus Porous Polyethylene versus Custom-Made Titanium Mesh : A Retrospective Review of 108 Patients
- PMID: 30396247
- PMCID: PMC6280051
- DOI: 10.3340/jkns.2018.0047
Cranioplasty Using Autologous Bone versus Porous Polyethylene versus Custom-Made Titanium Mesh : A Retrospective Review of 108 Patients
Abstract
Objective: The purpose of this study was to compare the cosmetic outcome and complications after cranioplasty (CP) due to three different implant materials, and analyze the mean implant survival and cumulative survival rate based on these results.
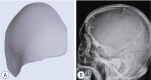
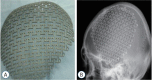
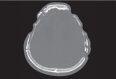
Methods: We reviewed 108 patients retrospectively who underwent CP between January 2014 and November 2016. Autologous bone (AB; 45 patients) and synthetic materials with porous polyethylene (PP; 32 patients) and custom-made 3-dimensional printed titanium mesh (CT; 31 patients) were used as implants.
Results: Regardless of implanted materials, more than 89.8% of the CP patients were satisfied with the cosmetic outcome. No statistically significant difference was observed among the three groups. The overall postoperative complication rates of each group were 31.1% in the AB group, 15.6% in the PP group and 3.2% in the CT group. The CT group showed lower complication rates compared with AB and PP groups (χ2-test : AB vs. PP, p=0.34; AB vs. CT, p=0.00; PP vs. CT, p=0.03). The AB and PP groups demonstrated a higher post-CP infection rate (11.1% and 6.3%) than the CT group (3.2%). However, no significant difference in the incidence of post-CP infection was observed among the three groups. The PP and CT groups demonstrated a higher mean implant survival time and cumulative survival rate than the AB group at the last follow-up (p<0.05).
Conclusion: In comparison with AB and PP, cranioplasty with CT shows benefits in terms of lower post-CP complication, less intraoperative bleeding loss, shorter operation time and in-hospital stay. The PP and CT groups showed higher implant survival time and cumulative survival rate compared with the AB group.
Keywords: Bone resorption; Infection; Reconstructive surgical procedure; Titanium.
Conflict of interest statement
No potential conflict of interest relevant to this article was reported.
Figures

References
-
- Agrawal D, Hussain N. Decompressive craniectomy in cerebral toxoplasmosis. Eur J Clin Microbiol Infect Dis. 2005;24:772–773. - PubMed
-
- Archavlis E, Carvi Y Nievas M. The impact of timing of cranioplasty in patients with large cranial defects after decompressive hemicraniectomy. Acta Neurochir (Wien) 2012;154:1055–1062. - PubMed
-
- Beauchamp KM, Kashuk J, Moore EE, Bolles G, Rabb C, Seinfeld J, et al. Cranioplasty after postinjury decompressive craniectomy: is timing of the essence? J Trauma. 2010;69:270–274. - PubMed
-
- Bruce JN, Bruce SS. Preservation of bone flaps in patients with postcraniotomy infections. J Neurosurg. 2003;98:1203–1207. - PubMed
-
- Cabraja M, Klein M, Lehmann TN. Long-term results following titanium cranioplasty of large skull defects. Neurosurg Focus. 2009;26:E10. - PubMed
LinkOut - more resources
Full Text Sources
Miscellaneous

